placenta on:
[Wikipedia]
[Google]
[Amazon]
The placenta (: placentas or placentae) is a temporary embryonic and later fetal organ that begins developing from the blastocyst shortly after implantation. It plays critical roles in facilitating nutrient, gas, and waste exchange between the physically separate maternal and fetal circulations, and is an important endocrine organ, producing
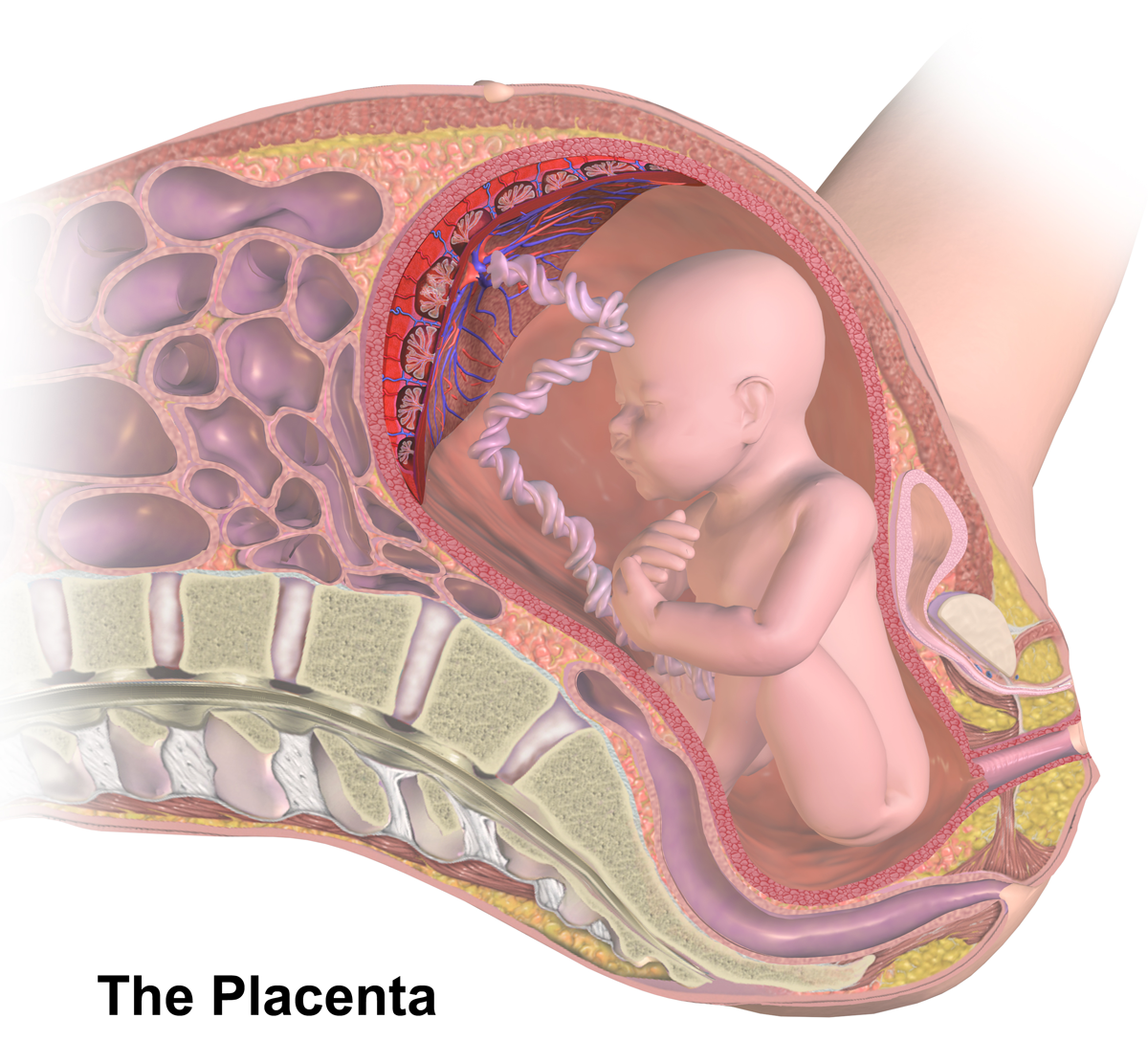
 The placenta begins to develop upon implantation of the blastocyst into the maternal endometrium, very early on in pregnancy at about week 4.
The outer layer of the late blastocyst, is formed of
The placenta begins to develop upon implantation of the blastocyst into the maternal endometrium, very early on in pregnancy at about week 4.
The outer layer of the late blastocyst, is formed of


File:Human placenta baby side.jpg , Human placenta immediately post birth.
File:Gray30.png, Fetus of about 8 weeks, enclosed in the amnion. Magnified a little over two diameters.
File:Placenta with fetal membranes.jpg, Placenta with attached fetal membranes, ruptured at the margin at the left in the image
File:CMV placentitis1.jpg,
The placenta-specