AIDS on:
[Wikipedia]
[Google]
[Amazon]
Human immunodeficiency virus infection and acquired immunodeficiency syndrome (HIV/AIDS) is a spectrum of conditions caused by
 The initial period following the contraction of HIV is called acute HIV, primary HIV or acute retroviral syndrome. Many individuals develop an influenza-like illness or a mononucleosis-like illness 2–4 weeks after exposure while others have no significant symptoms. Symptoms occur in 40–90% of cases and most commonly include
The initial period following the contraction of HIV is called acute HIV, primary HIV or acute retroviral syndrome. Many individuals develop an influenza-like illness or a mononucleosis-like illness 2–4 weeks after exposure while others have no significant symptoms. Symptoms occur in 40–90% of cases and most commonly include
 Acquired immunodeficiency syndrome (AIDS) is defined as an HIV infection with either a CD4+ T cell count below 200 cells per µL or the occurrence of specific diseases associated with HIV infection. In the absence of specific treatment, around half of people infected with HIV develop AIDS within ten years. The most common initial conditions that alert to the presence of AIDS are
Acquired immunodeficiency syndrome (AIDS) is defined as an HIV infection with either a CD4+ T cell count below 200 cells per µL or the occurrence of specific diseases associated with HIV infection. In the absence of specific treatment, around half of people infected with HIV develop AIDS within ten years. The most common initial conditions that alert to the presence of AIDS are
 The second-most frequent mode of HIV transmission is via blood and blood products. Blood-borne transmission can be through needle-sharing during intravenous drug use, needle-stick injury, transfusion of contaminated blood or blood product, or medical injections with unsterilized equipment. The risk from sharing a needle during drug injection is between 0.63% and 2.4% per act, with an average of 0.8%. The risk of acquiring HIV from a needle stick from an HIV-infected person is estimated as 0.3% (about 1 in 333) per act and the risk following mucous membrane exposure to infected blood as 0.09% (about 1 in 1000) per act. This risk may, however, be up to 5% if the introduced blood was from a person with a high viral load and the cut was deep. In the United States, intravenous drug users made up 12% of all new cases of HIV in 2009, and in some areas more than 80% of people who inject drugs are HIV-positive.
HIV is transmitted in about 90% of
The second-most frequent mode of HIV transmission is via blood and blood products. Blood-borne transmission can be through needle-sharing during intravenous drug use, needle-stick injury, transfusion of contaminated blood or blood product, or medical injections with unsterilized equipment. The risk from sharing a needle during drug injection is between 0.63% and 2.4% per act, with an average of 0.8%. The risk of acquiring HIV from a needle stick from an HIV-infected person is estimated as 0.3% (about 1 in 333) per act and the risk following mucous membrane exposure to infected blood as 0.09% (about 1 in 1000) per act. This risk may, however, be up to 5% if the introduced blood was from a person with a high viral load and the cut was deep. In the United States, intravenous drug users made up 12% of all new cases of HIV in 2009, and in some areas more than 80% of people who inject drugs are HIV-positive.
HIV is transmitted in about 90% of

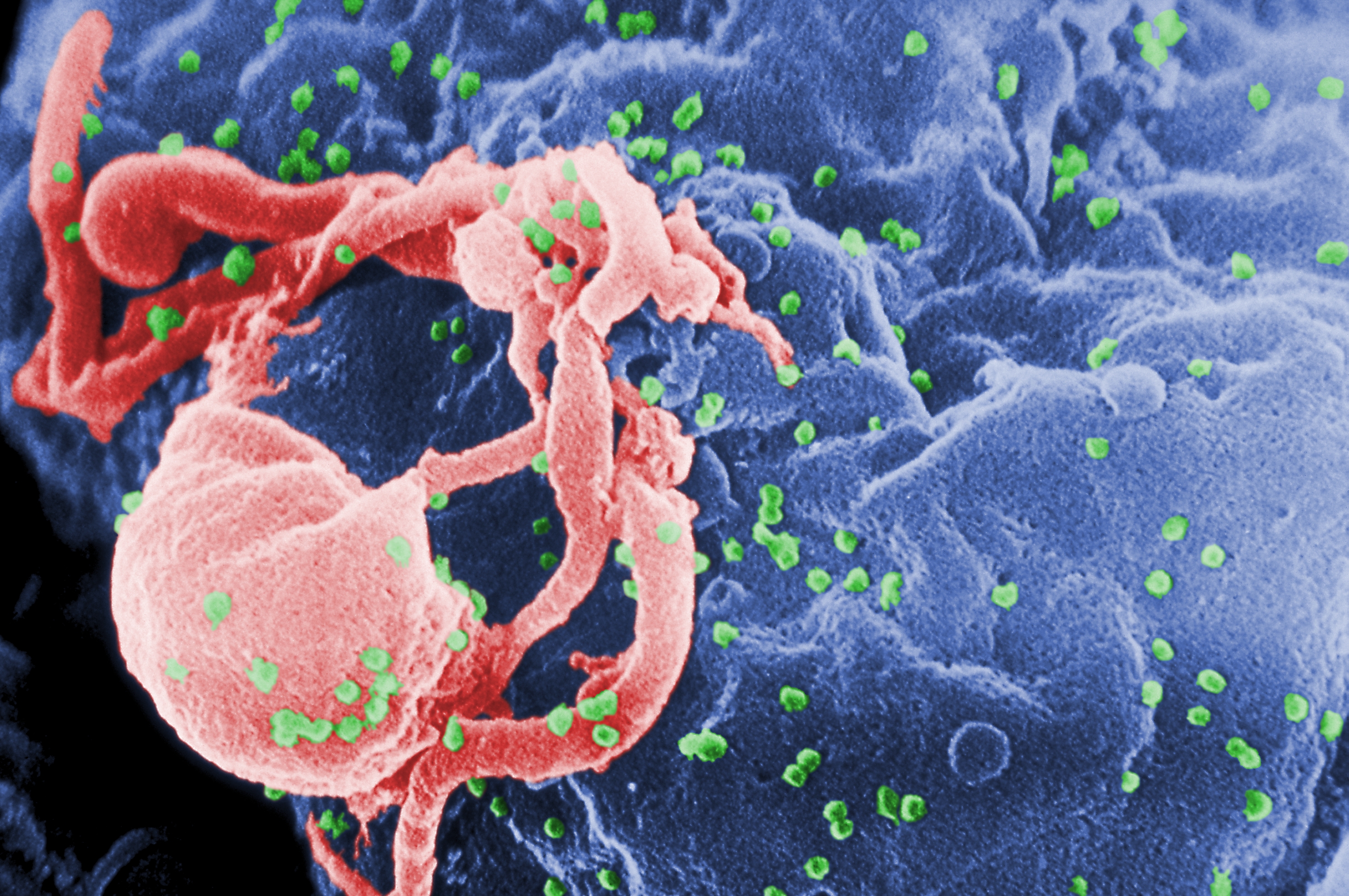 HIV is the cause of the spectrum of disease known as HIV/AIDS. HIV is a
HIV is the cause of the spectrum of disease known as HIV/AIDS. HIV is a
 HIV/AIDS is diagnosed via laboratory testing and then staged based on the presence of certain signs or symptoms. HIV screening is recommended by the United States Preventive Services Task Force for all people 15 years to 65 years of age, including all pregnant women. Additionally, testing is recommended for those at high risk, which includes anyone diagnosed with a sexually transmitted illness. In many areas of the world, a third of HIV carriers only discover they are infected at an advanced stage of the disease when AIDS or severe immunodeficiency has become apparent.
HIV/AIDS is diagnosed via laboratory testing and then staged based on the presence of certain signs or symptoms. HIV screening is recommended by the United States Preventive Services Task Force for all people 15 years to 65 years of age, including all pregnant women. Additionally, testing is recommended for those at high risk, which includes anyone diagnosed with a sexually transmitted illness. In many areas of the world, a third of HIV carriers only discover they are infected at an advanced stage of the disease when AIDS or severe immunodeficiency has become apparent.

 Most people infected with HIV develop specific
Most people infected with HIV develop specific

 Consistent
Consistent
 Current HAART options are combinations (or "cocktails") consisting of at least three medications belonging to at least two types, or "classes", of antiretroviral agents. Initially, treatment is typically a non-nucleoside reverse transcriptase inhibitor (NNRTI) plus two nucleoside analog reverse transcriptase inhibitors (NRTIs). Typical NRTIs include: zidovudine (AZT) or tenofovir (TDF) and lamivudine (3TC) or emtricitabine (FTC). , dolutegravir/lamivudine/tenofovir is listed by the
Current HAART options are combinations (or "cocktails") consisting of at least three medications belonging to at least two types, or "classes", of antiretroviral agents. Initially, treatment is typically a non-nucleoside reverse transcriptase inhibitor (NNRTI) plus two nucleoside analog reverse transcriptase inhibitors (NRTIs). Typical NRTIs include: zidovudine (AZT) or tenofovir (TDF) and lamivudine (3TC) or emtricitabine (FTC). , dolutegravir/lamivudine/tenofovir is listed by the
 HIV/AIDS has become a chronic rather than an acutely fatal disease in many areas of the world. Prognosis varies between people, and both the CD4 count and viral load are useful for predicted outcomes. Without treatment, average survival time after infection with HIV is estimated to be 9 to 11 years, depending on the HIV subtype. After the diagnosis of AIDS, if treatment is not available, survival ranges between 6 and 19 months. HAART and appropriate prevention of opportunistic infections reduces the death rate by 80%, and raises the life expectancy for a newly diagnosed young adult to 20–50 years. This is between two thirds and nearly that of the general population. If treatment is started late in the infection, prognosis is not as good: for example, if treatment is begun following the diagnosis of AIDS, life expectancy is ~10–40 years. Half of infants born with HIV die before two years of age without treatment.
HIV/AIDS has become a chronic rather than an acutely fatal disease in many areas of the world. Prognosis varies between people, and both the CD4 count and viral load are useful for predicted outcomes. Without treatment, average survival time after infection with HIV is estimated to be 9 to 11 years, depending on the HIV subtype. After the diagnosis of AIDS, if treatment is not available, survival ranges between 6 and 19 months. HAART and appropriate prevention of opportunistic infections reduces the death rate by 80%, and raises the life expectancy for a newly diagnosed young adult to 20–50 years. This is between two thirds and nearly that of the general population. If treatment is started late in the infection, prognosis is not as good: for example, if treatment is begun following the diagnosis of AIDS, life expectancy is ~10–40 years. Half of infants born with HIV die before two years of age without treatment.
 The primary causes of death from HIV/AIDS are opportunistic infections and
The primary causes of death from HIV/AIDS are opportunistic infections and
 Some authors consider HIV/AIDS a global
Some authors consider HIV/AIDS a global
 The first news story on the disease appeared on May 18, 1981, in the gay newspaper '' New York Native''. AIDS was first clinically reported on June 5, 1981, with five cases in the United States. The initial cases were a cluster of injecting drug users and gay men with no known cause of impaired immunity who showed symptoms of '' Pneumocystis carinii'' pneumonia (PCP), a rare opportunistic infection that was known to occur in people with very compromised immune systems. Soon thereafter, a large number of homosexual men developed a generally rare skin cancer called Kaposi's sarcoma (KS). Many more cases of PCP and KS emerged, alerting U.S. Centers for Disease Control and Prevention (CDC) and a CDC task force was formed to monitor the outbreak.
In the early days, the CDC did not have an official name for the disease, often referring to it by way of diseases associated with it, such as lymphadenopathy, the disease after which the discoverers of HIV originally named the virus. They also used ''Kaposi's sarcoma and opportunistic infections'', the name by which a task force had been set up in 1981. At one point the CDC referred to it as the "4H disease", as the syndrome seemed to affect heroin users, homosexuals,
The first news story on the disease appeared on May 18, 1981, in the gay newspaper '' New York Native''. AIDS was first clinically reported on June 5, 1981, with five cases in the United States. The initial cases were a cluster of injecting drug users and gay men with no known cause of impaired immunity who showed symptoms of '' Pneumocystis carinii'' pneumonia (PCP), a rare opportunistic infection that was known to occur in people with very compromised immune systems. Soon thereafter, a large number of homosexual men developed a generally rare skin cancer called Kaposi's sarcoma (KS). Many more cases of PCP and KS emerged, alerting U.S. Centers for Disease Control and Prevention (CDC) and a CDC task force was formed to monitor the outbreak.
In the early days, the CDC did not have an official name for the disease, often referring to it by way of diseases associated with it, such as lymphadenopathy, the disease after which the discoverers of HIV originally named the virus. They also used ''Kaposi's sarcoma and opportunistic infections'', the name by which a task force had been set up in 1981. At one point the CDC referred to it as the "4H disease", as the syndrome seemed to affect heroin users, homosexuals,
 The origin of HIV / AIDS and the circumstances that led to its emergence remain unsolved.
Both HIV-1 and HIV-2 are believed to have originated in non-human
The origin of HIV / AIDS and the circumstances that led to its emergence remain unsolved.
Both HIV-1 and HIV-2 are believed to have originated in non-human
 AIDS stigma exists around the world in a variety of ways, including ostracism, rejection, discrimination and avoidance of HIV-infected people; compulsory HIV testing without prior consent or protection of confidentiality; violence against HIV-infected individuals or people who are perceived to be infected with HIV; and the
AIDS stigma exists around the world in a variety of ways, including ostracism, rejection, discrimination and avoidance of HIV-infected people; compulsory HIV testing without prior consent or protection of confidentiality; violence against HIV-infected individuals or people who are perceived to be infected with HIV; and the
 HIV/AIDS affects the economics of both individuals and countries. The
HIV/AIDS affects the economics of both individuals and countries. The
UNAIDS
– Joint United Nations Program on HIV/AIDS
HIVinfo
– Information on HIV/AIDS treatment, prevention, and research, U.S. Department of Health and Human Services
2018 Recommendations of the International Antiviral Society
{{DEFAULTSORT:HIV AIDS 1981 in biology Articles containing video clips Health disasters Pandemics Slow virus diseases
infection
An infection is the invasion of tissues by pathogens, their multiplication, and the reaction of host tissues to the infectious agent and the toxins they produce. An infectious disease, also known as a transmissible disease or communicable di ...
with the human immunodeficiency virus (HIV), a retrovirus
A retrovirus is a type of virus that inserts a DNA copy of its RNA genome into the DNA of a host cell that it invades, thus changing the genome of that cell. Once inside the host cell's cytoplasm, the virus uses its own reverse transcriptas ...
. Following initial infection an individual may not notice any symptoms, or may experience a brief period of influenza-like illness. Typically, this is followed by a prolonged incubation period with no symptoms. If the infection progresses, it interferes more with the immune system
The immune system is a network of biological processes that protects an organism from diseases. It detects and responds to a wide variety of pathogens, from viruses to parasitic worms, as well as cancer cells and objects such as wood splinte ...
, increasing the risk of developing common infections such as tuberculosis
Tuberculosis (TB) is an infectious disease usually caused by '' Mycobacterium tuberculosis'' (MTB) bacteria. Tuberculosis generally affects the lungs, but it can also affect other parts of the body. Most infections show no symptoms, ...
, as well as other opportunistic infection
An opportunistic infection is an infection caused by pathogens (bacteria, fungi, parasites or viruses) that take advantage of an opportunity not normally available. These opportunities can stem from a variety of sources, such as a weakened immun ...
s, and tumors which are rare in people who have normal immune function. These late symptoms of infection are referred to as acquired immunodeficiency syndrome (AIDS). This stage is often also associated with unintended weight loss.
HIV is spread primarily by unprotected sex (including anal and vaginal sex), contaminated blood transfusion
Blood transfusion is the process of transferring blood products into a person's circulation intravenously. Transfusions are used for various medical conditions to replace lost components of the blood. Early transfusions used whole blood, but mo ...
s, hypodermic needle
A hypodermic needle (from Greek ὑπο- (''hypo-'' = under), and δέρμα (''derma'' = skin)), one of a category of medical tools which enter the skin, called sharps, is a very thin, hollow tube with one sharp tip. It is commonly used ...
s, and from mother to child during pregnancy
Pregnancy is the time during which one or more offspring develops ( gestates) inside a woman's uterus (womb). A multiple pregnancy involves more than one offspring, such as with twins.
Pregnancy usually occurs by sexual intercourse, but ...
, delivery, or breastfeeding. Some bodily fluids, such as saliva, sweat and tears, do not transmit the virus. Oral sex has little to no risk of transmitting the virus. Methods of prevention include safe sex, needle exchange program
A needle and syringe programme (NSP), also known as needle exchange program (NEP), is a social service that allows injecting drug users (IDUs) to obtain clean and unused hypodermic needles and associated paraphernalia at little or no cost. It ...
s, treating those who are infected, as well as both pre- and post-exposure prophylaxis. Disease in a baby can often be prevented by giving both the mother and child antiretroviral medication.
HIV/AIDS has had a large impact on society, both as an illness and as a source of discrimination
Discrimination is the act of making unjustified distinctions between people based on the groups, classes, or other categories to which they belong or are perceived to belong. People may be discriminated on the basis of Racial discrimination, r ...
. The disease also has large economic impacts. There are many misconceptions about HIV/AIDS, such as the belief that it can be transmitted by casual non-sexual contact. The disease has become subject to many controversies involving religion, including the Catholic Church's position not to support condom
A condom is a sheath-shaped Barrier contraception, barrier device used during sexual intercourse to reduce the probability of pregnancy or a Sexually transmitted disease, sexually transmitted infection (STI). There are both male and female con ...
use as prevention. It has attracted international medical and political attention as well as large-scale funding since it was identified in the 1980s.
HIV made the jump from other primates to humans in west-central Africa in the early-to-mid 20th century. AIDS was first recognized by the U.S. Centers for Disease Control and Prevention
The Centers for Disease Control and Prevention (CDC) is the national public health agency of the United States. It is a United States federal agency, under the Department of Health and Human Services, and is headquartered in Atlanta, Georg ...
(CDC) in 1981 and its cause—HIV infection—was identified in the early part of the decade. Since when AIDS was identified and as of 2021, the disease has caused an estimated 40 million deaths worldwide. In 2021, there were 650,000 deaths and about 38 million people worldwide living with HIV. An estimated 20.6 million of these people live in eastern and southern Africa. HIV/AIDS is considered a pandemic
A pandemic () is an epidemic of an infectious disease that has spread across a large region, for instance multiple continents or worldwide, affecting a substantial number of individuals. A widespread endemic disease with a stable number of in ...
—a disease outbreak which is present over a large area and is actively spreading.(subscription required)
The United States' National Institutes of Health (NIH) and the Gates Foundation have pledged $200 million focused on developing a global cure for AIDS. While there is no broadly available cure or vaccine
A vaccine is a biological preparation that provides active acquired immunity to a particular infectious or malignant disease. The safety and effectiveness of vaccines has been widely studied and verified.
, antiretroviral treatment can slow the course of the disease and may lead to a near-normal life expectancy. Treatment is recommended as soon as the diagnosis is made. Without treatment, the average survival time after infection is 11 years. Two individuals have been reported cured of AIDS, known as the Berlin Patient and the London Patient
Adam Castillejo, also known as "The London Patient", is the second person known to have been cured of HIV infection.
His body became resistant to HIV infection after receiving a bone marrow transplant to treat Hodgkin's lymphoma. The donor carri ...
.
Signs and symptoms
There are three main stages of HIV infection: acute infection, clinical latency, and AIDS.Mandell, Bennett, and Dolan (2010). Chapter 121.Acute infection
fever
Fever, also referred to as pyrexia, is defined as having a temperature above the normal range due to an increase in the body's temperature set point. There is not a single agreed-upon upper limit for normal temperature with sources using val ...
, large tender lymph nodes, throat inflammation, a rash
A rash is a change of the human skin which affects its color, appearance, or texture.
A rash may be localized in one part of the body, or affect all the skin. Rashes may cause the skin to change color, itch, become warm, bumpy, chapped, dry, c ...
, headache, tiredness, and/or sores of the mouth and genitals. The rash, which occurs in 20–50% of cases, presents itself on the trunk and is maculopapular, classically. Some people also develop opportunistic infections at this stage. Gastrointestinal symptoms, such as vomiting or diarrhea
Diarrhea, also spelled diarrhoea, is the condition of having at least three loose, liquid, or watery bowel movements each day. It often lasts for a few days and can result in dehydration due to fluid loss. Signs of dehydration often begin w ...
may occur. Neurological symptoms of peripheral neuropathy or Guillain–Barré syndrome also occur. The duration of the symptoms varies, but is usually one or two weeks.
Owing to their nonspecific character, these symptoms are not often recognized as signs of HIV infection. Even cases that do get seen by a family doctor or a hospital are often misdiagnosed as one of the many common infectious disease
An infection is the invasion of tissues by pathogens, their multiplication, and the reaction of host tissues to the infectious agent and the toxins they produce. An infectious disease, also known as a transmissible disease or communicable di ...
s with overlapping symptoms. Thus, it is recommended that HIV be considered in people presenting with an unexplained fever who may have risk factors for the infection.Mandell, Bennett, and Dolan (2010). Chapter 118.
Clinical latency
The initial symptoms are followed by a stage called clinical latency, asymptomatic HIV, or chronic HIV. Without treatment, this second stage of the natural history of HIV infection can last from about three years to over 20 years (on average, about eight years). While typically there are few or no symptoms at first, near the end of this stage many people experience fever, weight loss, gastrointestinal problems and muscle pains. Between 50% and 70% of people also developpersistent generalized lymphadenopathy
Persistent generalized lymphadenopathy (PGL) is enlarged, painless, non-tender lymph nodes occurring in a couple of different areas for more than three to six months for which no other reason can be found. To expand, the common site where PGL occur ...
, characterized by unexplained, non-painful enlargement of more than one group of lymph nodes (other than in the groin) for over three to six months.
Although most HIV-1 infected individuals have a detectable viral load and in the absence of treatment will eventually progress to AIDS, a small proportion (about 5%) retain high levels of CD4
In molecular biology, CD4 (cluster of differentiation 4) is a glycoprotein that serves as a co-receptor for the T-cell receptor (TCR). CD4 is found on the surface of immune cells such as T helper cells, monocytes, macrophages, and dendritic ce ...
+ T cells (T helper cell
The T helper cells (Th cells), also known as CD4+ cells or CD4-positive cells, are a type of T cell that play an important role in the adaptive immune system. They aid the activity of other immune cells by releasing cytokines. They are consider ...
s) without antiretroviral therapy for more than five years. These individuals are classified as "HIV controllers" or long-term nonprogressors
Long-term nonprogressors (LTNPs), sometimes also called elite controllers, are individuals infected with HIV, who maintain a CD4 count greater than 500 without antiretroviral therapy with a detectable viral load. Many of these patients have been H ...
(LTNP). Another group consists of those who maintain a low or undetectable viral load without anti-retroviral treatment, known as "elite controllers" or "elite suppressors". They represent approximately 1 in 300 infected persons.
Acquired immunodeficiency syndrome
pneumocystis pneumonia
''Pneumocystis'' pneumonia (PCP), also known as ''Pneumocystis jirovecii'' pneumonia (PJP), is a form of pneumonia that is caused by the yeast-like fungus ''Pneumocystis jirovecii''.
''Pneumocystis'' specimens are commonly found in the lungs of ...
(40%), cachexia
Cachexia () is a complex syndrome associated with an underlying illness, causing ongoing muscle loss that is not entirely reversed with nutritional supplementation. A range of diseases can cause cachexia, most commonly cancer, congestive heart fa ...
in the form of HIV wasting syndrome (20%), and esophageal candidiasis. Other common signs include recurrent respiratory tract infections.
Opportunistic infections may be caused by bacteria
Bacteria (; singular: bacterium) are ubiquitous, mostly free-living organisms often consisting of one biological cell. They constitute a large domain of prokaryotic microorganisms. Typically a few micrometres in length, bacteria were am ...
, virus
A virus is a submicroscopic infectious agent that replicates only inside the living cells of an organism. Viruses infect all life forms, from animals and plants to microorganisms, including bacteria and archaea.
Since Dmitri Ivanovsk ...
es, fungi
A fungus ( : fungi or funguses) is any member of the group of eukaryotic organisms that includes microorganisms such as yeasts and molds, as well as the more familiar mushrooms. These organisms are classified as a kingdom, separately fr ...
, and parasite
Parasitism is a close relationship between species, where one organism, the parasite, lives on or inside another organism, the host, causing it some harm, and is adapted structurally to this way of life. The entomologist E. O. Wilson h ...
s that are normally controlled by the immune system. Which infections occur depends partly on what organisms are common in the person's environment. These infections may affect nearly every organ system.
People with AIDS have an increased risk of developing various viral-induced cancers, including Kaposi's sarcoma, Burkitt's lymphoma
Burkitt lymphoma is a cancer of the lymphatic system, particularly B lymphocytes found in the germinal center. It is named after Denis Parsons Burkitt, the Irish surgeon who first described the disease in 1958 while working in equatorial Africa. ...
, primary central nervous system lymphoma
Primary central nervous system lymphoma (PCNSL), also termed primary diffuse large B-cell lymphoma of the central nervous system (DLBCL-CNS), is a primary intracranial tumor appearing mostly in patients with severe immunodeficiency (typically pat ...
, and cervical cancer
Cervical cancer is a cancer arising from the cervix. It is due to the abnormal growth of cells that have the ability to invade or spread to other parts of the body. Early on, typically no symptoms are seen. Later symptoms may include abnormal ...
. Kaposi's sarcoma is the most common cancer, occurring in 10% to 20% of people with HIV.Mandell, Bennett, and Dolan (2010). Chapter 169. The second-most common cancer is lymphoma, which is the cause of death of nearly 16% of people with AIDS and is the initial sign of AIDS in 3% to 4%. Both these cancers are associated with human herpesvirus 8 (HHV-8). Cervical cancer occurs more frequently in those with AIDS because of its association with human papillomavirus
Human papillomavirus infection (HPV infection) is caused by a DNA virus from the '' Papillomaviridae'' family. Many HPV infections cause no symptoms and 90% resolve spontaneously within two years. In some cases, an HPV infection persists and r ...
(HPV). Conjunctival cancer (of the layer that lines the inner part of eyelids and the white part of the eye) is also more common in those with HIV.
Additionally, people with AIDS frequently have systemic symptoms such as prolonged fevers, sweats (particularly at night), swollen lymph nodes, chills, weakness, and unintended weight loss. Diarrhea is another common symptom, present in about 90% of people with AIDS. They can also be affected by diverse psychiatric and neurological symptoms independent of opportunistic infections and cancers.
Transmission
HIV is spread by three main routes:sexual contact
Human sexual activity, human sexual practice or human sexual behaviour is the manner in which humans experience and express their sexuality. People engage in a variety of sexual acts, ranging from activities done alone (e.g., masturbation) t ...
, significant exposure to infected body fluids or tissues, and from mother to child during pregnancy, delivery, or breastfeeding (known as vertical transmission). There is no risk of acquiring HIV if exposed to feces
Feces ( or faeces), known colloquially and in slang as poo and poop, are the solid or semi-solid remains of food that was not digested in the small intestine, and has been broken down by bacteria in the large intestine. Feces contain a rela ...
, nasal secretions, saliva, sputum, sweat, tears, urine, or vomit unless these are contaminated with blood. It is also possible to be co-infected by more than one strain of HIV—a condition known as HIV superinfection.
Sexual
The most frequent mode of transmission of HIV is through sexual contact with an infected person. However, an HIV-positive person who has an undetectable viral load as a result of long-term treatment has effectively no risk of transmitting HIV sexually. The existence of functionally noncontagious HIV-positive people on antiretroviral therapy was controversially publicized in the 2008Swiss Statement
The Swiss Statement (French: ''La déclaration suisse''; known in German as ''das EKAF-Statement''), or the Swiss Consensus Statement, was an announcement published in January 2008 by the Swiss Federal Commission for AIDS/HIV (EKAF, ''Eidgenössisc ...
, and has since become accepted as medically sound.
Globally, the most common mode of HIV transmission is via sexual contacts between people of the opposite sex; however, the pattern of transmission varies among countries. , most HIV transmission in the United States occurred among men who had sex with men
Men who have sex with men (MSM) are male persons who engage in sexual activity with members of the same sex. The term was created in the 1990s by epidemiologists to study the spread of disease among all men who have sex with men, regardless of ...
(82% of new HIV diagnoses among males aged 13 and older and 70% of total new diagnoses). In the US, gay and bisexual men aged 13 to 24 accounted for an estimated 92% of new HIV diagnoses among all men in their age group and 27% of new diagnoses among all gay and bisexual men.
With regard to unprotected heterosexual contacts, estimates of the risk of HIV transmission per sexual act appear to be four to ten times higher in low-income countries than in high-income countries. In low-income countries, the risk of female-to-male transmission is estimated as 0.38% per act, and of male-to-female transmission as 0.30% per act; the equivalent estimates for high-income countries are 0.04% per act for female-to-male transmission, and 0.08% per act for male-to-female transmission. The risk of transmission from anal intercourse is especially high, estimated as 1.4–1.7% per act in both heterosexual and homosexual contacts. While the risk of transmission from oral sex is relatively low, it is still present. The risk from receiving oral sex has been described as "nearly nil"; however, a few cases have been reported. The per-act risk is estimated at 0–0.04% for receptive oral intercourse. In settings involving prostitution
Prostitution is the business or practice of engaging in Sex work, sexual activity in exchange for payment. The definition of "sexual activity" varies, and is often defined as an activity requiring physical contact (e.g., sexual intercourse, n ...
in low-income countries, risk of female-to-male transmission has been estimated as 2.4% per act, and of male-to-female transmission as 0.05% per act.
Risk of transmission increases in the presence of many sexually transmitted infections and genital ulcers. Genital ulcers appear to increase the risk approximately fivefold. Other sexually transmitted infections, such as gonorrhea, chlamydia, trichomoniasis
Trichomoniasis (trich) is an infectious disease caused by the parasite ''Trichomonas vaginalis''. About 70% of affected people do not have symptoms when infected. When symptoms occur, they typically begin 5 to 28 days after exposure. Symptoms ca ...
, and bacterial vaginosis
Bacterial vaginosis (BV) is a disease of the vagina caused by excessive growth of bacteria. Common symptoms include increased vaginal discharge that often smells like fish. The discharge is usually white or gray in color. Burning with urinati ...
, are associated with somewhat smaller increases in risk of transmission.
The viral load of an infected person is an important risk factor in both sexual and mother-to-child transmission. During the first 2.5 months of an HIV infection a person's infectiousness is twelve times higher due to the high viral load associated with acute HIV. If the person is in the late stages of infection, rates of transmission are approximately eightfold greater.
Commercial sex workers (including those in pornography) have an increased likelihood of contracting HIV. Rough sex can be a factor associated with an increased risk of transmission. Sexual assault
Sexual assault is an act in which one intentionally sexually touches another person without that person's consent, or coerces or physically forces a person to engage in a sexual act against their will. It is a form of sexual violence, which ...
is also believed to carry an increased risk of HIV transmission as condoms are rarely worn, physical trauma to the vagina or rectum is likely, and there may be a greater risk of concurrent sexually transmitted infections.
Body fluids
 The second-most frequent mode of HIV transmission is via blood and blood products. Blood-borne transmission can be through needle-sharing during intravenous drug use, needle-stick injury, transfusion of contaminated blood or blood product, or medical injections with unsterilized equipment. The risk from sharing a needle during drug injection is between 0.63% and 2.4% per act, with an average of 0.8%. The risk of acquiring HIV from a needle stick from an HIV-infected person is estimated as 0.3% (about 1 in 333) per act and the risk following mucous membrane exposure to infected blood as 0.09% (about 1 in 1000) per act. This risk may, however, be up to 5% if the introduced blood was from a person with a high viral load and the cut was deep. In the United States, intravenous drug users made up 12% of all new cases of HIV in 2009, and in some areas more than 80% of people who inject drugs are HIV-positive.
HIV is transmitted in about 90% of
The second-most frequent mode of HIV transmission is via blood and blood products. Blood-borne transmission can be through needle-sharing during intravenous drug use, needle-stick injury, transfusion of contaminated blood or blood product, or medical injections with unsterilized equipment. The risk from sharing a needle during drug injection is between 0.63% and 2.4% per act, with an average of 0.8%. The risk of acquiring HIV from a needle stick from an HIV-infected person is estimated as 0.3% (about 1 in 333) per act and the risk following mucous membrane exposure to infected blood as 0.09% (about 1 in 1000) per act. This risk may, however, be up to 5% if the introduced blood was from a person with a high viral load and the cut was deep. In the United States, intravenous drug users made up 12% of all new cases of HIV in 2009, and in some areas more than 80% of people who inject drugs are HIV-positive.
HIV is transmitted in about 90% of blood transfusion
Blood transfusion is the process of transferring blood products into a person's circulation intravenously. Transfusions are used for various medical conditions to replace lost components of the blood. Early transfusions used whole blood, but mo ...
s using infected blood. In developed countries the risk of acquiring HIV from a blood transfusion is extremely low (less than one in half a million) where improved donor selection and HIV screening
HIV tests are used to detect the presence of the human immunodeficiency virus (HIV), the virus that causes acquired immunodeficiency syndrome (AIDS), in serum, saliva, or urine. Such tests may detect antibodies, antigens, or RNA.
AIDS diagnos ...
is performed; for example, in the UK the risk is reported at one in five million and in the United States it was one in 1.5 million in 2008. In low-income countries, only half of transfusions may be appropriately screened (as of 2008),UNAIDS 2011 pg. 60–70 and it is estimated that up to 15% of HIV infections in these areas come from transfusion of infected blood and blood products, representing between 5% and 10% of global infections. It is possible to acquire HIV from organ and tissue transplantation, although this is rare because of screening
Screening may refer to:
* Screening cultures, a type a medical test that is done to find an infection
* Screening (economics), a strategy of combating adverse selection (includes sorting resumes to select employees)
* Screening (environmental), ...
.
Unsafe medical injections play a role in HIV spread in sub-Saharan Africa. In 2007, between 12% and 17% of infections in this region were attributed to medical syringe use. The World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level o ...
estimates the risk of transmission as a result of a medical injection in Africa at 1.2%. Risks are also associated with invasive procedures, assisted delivery, and dental care in this area of the world.
People giving or receiving tattoo
A tattoo is a form of body modification made by inserting tattoo ink, dyes, and/or pigments, either indelible or temporary, into the dermis layer of the skin to form a design. Tattoo artists create these designs using several tattooing ...
s, piercings
Body piercing, which is a form of body modification, is the practice of puncturing or cutting a part of the human body, creating an opening in which jewelry may be worn, or where an Implant (medicine), implant could be inserted. The word ''pier ...
, and scarification are theoretically at risk of infection but no confirmed cases have been documented. It is not possible for mosquitoes or other insects to transmit HIV.
Mother-to-child
HIV can be transmitted from mother to child during pregnancy, during delivery, or through breast milk, resulting in the baby also contracting HIV. As of 2008, vertical transmission accounted for about 90% of cases of HIV in children. In the absence of treatment, the risk of transmission before or during birth is around 20%, and in those who also breastfeed 35%. Treatment decreases this risk to less than 5%. Antiretrovirals when taken by either the mother or the baby decrease the risk of transmission in those who do breastfeed. If blood contaminates food during pre-chewing it may pose a risk of transmission. If a woman is untreated, two years of breastfeeding results in an HIV/AIDS risk in her baby of about 17%. Due to the increased risk of death without breastfeeding in many areas in the developing world, the World Health Organization recommends either exclusive breastfeeding or the provision of safe formula. All women known to be HIV-positive should be taking lifelong antiretroviral therapy.Virology
 HIV is the cause of the spectrum of disease known as HIV/AIDS. HIV is a
HIV is the cause of the spectrum of disease known as HIV/AIDS. HIV is a retrovirus
A retrovirus is a type of virus that inserts a DNA copy of its RNA genome into the DNA of a host cell that it invades, thus changing the genome of that cell. Once inside the host cell's cytoplasm, the virus uses its own reverse transcriptas ...
that primarily infects components of the human immune system
The immune system is a network of biological processes that protects an organism from diseases. It detects and responds to a wide variety of pathogens, from viruses to parasitic worms, as well as cancer cells and objects such as wood splinte ...
such as CD4+ T cells, macrophage
Macrophages (abbreviated as M φ, MΦ or MP) ( el, large eaters, from Greek ''μακρός'' (') = large, ''φαγεῖν'' (') = to eat) are a type of white blood cell of the immune system that engulfs and digests pathogens, such as cancer ce ...
s and dendritic cell
Dendritic cells (DCs) are antigen-presenting cells (also known as ''accessory cells'') of the mammalian immune system. Their main function is to process antigen material and present it on the cell surface to the T cells of the immune system. Th ...
s. It directly and indirectly destroys CD4+ T cells.
HIV is a member of the genus
Genus ( plural genera ) is a taxonomic rank used in the biological classification of living and fossil organisms as well as viruses. In the hierarchy of biological classification, genus comes above species and below family. In binomial nom ...
''Lentivirus
''Lentivirus'' is a genus of retroviruses that cause chronic and deadly diseases characterized by long incubation periods, in humans and other mammalian species. The genus includes the human immunodeficiency virus (HIV), which causes AIDS. L ...
'', part of the family '' Retroviridae''. Lentiviruses share many morphological and biological
Biology is the scientific study of life. It is a natural science with a broad scope but has several unifying themes that tie it together as a single, coherent field. For instance, all organisms are made up of cells that process hereditary in ...
characteristics. Many species of mammals are infected by lentiviruses, which are characteristically responsible for long-duration illnesses with a long incubation period. Lentiviruses are transmitted as single-stranded, positive-sense
A sense is a biological system used by an organism for sensation, the process of gathering information about the world through the detection of stimuli. (For example, in the human body, the brain which is part of the central nervous system re ...
, enveloped RNA virus
An RNA virus is a virusother than a retrovirusthat has ribonucleic acid ( RNA) as its genetic material. The nucleic acid is usually single-stranded RNA (ssRNA) but it may be double-stranded (dsRNA). Notable human diseases caused by RNA virus ...
es. Upon entry into the target cell, the viral RNA genome
In the fields of molecular biology and genetics, a genome is all the genetic information of an organism. It consists of nucleotide sequences of DNA (or RNA in RNA viruses). The nuclear genome includes protein-coding genes and non-coding ...
is converted (reverse transcribed) into double-stranded DNA by a virally encoded reverse transcriptase
A reverse transcriptase (RT) is an enzyme used to generate complementary DNA (cDNA) from an RNA template, a process termed reverse transcription. Reverse transcriptases are used by viruses such as HIV and hepatitis B to replicate their genom ...
that is transported along with the viral genome in the virus particle. The resulting viral DNA is then imported into the cell nucleus and integrated into the cellular DNA by a virally encoded integrase and host co-factors. Once integrated, the virus may become latent, allowing the virus and its host cell to avoid detection by the immune system. Alternatively, the virus may be transcribed, producing new RNA genomes and viral proteins that are packaged and released from the cell as new virus particles that begin the replication cycle anew.
HIV is now known to spread between CD4+ T cells by two parallel routes: cell-free spread and cell-to-cell spread, i.e. it employs hybrid spreading mechanisms. In the cell-free spread, virus particles bud from an infected T cell, enter the blood/extracellular fluid and then infect another T cell following a chance encounter. HIV can also disseminate by direct transmission from one cell to another by a process of cell-to-cell spread. The hybrid spreading mechanisms of HIV contribute to the virus's ongoing replication against antiretroviral therapies.
Two types of HIV have been characterized: HIV-1 and HIV-2. HIV-1 is the virus that was originally discovered (and initially referred to also as LAV or HTLV-III). It is more virulent, more infective, and is the cause of the majority of HIV infections globally. The lower infectivity of HIV-2 as compared with HIV-1 implies that fewer people exposed to HIV-2 will be infected per exposure. Because of its relatively poor capacity for transmission, HIV-2 is largely confined to West Africa
West Africa or Western Africa is the westernmost region of Africa. The United Nations defines Western Africa as the 16 countries of Benin, Burkina Faso, Cape Verde, The Gambia, Ghana, Guinea, Guinea-Bissau, Ivory Coast, Liberia, Mali ...
.
Pathophysiology
After the virus enters the body, there is a period of rapidviral replication
Viral replication is the formation of biological viruses during the infection process in the target host cells. Viruses must first get into the cell before viral replication can occur. Through the generation of abundant copies of its genome an ...
, leading to an abundance of virus in the peripheral blood. During primary infection, the level of HIV may reach several million virus particles per milliliter of blood. This response is accompanied by a marked drop in the number of circulating CD4+ T cells. The acute viremia is almost invariably associated with activation of CD8+ T cells, which kill HIV-infected cells, and subsequently with antibody production, or seroconversion. The CD8+ T cell response is thought to be important in controlling virus levels, which peak and then decline, as the CD4+ T cell counts recover. A good CD8+ T cell response has been linked to slower disease progression and a better prognosis, though it does not eliminate the virus.
Ultimately, HIV causes AIDS by depleting CD4+ T cells. This weakens the immune system and allows opportunistic infection
An opportunistic infection is an infection caused by pathogens (bacteria, fungi, parasites or viruses) that take advantage of an opportunity not normally available. These opportunities can stem from a variety of sources, such as a weakened immun ...
s. T cells are essential to the immune response and without them, the body cannot fight infections or kill cancerous cells. The mechanism of CD4+ T cell depletion differs in the acute and chronic phases. During the acute phase, HIV-induced cell lysis and killing of infected cells by CD8+ T cells accounts for CD4+ T cell depletion, although apoptosis
Apoptosis (from grc, ἀπόπτωσις, apóptōsis, 'falling off') is a form of programmed cell death that occurs in multicellular organisms. Biochemical events lead to characteristic cell changes ( morphology) and death. These changes in ...
may also be a factor. During the chronic phase, the consequences of generalized immune activation coupled with the gradual loss of the ability of the immune system to generate new T cells appear to account for the slow decline in CD4+ T cell numbers.
Although the symptoms of immune deficiency characteristic of AIDS do not appear for years after a person is infected, the bulk of CD4+ T cell loss occurs during the first weeks of infection, especially in the intestinal mucosa, which harbors the majority of the lymphocytes found in the body. The reason for the preferential loss of mucosal CD4+ T cells is that the majority of mucosal CD4+ T cells express the CCR5 protein which HIV uses as a co-receptor to gain access to the cells, whereas only a small fraction of CD4+ T cells in the bloodstream do so. A specific genetic change that alters the CCR5 protein when present in both chromosomes
A chromosome is a long DNA molecule with part or all of the genetic material of an organism. In most chromosomes the very long thin DNA fibers are coated with packaging proteins; in eukaryotic cells the most important of these proteins ar ...
very effectively prevents HIV-1 infection.
HIV seeks out and destroys CCR5 expressing CD4+ T cells during acute infection. A vigorous immune response eventually controls the infection and initiates the clinically latent phase. CD4+ T cells in mucosal tissues remain particularly affected. Continuous HIV replication causes a state of generalized immune activation persisting throughout the chronic phase. Immune activation, which is reflected by the increased activation state of immune cells and release of pro-inflammatory cytokine
Cytokines are a broad and loose category of small proteins (~5–25 kDa) important in cell signaling. Cytokines are peptides and cannot cross the lipid bilayer of cells to enter the cytoplasm. Cytokines have been shown to be involved in au ...
s, results from the activity of several HIV gene products and the immune response to ongoing HIV replication. It is also linked to the breakdown of the immune surveillance system of the gastrointestinal mucosal barrier caused by the depletion of mucosal CD4+ T cells during the acute phase of disease.
Diagnosis
 HIV/AIDS is diagnosed via laboratory testing and then staged based on the presence of certain signs or symptoms. HIV screening is recommended by the United States Preventive Services Task Force for all people 15 years to 65 years of age, including all pregnant women. Additionally, testing is recommended for those at high risk, which includes anyone diagnosed with a sexually transmitted illness. In many areas of the world, a third of HIV carriers only discover they are infected at an advanced stage of the disease when AIDS or severe immunodeficiency has become apparent.
HIV/AIDS is diagnosed via laboratory testing and then staged based on the presence of certain signs or symptoms. HIV screening is recommended by the United States Preventive Services Task Force for all people 15 years to 65 years of age, including all pregnant women. Additionally, testing is recommended for those at high risk, which includes anyone diagnosed with a sexually transmitted illness. In many areas of the world, a third of HIV carriers only discover they are infected at an advanced stage of the disease when AIDS or severe immunodeficiency has become apparent.
HIV testing

 Most people infected with HIV develop specific
Most people infected with HIV develop specific antibodies
An antibody (Ab), also known as an immunoglobulin (Ig), is a large, Y-shaped protein used by the immune system to identify and neutralize foreign objects such as pathogenic bacteria and viruses. The antibody recognizes a unique molecule of ...
(i.e. seroconvert) within three to twelve weeks after the initial infection. Diagnosis of primary HIV before seroconversion is done by measuring HIV- RNA or p24 antigen
HIV tests are used to detect the presence of the human immunodeficiency virus (HIV), the virus that causes acquired immunodeficiency syndrome (AIDS), in serum, saliva, or urine. Such tests may detect antibodies, antigens, or RNA.
AIDS diagnos ...
. Positive results obtained by antibody or PCR testing are confirmed either by a different antibody or by PCR.
Antibody tests in children younger than 18 months are typically inaccurate, due to the continued presence of maternal antibodies Passive immunity is the transfer of active humoral immunity of ready-made antibodies. Passive immunity can occur naturally, when maternal antibodies are transferred to the fetus through the placenta, and it can also be induced artificially, when ...
. Thus HIV infection can only be diagnosed by PCR testing for HIV RNA or DNA, or via testing for the p24 antigen. Much of the world lacks access to reliable PCR testing, and people in many places simply wait until either symptoms develop or the child is old enough for accurate antibody testing. In sub-Saharan Africa between 2007 and 2009, between 30% and 70% of the population were aware of their HIV status.UNAIDS 2011 pg. 70–80 In 2009, between 3.6% and 42% of men and women in sub-Saharan countries were tested; this represented a significant increase compared to previous years.
Classifications
Two main clinical staging systems are used to classify HIV and HIV-related disease forsurveillance
Surveillance is the monitoring of behavior, many activities, or information for the purpose of information gathering, influencing, managing or directing. This can include observation from a distance by means of electronic equipment, such as ...
purposes: the WHO disease staging system for HIV infection and disease WHO Disease Staging System for HIV Infection and Disease was first produced in 1990 by the World Health Organization and updated in September 2005. It is an approach for use in resource limited settings and is widely used in Africa and Asia and has ...
, and the CDC classification system for HIV infection
The CDC Classification System for HIV Infection is the medical classification system used by the United States Centers for Disease Control and Prevention (CDC) to classify HIV disease and infection. The system is used to allow the government to ...
. The CDC's classification system is more frequently adopted in developed countries. Since the WHO's staging system does not require laboratory tests, it is suited to the resource-restricted conditions encountered in developing countries, where it can also be used to help guide clinical management. Despite their differences, the two systems allow a comparison for statistical purposes.
The World Health Organization first proposed a definition for AIDS in 1986. Since then, the WHO classification has been updated and expanded several times, with the most recent version being published in 2007. The WHO system uses the following categories:
* Primary HIV infection: May be either asymptomatic or associated with acute retroviral syndrome
* Stage I: HIV infection is asymptomatic with a CD4+ T cell count (also known as CD4 count) greater than 500 per microlitre (µl or cubic mm) of blood. May include generalized lymph node enlargement.
* Stage II: Mild symptoms, which may include minor mucocutaneous manifestations and recurrent upper respiratory tract infections. A CD4 count of less than 500/µl
* Stage III: Advanced symptoms, which may include unexplained chronic diarrhea for longer than a month, severe bacterial infections including tuberculosis of the lung, and a CD4 count of less than 350/µl
* Stage IV or AIDS: severe symptoms, which include toxoplasmosis
Toxoplasmosis is a parasitic disease caused by '' Toxoplasma gondii'', an apicomplexan. Infections with toxoplasmosis are associated with a variety of neuropsychiatric and behavioral conditions. Occasionally, people may have a few weeks or mont ...
of the brain, candidiasis of the esophagus
The esophagus (American English) or oesophagus (British English; both ), non-technically known also as the food pipe or gullet, is an organ in vertebrates through which food passes, aided by peristaltic contractions, from the pharynx to t ...
, trachea
The trachea, also known as the windpipe, is a cartilaginous tube that connects the larynx to the bronchi of the lungs, allowing the passage of air, and so is present in almost all air- breathing animals with lungs. The trachea extends from t ...
, bronchi, or lung
The lungs are the primary organs of the respiratory system in humans and most other animals, including some snails and a small number of fish. In mammals and most other vertebrates, two lungs are located near the backbone on either side of ...
s, and Kaposi's sarcoma. A CD4 count of less than 200/µl
The U.S. Centers for Disease Control and Prevention also created a classification system for HIV, and updated it in 2008 and 2014. This system classifies HIV infections based on CD4 count and clinical symptoms, and describes the infection in five groups. In those greater than six years of age it is:
* Stage 0: the time between a negative or indeterminate HIV test followed less than 180 days by a positive test.
* Stage 1: CD4 count ≥ 500 cells/µl and no AIDS-defining conditions.
* Stage 2: CD4 count 200 to 500 cells/µl and no AIDS-defining conditions.
* Stage 3: CD4 count ≤ 200 cells/µl or AIDS-defining conditions.
* Unknown: if insufficient information is available to make any of the above classifications.
For surveillance purposes, the AIDS diagnosis still stands even if, after treatment, the CD4+ T cell count rises to above 200 per µL of blood or other AIDS-defining illnesses are cured.
Prevention

Sexual contact
 Consistent
Consistent condom
A condom is a sheath-shaped Barrier contraception, barrier device used during sexual intercourse to reduce the probability of pregnancy or a Sexually transmitted disease, sexually transmitted infection (STI). There are both male and female con ...
use reduces the risk of HIV transmission by approximately 80% over the long term. When condoms are used consistently by a couple in which one person is infected, the rate of HIV infection is less than 1% per year. There is some evidence to suggest that female condom
An internal condom (also known as a femidom or female condom) is a barrier device that is used during sexual intercourse as a barrier contraceptive to reduce the probability of pregnancy or a sexually transmitted infection (STI). Meant as an al ...
s may provide an equivalent level of protection. Application of a vaginal gel containing tenofovir (a reverse transcriptase inhibitor) immediately before sex seems to reduce infection rates by approximately 40% among African women. By contrast, use of the spermicide nonoxynol-9 may increase the risk of transmission due to its tendency to cause vaginal and rectal irritation.
Circumcision
Circumcision is a procedure that removes the foreskin from the human penis. In the most common form of the operation, the foreskin is extended with forceps, then a circumcision device may be placed, after which the foreskin is excised. Top ...
in sub-Saharan Africa
Sub-Saharan Africa is, geographically, the area and regions of the continent of Africa that lies south of the Sahara. These include West Africa, East Africa, Central Africa, and Southern Africa. Geopolitically, in addition to the List of sov ...
"reduces the acquisition of HIV by heterosexual men by between 38% and 66% over 24 months". Owing to these studies, both the World Health Organization and UNAIDS recommended male circumcision in 2007 as a method of preventing female-to-male HIV transmission in areas with high rates of HIV. However, whether it protects against male-to-female transmission is disputed,(subscription required) and whether it is of benefit in developed countries
A developed country (or industrialized country, high-income country, more economically developed country (MEDC), advanced country) is a sovereign state that has a high quality of life, developed economy and advanced technological infrastruct ...
and among men who have sex with men
Men who have sex with men (MSM) are male persons who engage in sexual activity with members of the same sex. The term was created in the 1990s by epidemiologists to study the spread of disease among all men who have sex with men, regardless of ...
is undetermined.
Programs encouraging sexual abstinence do not appear to affect subsequent HIV risk. Evidence of any benefit from peer education
Peer education is an approach to health promotion, in which community members are supported to promote health-enhancing change among their peers. Peer education is the teaching or sharing of health information, values and behavior in educating othe ...
is equally poor. Comprehensive sexual education provided at school may decrease high-risk behavior. A substantial minority of young people continues to engage in high-risk practices despite knowing about HIV/AIDS, underestimating their own risk of becoming infected with HIV. Voluntary counseling and testing people for HIV does not affect risky behavior in those who test negative but does increase condom use in those who test positive. Enhanced family planning services appear to increase the likelihood of women with HIV using contraception, compared to basic services. It is not known whether treating other sexually transmitted infections is effective in preventing HIV.
Pre-exposure
Antiretroviral treatment among people with HIV whose CD4 count ≤ 550 cells/µL is a very effective way to prevent HIV infection of their partner (a strategy known as treatment as prevention, or TASP). TASP is associated with a 10- to 20-fold reduction in transmission risk. Pre-exposure prophylaxis (PrEP) with a daily dose of the medications tenofovir, with or without emtricitabine, is effective in people at high risk including men who have sex with men, couples where one is HIV-positive, and young heterosexuals in Africa. It may also be effective in intravenous drug users, with a study finding a decrease in risk of 0.7 to 0.4 per 100 person years. TheUSPSTF
The United States Preventive Services Task Force (USPSTF) is "an independent panel of experts in primary care and prevention that systematically reviews the evidence of effectiveness and develops recommendations for clinical preventive services". ...
, in 2019, recommended PrEP in those who are at high risk.
Universal precautions within the health care environment are believed to be effective in decreasing the risk of HIV. Intravenous drug use is an important risk factor, and harm reduction strategies such as needle-exchange program
A needle and syringe programme (NSP), also known as needle exchange program (NEP), is a social service that allows injecting drug users (IDUs) to obtain clean and unused hypodermic needles and associated paraphernalia at little or no cost. It ...
s and opioid substitution therapy appear effective in decreasing this risk.
Post-exposure
A course of antiretrovirals administered within 48 to 72 hours after exposure to HIV-positive blood or genital secretions is referred to as post-exposure prophylaxis (PEP). The use of the single agent zidovudine reduces the risk of a HIV infection five-fold following a needle-stick injury. , the prevention regimen recommended in the United States consists of three medications— tenofovir, emtricitabine andraltegravir
Raltegravir, sold under the brand name Isentress, is an antiretroviral medication used, together with other medication, to treat HIV/AIDS. It may also be used, as part of post exposure prophylaxis, to prevent HIV infection following potential ex ...
—as this may reduce the risk further.
PEP treatment is recommended after a sexual assault
Sexual assault is an act in which one intentionally sexually touches another person without that person's consent, or coerces or physically forces a person to engage in a sexual act against their will. It is a form of sexual violence, which ...
when the perpetrator is known to be HIV-positive, but is controversial when their HIV status is unknown. The duration of treatment is usually four weeks and is frequently associated with adverse effects—where zidovudine is used, about 70% of cases result in adverse effects such as nausea (24%), fatigue (22%), emotional distress (13%) and headaches (9%).
Mother-to-child
Programs to prevent the vertical transmission of HIV (from mothers to children) can reduce rates of transmission by 92–99%. This primarily involves the use of a combination of antiviral medications during pregnancy and after birth in the infant, and potentially includes bottle feeding rather thanbreastfeeding
Breastfeeding, or nursing, is the process by which human breast milk is fed to a child. Breast milk may be from the breast, or may be expressed by hand or pumped and fed to the infant. The World Health Organization (WHO) recommends that bre ...
. If replacement feeding is acceptable, feasible, affordable, sustainable and safe, mothers should avoid breastfeeding their infants; however, exclusive breastfeeding is recommended during the first months of life if this is not the case. If exclusive breastfeeding is carried out, the provision of extended antiretroviral prophylaxis to the infant decreases the risk of transmission. In 2015, Cuba
Cuba ( , ), officially the Republic of Cuba ( es, República de Cuba, links=no ), is an island country comprising the island of Cuba, as well as Isla de la Juventud and several minor archipelagos. Cuba is located where the northern Caribb ...
became the first country in the world to eradicate mother-to-child transmission of HIV.
Vaccination
Currently there is no licensed vaccine for HIV or AIDS. The most effective vaccine trial to date,RV 144 RV 144, or the Thai trial, was an HIV vaccine clinical trial that was conducted in Thailand between 2003 and 2006. It used a combination of two HIV vaccines that had each failed in earlier trials. Participants were vaccinated over the course of 24 w ...
, was published in 2009; it found a partial reduction in the risk of transmission of roughly 30%, stimulating some hope in the research community of developing a truly effective vaccine. Further trials of the RV 144 vaccine are ongoing.
Treatment
There is currently no cure, nor an effective HIV vaccine. Treatment consists of highly active antiretroviral therapy (HAART), which slows progression of the disease. , more than 6.6 million people were receiving HAART in low- and middle-income countries.UNAIDS 2011 pg. 1–10 Treatment also includes preventive and active treatment of opportunistic infections. , four people have been successfully cleared of HIV. Rapid initiation of antiretroviral therapy within one week of diagnosis appear to improve treatment outcomes in low and medium-income settings.Antiviral therapy
 Current HAART options are combinations (or "cocktails") consisting of at least three medications belonging to at least two types, or "classes", of antiretroviral agents. Initially, treatment is typically a non-nucleoside reverse transcriptase inhibitor (NNRTI) plus two nucleoside analog reverse transcriptase inhibitors (NRTIs). Typical NRTIs include: zidovudine (AZT) or tenofovir (TDF) and lamivudine (3TC) or emtricitabine (FTC). , dolutegravir/lamivudine/tenofovir is listed by the
Current HAART options are combinations (or "cocktails") consisting of at least three medications belonging to at least two types, or "classes", of antiretroviral agents. Initially, treatment is typically a non-nucleoside reverse transcriptase inhibitor (NNRTI) plus two nucleoside analog reverse transcriptase inhibitors (NRTIs). Typical NRTIs include: zidovudine (AZT) or tenofovir (TDF) and lamivudine (3TC) or emtricitabine (FTC). , dolutegravir/lamivudine/tenofovir is listed by the World Health Organization
The World Health Organization (WHO) is a specialized agency of the United Nations responsible for international public health. The WHO Constitution states its main objective as "the attainment by all peoples of the highest possible level o ...
as the first-line treatment for adults, with tenofovir/lamivudine/efavirenz as an alternative. Combinations of agents that include protease inhibitors (PI) are used if the above regimen loses effectiveness.
The World Health Organization and the United States recommend antiretrovirals in people of all ages (including pregnant women) as soon as the diagnosis is made, regardless of CD4 count. Once treatment is begun, it is recommended that it is continued without breaks or "holidays". Many people are diagnosed only after treatment ideally should have begun. The desired outcome of treatment is a long-term plasma HIV-RNA count below 50 copies/mL. Levels to determine if treatment is effective are initially recommended after four weeks and once levels fall below 50 copies/mL checks every three to six months are typically adequate. Inadequate control is deemed to be greater than 400 copies/mL. Based on these criteria treatment is effective in more than 95% of people during the first year.
Benefits of treatment include a decreased risk of progression to AIDS and a decreased risk of death. In the developing world, treatment also improves physical and mental health. With treatment, there is a 70% reduced risk of acquiring tuberculosis. Additional benefits include a decreased risk of transmission of the disease to sexual partners and a decrease in mother-to-child transmission. The effectiveness of treatment depends to a large part on compliance. Reasons for non-adherence to treatment include poor access to medical care, inadequate social supports, mental illness
A mental disorder, also referred to as a mental illness or psychiatric disorder, is a behavioral or mental pattern that causes significant distress or impairment of personal functioning. Such features may be persistent, relapsing and remitt ...
and drug abuse. The complexity of treatment regimens (due to pill numbers and dosing frequency) and adverse effect
An adverse effect is an undesired harmful effect resulting from a medication or other intervention, such as surgery. An adverse effect may be termed a " side effect", when judged to be secondary to a main or therapeutic effect. The term compl ...
s may reduce adherence. Even though cost is an important issue with some medications, 47% of those who needed them were taking them in low- and middle-income countries , and the rate of adherence is similar in low-income and high-income countries.
Specific adverse events are related to the antiretroviral agent taken. Some relatively common adverse events include: lipodystrophy syndrome, dyslipidemia, and diabetes mellitus
Diabetes, also known as diabetes mellitus, is a group of metabolic disorders characterized by a high blood sugar level ( hyperglycemia) over a prolonged period of time. Symptoms often include frequent urination, increased thirst and increased ...
, especially with protease inhibitors. Other common symptoms include diarrhea, and an increased risk of cardiovascular disease
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, hea ...
. Newer recommended treatments are associated with fewer adverse effects. Certain medications may be associated with birth defect
A birth defect, also known as a congenital disorder, is an abnormal condition that is present at birth regardless of its cause. Birth defects may result in disabilities that may be physical, intellectual, or developmental. The disabilities ca ...
s and therefore may be unsuitable for women hoping to have children.
Treatment recommendations for children are somewhat different from those for adults. The World Health Organization recommends treating all children less than five years of age; children above five are treated like adults. The United States guidelines recommend treating all children less than 12 months of age and all those with HIV RNA counts greater than 100,000 copies/mL between one year and five years of age.
The European Medicines Agency
The European Medicines Agency (EMA) is an agency of the European Union (EU) in charge of the evaluation and supervision of medicinal products. Prior to 2004, it was known as the European Agency for the Evaluation of Medicinal Products or Eur ...
(EMA) has recommended the granting of marketing authorizations for two new antiretroviral (ARV) medicines, rilpivirine
Rilpivirine, sold under the brand names Edurant and Rekambys, is a medication, developed by Tibotec, used for the treatment of HIV/AIDS. It is a second-generation non-nucleoside reverse transcriptase inhibitor (NNRTI) with higher potency, longer ...
(Rekambys) and cabotegravir (Vocabria), to be used together for the treatment of people with human immunodeficiency virus type 1 (HIV-1) infection. Text was copied from this source which is © European Medicines Agency. Reproduction is authorized provided the source is acknowledged. The two medicines are the first ARVs that come in a long-acting injectable formulation. This means that instead of daily pills, people receive intramuscular injections monthly or every two months.
The combination of Rekambys and Vocabria injection is intended for maintenance treatment of adults who have undetectable HIV levels in the blood (viral load less than 50 copies/ml) with their current ARV treatment, and when the virus has not developed resistance to a certain class of anti-HIV medicines called non-nucleoside reverse transcriptase inhibitors (NNRTIs) and integrase strand transfer inhibitors (INIs).
Cabotegravir combined with rilpivirine (Cabenuva) is a complete regimen for the treatment of human immunodeficiency virus type 1 (HIV-1) infection in adults to replace a current antiretroviral regimen in those who are virologically suppressed on a stable antiretroviral regimen with no history of treatment failure and with no known or suspected resistance to either cabotegravir or rilpivirine
Rilpivirine, sold under the brand names Edurant and Rekambys, is a medication, developed by Tibotec, used for the treatment of HIV/AIDS. It is a second-generation non-nucleoside reverse transcriptase inhibitor (NNRTI) with higher potency, longer ...
.
Opportunistic infections
Measures to prevent opportunistic infections are effective in many people with HIV/AIDS. In addition to improving current disease, treatment with antiretrovirals reduces the risk of developing additional opportunistic infections. Adults and adolescents who are living with HIV (even on anti-retroviral therapy) with no evidence of active tuberculosis in settings with high tuberculosis burden should receive isoniazid preventive therapy (IPT); the tuberculin skin test can be used to help decide if IPT is needed. Children with HIV may benefit from screening for tuberculosis.Vaccination
Vaccination is the administration of a vaccine to help the immune system develop immunity from a disease. Vaccines contain a microorganism or virus in a weakened, live or killed state, or proteins or toxins from the organism. In stimulat ...
against hepatitis
Hepatitis is inflammation of the liver tissue. Some people or animals with hepatitis have no symptoms, whereas others develop yellow discoloration of the skin and whites of the eyes ( jaundice), poor appetite, vomiting, tiredness, abdominal ...
A and B is advised for all people at risk of HIV before they become infected; however, it may also be given after infection.
Trimethoprim/sulfamethoxazole prophylaxis between four and six weeks of age, and ceasing breastfeeding of infants born to HIV-positive mothers, is recommended in resource-limited settings.UNAIDS 2011 pg. 150–160 It is also recommended to prevent PCP when a person's CD4 count is below 200 cells/uL and in those who have or have previously had PCP. People with substantial immunosuppression are also advised to receive prophylactic therapy for toxoplasmosis
Toxoplasmosis is a parasitic disease caused by '' Toxoplasma gondii'', an apicomplexan. Infections with toxoplasmosis are associated with a variety of neuropsychiatric and behavioral conditions. Occasionally, people may have a few weeks or mont ...
and MAC. Appropriate preventive measures reduced the rate of these infections by 50% between 1992 and 1997. Influenza vaccination and pneumococcal polysaccharide vaccine are often recommended in people with HIV/AIDS with some evidence of benefit.
Diet
The World Health Organization (WHO) has issued recommendations regarding nutrient requirements in HIV/AIDS. A generally healthy diet is promoted. Dietary intake of micronutrients at RDA levels by HIV-infected adults is recommended by the WHO; higher intake ofvitamin A
Vitamin A is a fat-soluble vitamin and an essential nutrient for humans. It is a group of organic compounds that includes retinol, retinal (also known as retinaldehyde), retinoic acid, and several provitamin A carotenoids (most notably ...
, zinc
Zinc is a chemical element with the symbol Zn and atomic number 30. Zinc is a slightly brittle metal at room temperature and has a shiny-greyish appearance when oxidation is removed. It is the first element in group 12 (IIB) of the periodi ...
, and iron can produce adverse effects in HIV-positive adults, and is not recommended unless there is documented deficiency. Dietary supplementation for people who are infected with HIV and who have inadequate nutrition or dietary deficiencies may strengthen their immune systems or help them recover from infections; however, evidence indicating an overall benefit in morbidity or reduction in mortality is not consistent.
Evidence for supplementation with selenium is mixed with some tentative evidence of benefit. For pregnant and lactating women with HIV, multivitamin
A multivitamin is a preparation intended to serve as a dietary supplement with vitamins, dietary minerals, and other nutritional elements. Such preparations are available in the form of tablets, capsules, pastilles, powders, liquids, or injecta ...
supplement improves outcomes for both mothers and children. If the pregnant or lactating mother has been advised to take anti-retroviral medication to prevent mother-to-child HIV transmission, multivitamin supplements should not replace these treatments. There is some evidence that vitamin A supplementation in children with an HIV infection reduces mortality and improves growth.
Alternative medicine
In the US, approximately 60% of people with HIV use various forms of complementary or alternative medicine, whose effectiveness has not been established. There is not enough evidence to support the use ofherbal medicine
Herbal medicine (also herbalism) is the study of pharmacognosy and the use of medicinal plants, which are a basis of traditional medicine. With worldwide research into pharmacology, some herbal medicines have been translated into modern remedie ...
s. There is insufficient evidence to recommend or support the use of medical cannabis
Medical cannabis, or medical marijuana (MMJ), is cannabis and cannabinoids that are prescribed by physicians for their patients. The use of cannabis as medicine has not been rigorously tested due to production and governmental restriction ...
to try to increase appetite or weight gain.
Prognosis
cancer
Cancer is a group of diseases involving abnormal cell growth with the potential to invade or spread to other parts of the body. These contrast with benign tumors, which do not spread. Possible signs and symptoms include a lump, abnormal b ...
, both of which are frequently the result of the progressive failure of the immune system. Risk of cancer appears to increase once the CD4 count is below 500/μL. The rate of clinical disease progression varies widely between individuals and has been shown to be affected by a number of factors such as a person's susceptibility and immune function; their access to health care, the presence of co-infections; and the particular strain (or strains) of the virus involved.
Tuberculosis
Tuberculosis (TB) is an infectious disease usually caused by '' Mycobacterium tuberculosis'' (MTB) bacteria. Tuberculosis generally affects the lungs, but it can also affect other parts of the body. Most infections show no symptoms, ...
co-infection is one of the leading causes of sickness and death in those with HIV/AIDS being present in a third of all HIV-infected people and causing 25% of HIV-related deaths. HIV is also one of the most important risk factors for tuberculosis. Hepatitis C
Hepatitis C is an infectious disease caused by the hepatitis C virus (HCV) that primarily affects the liver; it is a type of viral hepatitis. During the initial infection people often have mild or no symptoms. Occasionally a fever, dark urine, ...
is another very common co-infection where each disease increases the progression of the other. The two most common cancers associated with HIV/AIDS are Kaposi's sarcoma and AIDS-related non-Hodgkin's lymphoma. Other cancers that are more frequent include anal cancer, Burkitt's lymphoma
Burkitt lymphoma is a cancer of the lymphatic system, particularly B lymphocytes found in the germinal center. It is named after Denis Parsons Burkitt, the Irish surgeon who first described the disease in 1958 while working in equatorial Africa. ...
, primary central nervous system lymphoma
Primary central nervous system lymphoma (PCNSL), also termed primary diffuse large B-cell lymphoma of the central nervous system (DLBCL-CNS), is a primary intracranial tumor appearing mostly in patients with severe immunodeficiency (typically pat ...
, and cervical cancer
Cervical cancer is a cancer arising from the cervix. It is due to the abnormal growth of cells that have the ability to invade or spread to other parts of the body. Early on, typically no symptoms are seen. Later symptoms may include abnormal ...
.
Even with anti-retroviral treatment, over the long term HIV-infected people may experience neurocognitive disorders, osteoporosis, neuropathy
Peripheral neuropathy, often shortened to neuropathy, is a general term describing disease affecting the peripheral nerves, meaning nerves beyond the brain and spinal cord. Damage to peripheral nerves may impair sensation, movement, gland, or o ...
, cancers, nephropathy, and cardiovascular disease
Cardiovascular disease (CVD) is a class of diseases that involve the heart or blood vessels. CVD includes coronary artery diseases (CAD) such as angina and myocardial infarction (commonly known as a heart attack). Other CVDs include stroke, hea ...
. Some conditions, such as lipodystrophy, may be caused both by HIV and its treatment.
Epidemiology
 Some authors consider HIV/AIDS a global
Some authors consider HIV/AIDS a global pandemic
A pandemic () is an epidemic of an infectious disease that has spread across a large region, for instance multiple continents or worldwide, affecting a substantial number of individuals. A widespread endemic disease with a stable number of in ...
. approximately 36.7 million people worldwide have HIV, the number of new infections that year being about 1.8 million. This is down from 3.1 million new infections in 2001. Slightly over half the infected population are women and 2.1 million are children. It resulted in about 1 million deaths in 2016, down from a peak of 1.9 million in 2005.
Sub-Saharan Africa
Sub-Saharan Africa is, geographically, the area and regions of the continent of Africa that lies south of the Sahara. These include West Africa, East Africa, Central Africa, and Southern Africa. Geopolitically, in addition to the List of sov ...
is the region most affected. In 2010, an estimated 68% (22.9 million) of all HIV cases and 66% of all deaths (1.2 million) occurred in this region.UNAIDS 2011 pg. 20–30 This means that about 5% of the adult population is infectedUNAIDS 2011 pp. 40–50 and it is believed to be the cause of 10% of all deaths in children.Mandell, Bennett, and Dolan (2010). Chapter 117. Here, in contrast to other regions, women comprise nearly 60% of cases. South Africa
South Africa, officially the Republic of South Africa (RSA), is the southernmost country in Africa. It is bounded to the south by of coastline that stretch along the South Atlantic and Indian Oceans; to the north by the neighbouring coun ...
has the largest population of people with HIV of any country in the world at 5.9 million. Life expectancy
Life expectancy is a statistical measure of the average time an organism is expected to live, based on the year of its birth, current age, and other demographic factors like sex. The most commonly used measure is life expectancy at birth ...
has fallen in the worst-affected countries due to HIV/AIDS; for example, in 2006 it was estimated that it had dropped from 65 to 35 years in Botswana
Botswana (, ), officially the Republic of Botswana ( tn, Lefatshe la Botswana, label= Setswana, ), is a landlocked country in Southern Africa. Botswana is topographically flat, with approximately 70 percent of its territory being the Kal ...
. Mother-to-child transmission in Botswana and South Africa, , has decreased to less than 5%, with improvement in many other African nations due to improved access to antiretroviral therapy.
South & South East Asia is the second most affected; in 2010 this region contained an estimated 4 million cases or 12% of all people living with HIV resulting in approximately 250,000 deaths. Approximately 2.4 million of these cases are in India.
During 2008 in the United States approximately 1.2 million people were living with HIV, resulting in about 17,500 deaths. The US Centers for Disease Control and Prevention estimated that in that year, 20% of infected Americans were unaware of their infection. about 675,000 people have died of HIV/AIDS in the US since the beginning of the HIV epidemic. In the United Kingdom
The United Kingdom of Great Britain and Northern Ireland, commonly known as the United Kingdom (UK) or Britain, is a country in Europe, off the north-western coast of the continental mainland. It comprises England, Scotland, Wales and ...
, there were approximately 101,200 cases which resulted in 594 deaths. In Canada as of 2008, there were about 65,000 cases causing 53 deaths. Between the first recognition of AIDS (in 1981) and 2009, it has led to nearly 30 million deaths. Rates of HIV are lowest in North Africa and the Middle East (0.1% or less), East Asia
East Asia is the eastern region of Asia, which is defined in both geographical and ethno-cultural terms. The modern states of East Asia include China, Japan, Mongolia, North Korea, South Korea, and Taiwan. China, North Korea, South Korea ...
(0.1%), and Western and Central Europe (0.2%). The worst-affected European countries, in 2009 and 2012 estimates, are Russia
Russia (, , ), or the Russian Federation, is a transcontinental country spanning Eastern Europe and Northern Asia. It is the largest country in the world, with its internationally recognised territory covering , and encompassing one-ei ...
, Ukraine
Ukraine ( uk, Україна, Ukraïna, ) is a country in Eastern Europe. It is the second-largest European country after Russia, which it borders to the east and northeast. Ukraine covers approximately . Prior to the ongoing Russian inva ...
, Latvia
Latvia ( or ; lv, Latvija ; ltg, Latveja; liv, Leţmō), officially the Republic of Latvia ( lv, Latvijas Republika, links=no, ltg, Latvejas Republika, links=no, liv, Leţmō Vabāmō, links=no), is a country in the Baltic region of ...
, Moldova
Moldova ( , ; ), officially the Republic of Moldova ( ro, Republica Moldova), is a landlocked country in Eastern Europe. It is bordered by Romania to the west and Ukraine to the north, east, and south. The unrecognised state of Transnistri ...
, Portugal
Portugal, officially the Portuguese Republic ( pt, República Portuguesa, links=yes ), is a country whose mainland is located on the Iberian Peninsula of Southwestern Europe, and whose territory also includes the Atlantic archipelagos of th ...
and Belarus
Belarus,, , ; alternatively and formerly known as Byelorussia (from Russian ). officially the Republic of Belarus,; rus, Республика Беларусь, Respublika Belarus. is a landlocked country in Eastern Europe. It is bordered by ...
, in decreasing order of prevalence.
History
Discovery
 The first news story on the disease appeared on May 18, 1981, in the gay newspaper '' New York Native''. AIDS was first clinically reported on June 5, 1981, with five cases in the United States. The initial cases were a cluster of injecting drug users and gay men with no known cause of impaired immunity who showed symptoms of '' Pneumocystis carinii'' pneumonia (PCP), a rare opportunistic infection that was known to occur in people with very compromised immune systems. Soon thereafter, a large number of homosexual men developed a generally rare skin cancer called Kaposi's sarcoma (KS). Many more cases of PCP and KS emerged, alerting U.S. Centers for Disease Control and Prevention (CDC) and a CDC task force was formed to monitor the outbreak.
In the early days, the CDC did not have an official name for the disease, often referring to it by way of diseases associated with it, such as lymphadenopathy, the disease after which the discoverers of HIV originally named the virus. They also used ''Kaposi's sarcoma and opportunistic infections'', the name by which a task force had been set up in 1981. At one point the CDC referred to it as the "4H disease", as the syndrome seemed to affect heroin users, homosexuals,
The first news story on the disease appeared on May 18, 1981, in the gay newspaper '' New York Native''. AIDS was first clinically reported on June 5, 1981, with five cases in the United States. The initial cases were a cluster of injecting drug users and gay men with no known cause of impaired immunity who showed symptoms of '' Pneumocystis carinii'' pneumonia (PCP), a rare opportunistic infection that was known to occur in people with very compromised immune systems. Soon thereafter, a large number of homosexual men developed a generally rare skin cancer called Kaposi's sarcoma (KS). Many more cases of PCP and KS emerged, alerting U.S. Centers for Disease Control and Prevention (CDC) and a CDC task force was formed to monitor the outbreak.
In the early days, the CDC did not have an official name for the disease, often referring to it by way of diseases associated with it, such as lymphadenopathy, the disease after which the discoverers of HIV originally named the virus. They also used ''Kaposi's sarcoma and opportunistic infections'', the name by which a task force had been set up in 1981. At one point the CDC referred to it as the "4H disease", as the syndrome seemed to affect heroin users, homosexuals, hemophiliacs
Haemophilia, or hemophilia (), is a mostly inherited genetic disorder that impairs the body's ability to make blood clots, a process needed to stop bleeding. This results in people bleeding for a longer time after an injury, easy bruising ...
, and Haiti
Haiti (; ht, Ayiti ; French: ), officially the Republic of Haiti (); ) and formerly known as Hayti, is a country located on the island of Hispaniola in the Greater Antilles archipelago of the Caribbean Sea, east of Cuba and Jamaica, and s ...
ans. The term ''GRID'', which stood for gay-related immune deficiency
AIDS is caused by a human immunodeficiency virus (HIV), which originated in non-human primates
in Central and West Africa. While various sub-groups of the virus acquired human infectivity at different times, the present pandemic had its origins i ...
, had also been coined. However, after determining that AIDS was not isolated to the gay community, it was realized that the term ''GRID'' was misleading, and the term ''AIDS'' was introduced at a meeting in July 1982. By September 1982 the CDC started referring to the disease as AIDS.
In 1983, two separate research groups led by Robert Gallo and Luc Montagnier
Luc Montagnier (; , ; 18 August 1932 – 8 February 2022) was a French virologist and joint recipient, with and , of the 2008 Nobel Prize in Physiology or Medicine for his discovery of the human immunodeficiency virus (HIV). He worked as a r ...
declared that a novel retrovirus may have been infecting people with AIDS, and published their findings in the same issue of the journal ''Science
Science is a systematic endeavor that builds and organizes knowledge in the form of testable explanations and predictions about the universe.
Science may be as old as the human species, and some of the earliest archeological evidence ...
''. Gallo claimed a virus which his group had isolated from a person with AIDS was strikingly similar in shape
A shape or figure is a graphical representation of an object or its external boundary, outline, or external surface, as opposed to other properties such as color, texture, or material type.
A plane shape or plane figure is constrained to lie ...
to other human T-lymphotropic virus
The human T-lymphotropic virus, human T-cell lymphotropic virus, or human T-cell leukemia-lymphoma virus (HTLV) family of viruses are a group of human retroviruses that are known to cause a type of cancer called adult T-cell leukemia/lymphoma and ...
es (HTLVs) that his group had been the first to isolate. Gallo's group called their newly isolated virus HTLV-III. At the same time, Montagnier's group isolated a virus from a person presenting with swelling of the lymph nodes of the neck and physical weakness, two characteristic symptoms of AIDS. Contradicting the report from Gallo's group, Montagnier and his colleagues showed that core proteins of this virus were immunologically different from those of HTLV-I. Montagnier's group named their isolated virus lymphadenopathy-associated virus (LAV). As these two viruses turned out to be the same, in 1986, LAV and HTLV-III were renamed HIV.
Origins
 The origin of HIV / AIDS and the circumstances that led to its emergence remain unsolved.
Both HIV-1 and HIV-2 are believed to have originated in non-human
The origin of HIV / AIDS and the circumstances that led to its emergence remain unsolved.
Both HIV-1 and HIV-2 are believed to have originated in non-human primate
Primates are a diverse order of mammals. They are divided into the strepsirrhines, which include the lemurs, galagos, and lorisids, and the haplorhines, which include the tarsiers and the simians ( monkeys and apes, the latter includin ...
s in West-central Africa and were transferred to humans in the early 20th century. HIV-1 appears to have originated in southern Cameroon
Cameroon (; french: Cameroun, ff, Kamerun), officially the Republic of Cameroon (french: République du Cameroun, links=no), is a country in west-central Africa. It is bordered by Nigeria to the west and north; Chad to the northeast; the ...
through the evolution of SIV(cpz), a simian immunodeficiency virus (SIV) that infects wild chimpanzee
The chimpanzee (''Pan troglodytes''), also known as simply the chimp, is a species of great ape native to the forest and savannah of tropical Africa. It has four confirmed subspecies and a fifth proposed subspecies. When its close relative t ...
s (HIV-1 descends from the SIVcpz endemic in the chimpanzee subspecies ''Pan troglodytes troglodytes''). The closest relative of HIV-2 is SIV (smm), a virus of the sooty mangabey (''Cercocebus atys atys''), an Old World monkey living in coastal West Africa (from southern Senegal
Senegal,; Wolof: ''Senegaal''; Pulaar: 𞤅𞤫𞤲𞤫𞤺𞤢𞥄𞤤𞤭 (Senegaali); Arabic: السنغال ''As-Sinighal'') officially the Republic of Senegal,; Wolof: ''Réewum Senegaal''; Pulaar : 𞤈𞤫𞤲𞤣𞤢𞥄𞤲𞤣𞤭 ...
to western Ivory Coast
Ivory Coast, also known as Côte d'Ivoire, officially the Republic of Côte d'Ivoire, is a country on the southern coast of West Africa. Its capital is Yamoussoukro, in the centre of the country, while its largest city and economic centre i ...
). New World monkeys such as the owl monkey are resistant to HIV-1 infection, possibly because of a genomic fusion of two viral resistance genes.(subscription required) HIV-1 is thought to have jumped the species barrier on at least three separate occasions, giving rise to the three groups of the virus, M, N, and O.
There is evidence that humans who participate in bushmeat activities, either as hunters or as bushmeat vendors, commonly acquire SIV. However, SIV is a weak virus which is typically suppressed by the human immune system within weeks of infection. It is thought that several transmissions of the virus from individual to individual in quick succession are necessary to allow it enough time to mutate into HIV. Furthermore, due to its relatively low person-to-person transmission rate, SIV can only spread throughout the population in the presence of one or more high-risk transmission channels, which are thought to have been absent in Africa before the 20th century.
Specific proposed high-risk transmission channels, allowing the virus to adapt to humans and spread throughout society, depend on the proposed timing of the animal-to-human crossing. Genetic studies of the virus suggest that the most recent common ancestor of the HIV-1 M group dates back to 1910. (subscription required) Proponents of this dating link the HIV epidemic with the emergence of colonialism
Colonialism is a practice or policy of control by one people or power over other people or areas, often by establishing colonies and generally with the aim of economic dominance. In the process of colonisation, colonisers may impose their reli ...
and growth of large colonial African cities, leading to social changes, including a higher degree of sexual promiscuity, the spread of prostitution, and the accompanying high frequency of genital ulcer disease
A genital ulcer is an open sore located on the genital area, which includes the vulva, penis, perianal region, or anus. Genital ulcers are most commonly caused by infectious agents (fungal infections, secondary bacterial infections, or sexually t ...
s (such as syphilis
Syphilis () is a sexually transmitted infection caused by the bacterium '' Treponema pallidum'' subspecies ''pallidum''. The signs and symptoms of syphilis vary depending in which of the four stages it presents (primary, secondary, latent, a ...
) in nascent colonial cities. While transmission rates of HIV during vaginal intercourse are low under regular circumstances, they are increased manyfold if one of the partners has a sexually transmitted infection causing genital ulcers. Early 1900s colonial cities were notable for their high prevalence of prostitution and genital ulcers, to the degree that, as of 1928, as many as 45% of female residents of eastern Kinshasa
Kinshasa (; ; ln, Kinsásá), formerly Léopoldville ( nl, Leopoldstad), is the capital and largest city of the Democratic Republic of the Congo. Once a site of fishing and trading villages situated along the Congo River, Kinshasa is now one of ...
were thought to have been prostitutes, and, as of 1933, around 15% of all residents of the same city had syphilis.
An alternative view holds that unsafe medical practices in Africa after World War II, such as unsterile reuse of single-use syringes during mass vaccination, antibiotic and anti-malaria treatment campaigns, were the initial vector that allowed the virus to adapt to humans and spread.(subscription required)
The earliest well-documented case of HIV in a human dates back to 1959 in the Congo. The virus may have been present in the U.S. as early as the mid-to-late 1950s, as a sixteen-year-old male named Robert Rayford
Robert Lee Rayford (February 3, 1953 – May 15 1969), sometimes identified as Robert R. due to his age, was an American teenager from Missouri who has been suggested to represent the earliest confirmed case of HIV/AIDS in North America based ...
presented with symptoms in 1966 and died in 1969. In the 1970s, there were cases of getting parasites and becoming sick with what was called “gay bowel disease,” but what is now suspected to have been AIDS.
The earliest retrospectively described case of AIDS is believed to have been in Norway beginning in 1966. In July 1960, in the wake of Congo's independence, the United Nations
The United Nations (UN) is an intergovernmental organization whose stated purposes are to maintain international peace and security, develop friendly relations among nations, achieve international cooperation, and be a centre for harmoni ...
recruited Francophone
French became an international language in the Middle Ages, when the power of the Kingdom of France made it the second international language, alongside Latin. This status continued to grow into the 18th century, by which time French was the l ...
experts and technicians from all over the world to assist in filling administrative gaps left by Belgium
Belgium, ; french: Belgique ; german: Belgien officially the Kingdom of Belgium, is a country in Northwestern Europe. The country is bordered by the Netherlands to the north, Germany to the east, Luxembourg to the southeast, France to ...
, who did not leave behind an African elite to run the country. By 1962, Haitians made up the second-largest group of well-educated experts (out of the 48 national groups recruited), that totaled around 4500 in the country. Dr. Jacques Pépin, a Canadian author of ''The Origins of AIDS'', stipulates that Haiti was one of HIV's entry points to the U.S. and that a Haitian may have carried HIV back across the Atlantic in the 1960s. Although there was known to have been at least one case of AIDS in the U.S. from 1966, the vast majority of infections occurring outside sub-Saharan Africa (including the U.S.) can be traced back to a single unknown individual who became infected with HIV in Haiti
Haiti (; ht, Ayiti ; French: ), officially the Republic of Haiti (); ) and formerly known as Hayti, is a country located on the island of Hispaniola in the Greater Antilles archipelago of the Caribbean Sea, east of Cuba and Jamaica, and s ...
and then brought the infection to the U.S. at some time around 1969. The epidemic then rapidly spread among high-risk groups (initially, sexually promiscuous men who have sex with men). By 1978, the prevalence of HIV-1 among gay male residents of New York City
New York, often called New York City or NYC, is the List of United States cities by population, most populous city in the United States. With a 2020 population of 8,804,190 distributed over , New York City is also the L ...
and San Francisco
San Francisco (; Spanish for " Saint Francis"), officially the City and County of San Francisco, is the commercial, financial, and cultural center of Northern California. The city proper is the fourth most populous in California and 17t ...
was estimated at 5%, suggesting that several thousand individuals in the country had been infected.
Society and culture
Stigma
 AIDS stigma exists around the world in a variety of ways, including ostracism, rejection, discrimination and avoidance of HIV-infected people; compulsory HIV testing without prior consent or protection of confidentiality; violence against HIV-infected individuals or people who are perceived to be infected with HIV; and the
AIDS stigma exists around the world in a variety of ways, including ostracism, rejection, discrimination and avoidance of HIV-infected people; compulsory HIV testing without prior consent or protection of confidentiality; violence against HIV-infected individuals or people who are perceived to be infected with HIV; and the quarantine
A quarantine is a restriction on the movement of people, animals and goods which is intended to prevent the spread of disease or pests. It is often used in connection to disease and illness, preventing the movement of those who may have been ...
of HIV-infected individuals. Stigma-related violence or the fear of violence prevents many people from seeking HIV testing, returning for their results, or securing treatment, possibly turning what could be a manageable chronic illness into a death sentence and perpetuating the spread of HIV.
AIDS stigma has been further divided into the following three categories:
* ''Instrumental AIDS stigma''—a reflection of the fear and apprehension that are likely to be associated with any deadly and transmissible illness.
* ''Symbolic AIDS stigma''—the use of HIV/AIDS to express attitudes toward the social groups or lifestyles perceived to be associated with the disease.
* ''Courtesy AIDS stigma''—stigmatization of people connected to the issue of HIV/AIDS or HIV-positive people.
Often, AIDS stigma is expressed in conjunction with one or more other stigmas, particularly those associated with homosexuality, bisexuality
Bisexuality is a romantic or sexual attraction or behavior toward both males and females, or to more than one gender. It may also be defined to include romantic or sexual attraction to people regardless of their sex or gender identity, ...
, promiscuity, prostitution, and intravenous drug use.
In many developed countries
A developed country (or industrialized country, high-income country, more economically developed country (MEDC), advanced country) is a sovereign state that has a high quality of life, developed economy and advanced technological infrastruct ...
, there is an association between AIDS and homosexuality or bisexuality, and this association is correlated with higher levels of sexual prejudice, such as anti-homosexual or anti-bisexual attitudes. There is also a perceived association between AIDS and all male-male sexual behavior, including sex between uninfected men. However, the dominant mode of spread worldwide for HIV remains heterosexual transmission. To get a better understanding of the anti-homosexual attitudes around AIDs the musical ''Rent'' explores this.
In 2003, as part of an overall reform of marriage and population legislation, it became legal for those diagnosed with AIDS to marry in China.
In 2013, the U.S. National Library of Medicine developed a traveling exhibition titled ''Surviving and Thriving: AIDS, Politics, and Culture''; this covered medical research, the U.S. government's response, and personal stories from people with AIDS, caregivers, and activists.
Economic impact
gross domestic product
Gross domestic product (GDP) is a monetary measure of the market value of all the final goods and services produced and sold (not resold) in a specific time period by countries. Due to its complex and subjective nature this measure is of ...
of the most affected countries has decreased due to the lack of human capital. Without proper nutrition, health care and medicine, large numbers of people die from AIDS-related complications. Before death they will not only be unable to work, but will also require significant medical care. It is estimated that as of 2007 there were 12 million AIDS orphans. Many are cared for by elderly grandparents.
Returning to work after beginning treatment for HIV/AIDS is difficult, and affected people often work less than the average worker. Unemployment
Unemployment, according to the OECD (Organisation for Economic Co-operation and Development), is people above a specified age (usually 15) not being in paid employment or self-employment but currently available for work during the refe ...
in people with HIV/AIDS also is associated with suicidal ideation
Suicidal ideation, or suicidal thoughts, means having thoughts, ideas, or ruminations about the possibility of ending one's own life.World Health Organization, ''ICD-11 for Mortality and Morbidity Statistics'', ver. 09/2020MB26.A Suicidal ideatio ...
, memory problems, and social isolation. Employment increases self-esteem
Self-esteem is confidence in one's own worth or abilities. Self-esteem encompasses beliefs about oneself (for example, "I am loved", "I am worthy") as well as emotional states, such as triumph, despair, pride, and shame. Smith and Mackie (2007) d ...
, sense of dignity, confidence, and quality of life
Quality of life (QOL) is defined by the World Health Organization as "an individual's perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards ...
for people with HIV/AIDS. Anti-retroviral treatment may help people with HIV/AIDS work more, and may increase the chance that a person with HIV/AIDS will be employed (low-quality evidence).
By affecting mainly young adults, AIDS reduces the taxable population, in turn reducing the resources available for public expenditures such as education and health services not related to AIDS, resulting in increasing pressure on the state's finances and slower growth of the economy. This causes a slower growth of the tax base, an effect that is reinforced if there are growing expenditures on treating the sick, training (to replace sick workers), sick pay, and caring for AIDS orphans. This is especially true if the sharp increase in adult mortality shifts the responsibility from the family to the government in caring for these orphans.
At the household level, AIDS causes both loss of income and increased spending on healthcare. A study in Côte d'Ivoire
Ivory Coast, also known as Côte d'Ivoire, officially the Republic of Côte d'Ivoire, is a country on the southern coast of West Africa. Its capital is Yamoussoukro, in the centre of the country, while its largest city and economic centre ...
showed that households having a person with HIV/AIDS spent twice as much on medical expenses as other households. This additional expenditure also leaves less income to spend on education and other personal or family investment.
Religion and AIDS
The topic of religion and AIDS has become highly controversial, primarily because some religious authorities have publicly declared their opposition to the use of condoms. The religious approach to prevent the spread of AIDS, according to a report by American health expert Matthew Hanley titled ''The Catholic Church and the Global AIDS Crisis'', argues that cultural changes are needed, including a re-emphasis on fidelity within marriage and sexual abstinence outside of it. Some religious organizations have claimed that prayer can cure HIV/AIDS. In 2011, the BBC reported that some churches in London were claiming that prayer would cure AIDS, and the Hackney-based Centre for the Study of Sexual Health and HIV reported that several people stopped taking their medication, sometimes on the direct advice of their pastor, leading to many deaths. TheSynagogue Church Of All Nations
The Synagogue Church Of All Nations (SCOAN) is a charismatic Christian megachurch located in Lagos, Nigeria.
History
T. B. Joshua wrote that in a heavenly vision he received 'divine anointing' and a covenant from God to start his ministry i ...
advertised an "anointing water" to promote God's healing, although the group denies advising people to stop taking medication.
Media portrayal
One of the first high-profile cases of AIDS was the American gay actorRock Hudson
Rock Hudson (born Roy Harold Scherer Jr.; November 17, 1925 – October 2, 1985) was an American actor. One of the most popular movie stars of his time, he had a screen career spanning more than three decades. A prominent heartthrob in the Gold ...
. He had been diagnosed during 1984, announced that he had had the virus on July 25, 1985, and died a few months later on October 2, 1985. Another notable British casualty of AIDS that year was Nicholas Eden
Nicholas Eden, 2nd Earl of Avon, OBE Territorial Decoration, TD Deputy Lieutenant, DL (3 October 1930 – 17 August 1985), styled Viscount Eden between 1961 and 1977, was a British Army officer and, later, a Conservative Party (UK), Conservativ ...
, a gay politician and son of the late prime minister Anthony Eden
Robert Anthony Eden, 1st Earl of Avon, (12 June 1897 – 14 January 1977) was a British Conservative Party politician who served as Prime Minister of the United Kingdom from 1955 until his resignation in 1957.
Achieving rapid promo ...
. On November 24, 1991, the virus claimed the life of British rock star Freddie Mercury, lead singer of the band Queen
Queen or QUEEN may refer to:
Monarchy
* Queen regnant, a female monarch of a Kingdom
** List of queens regnant
* Queen consort, the wife of a reigning king
* Queen dowager, the widow of a king
* Queen mother, a queen dowager who is the mother ...
, who died from an AIDS-related illness having only revealed the diagnosis on the previous day.
One of the first high-profile heterosexual cases of the virus was American tennis player Arthur Ashe
Arthur Robert Ashe Jr. (July 10, 1943 – February 6, 1993) was an American professional tennis player who won three Grand Slam singles titles. He started to play tennis at six years old. He was the first black player selected to the Un ...
. He was diagnosed as HIV-positive on August 31, 1988, having contracted the virus from blood transfusions during heart surgery earlier in the 1980s. Further tests within 24 hours of the initial diagnosis revealed that Ashe had AIDS, but he did not tell the public about his diagnosis until April 1992. He died as a result on February 6, 1993, aged 49.
Therese Frare's photograph of gay activist David Kirby, as he lay dying from AIDS while surrounded by family, was taken in April 1990. ''Life
Life is a quality that distinguishes matter that has biological processes, such as signaling and self-sustaining processes, from that which does not, and is defined by the capacity for growth, reaction to stimuli, metabolism, energy ...
'' magazine said the photo became the one image "most powerfully identified with the HIV/AIDS epidemic." The photo was displayed in ''Life'', was the winner of the World Press Photo, and acquired worldwide notoriety after being used in a United Colors of Benetton
Benetton Group S.r.l. () is a global fashion brand based in Ponzano Veneto, Italy, founded in 1965. Benetton Group has a network of about 5,000 stores worldwide. It is a wholly owned subsidiary of the Benetton family's holding company Edizio ...
advertising campaign in 1992.
Many famous artists and AIDS activists such as Larry Kramer
Laurence David Kramer (June 25, 1935May 27, 2020) was an American playwright, author, film producer, public health advocate, and gay rights activist. He began his career rewriting scripts while working for Columbia Pictures, which led him to Lo ...
, Diamanda Galás and Rosa von Praunheim campaign for AIDS education and the rights of those affected. These artists worked with various media formats.
Criminal transmission
Criminal transmission of HIV is the intentional or reckless infection of a person with the human immunodeficiency virus (HIV). Some countries or jurisdictions, including some areas of the United States, have laws that criminalize HIV transmission or exposure. Others may charge the accused under laws enacted before the HIV pandemic. In 1996, Ugandan-born CanadianJohnson Aziga
Johnson Aziga (born 1956) is a Ugandan-born Canadian man formerly residing in Hamilton, Ontario, Canada, notable as the first person to be charged and convicted of first-degree murder in Canada for spreading HIV, after two women whom he had infecte ...
was diagnosed with HIV; he subsequently had unprotected sex with eleven women without disclosing his diagnosis. By 2003, seven had contracted HIV; two died from complications related to AIDS. Aziga was convicted of first-degree murder
Murder is the unlawful killing of another human without justification or valid excuse, especially the unlawful killing of another human with malice aforethought. ("The killing of another person without justification or excuse, especially t ...
and sentenced to life imprisonment
Life imprisonment is any sentence of imprisonment for a crime under which convicted people are to remain in prison for the rest of their natural lives or indefinitely until pardoned, paroled, or otherwise commuted to a fixed term. Crimes fo ...
.
Misconceptions
There are manymisconceptions about HIV and AIDS
The spread of HIV/AIDS has affected millions of people worldwide; AIDS is considered a pandemic. The World Health Organization (WHO) estimated that in 2016 there were 36.7 million people worldwide living with HIV/AIDS, with 1.8 million n ...
. Three misconceptions are that AIDS can spread through casual contact, that sexual intercourse with a virgin will cure AIDS, and that HIV can infect only gay men and drug users. In 2014, some among the British public wrongly thought one could get HIV from kissing (16%), sharing a glass (5%), spitting (16%), a public toilet seat (4%), and coughing or sneezing (5%). Other misconceptions are that any act of anal intercourse between two uninfected gay men can lead to HIV infection, and that open discussion of HIV and homosexuality in schools will lead to increased rates of AIDS.
A small group of individuals continue to dispute the connection between HIV and AIDS, the existence of HIV itself, or the validity of HIV testing and treatment methods. These claims, known as AIDS denialism, have been examined and rejected by the scientific community. However, they have had a significant political impact, particularly in South Africa, where the government's official embrace of AIDS denialism (1999–2005) was responsible for its ineffective response to that country's AIDS epidemic, and has been blamed for hundreds of thousands of avoidable deaths and HIV infections.
Several discredited conspiracy theories have held that HIV was created by scientists, either inadvertently or deliberately. Operation INFEKTION was a worldwide Soviet active measures operation to spread the claim that the United States had created HIV/AIDS. Surveys show that a significant number of people believed—and continue to believe—in such claims.
At the peak of the HIV/AIDS outbreak, there was also misinformation spread from some governmental institutions. For example, Anthony Fauci
Anthony Stephen Fauci (; born December 24, 1940) is an American physician-scientist and immunologist serving as the director of the National Institute of Allergy and Infectious Diseases (NIAID) and the chief medical advisor to the preside ...
, head of the National Institute of Allergy and Infectious Diseases during the AIDS outbreak, stated in the context of a conversation about childhood infections, “if the close contact of a child is a household contact, perhaps there will be a certain number of cases of individuals who are just living with and in close contact with someone with AIDS, or at risk of AIDS, who does not necessarily have to have intimate sexual contact or share a needle, but just the ordinary close contact that one sees in normal interpersonal relations.” This and similar statements made by governmental agencies potentially fueled the unfounded fear that the public had that AIDS could be spread by ordinary close contact rather than through sexual or fluid transmission as is most commonly the case.
Research
HIV/AIDS research includes all medical research which attempts to prevent, treat, or cure HIV/AIDS, along with fundamental research about the nature of HIV as an infectious agent, and about AIDS as the disease caused by HIV. Many governments and research institutions participate in HIV/AIDS research. This research includes behavioralhealth interventions
A public health intervention is any effort or policy that attempts to improve mental and physical health on a population level. Public health interventions may be run by a variety of organizations, including governmental health departments and ...
such as sex education
Sex education, also known as sexual education, sexuality education or sex ed, is the instruction of issues relating to human sexuality, including emotional relations and responsibilities, human sexual anatomy, sexual activity, sexual reproduc ...
, and drug development, such as research into microbicides for sexually transmitted diseases
Microbicides for sexually transmitted diseases are pharmacologic agents and chemical substances that are capable of killing or destroying certain microorganisms that commonly cause human infection (for example, the human immunodeficiency virus) ...
, HIV vaccines, and antiretroviral drugs. Other medical research areas include the topics of pre-exposure prophylaxis, post-exposure prophylaxis, and circumcision and HIV. Public health officials, researchers, and programs can gain a more comprehensive picture of the barriers they face, and the efficacy of current approaches to HIV treatment and prevention, by tracking standard HIV indicators. Use of common indicators is an increasing focus of development organizations and researchers.
References
External links
*UNAIDS
– Joint United Nations Program on HIV/AIDS
HIVinfo
– Information on HIV/AIDS treatment, prevention, and research, U.S. Department of Health and Human Services
2018 Recommendations of the International Antiviral Society
{{DEFAULTSORT:HIV AIDS 1981 in biology Articles containing video clips Health disasters Pandemics Slow virus diseases
Aids
Human immunodeficiency virus infection and acquired immunodeficiency syndrome (HIV/AIDS) is a spectrum of conditions caused by infection with the human immunodeficiency virus (HIV), a retrovirus. Following initial infection an individual ma ...
Wikipedia medicine articles ready to translate (full)
Wikipedia infectious disease articles ready to translate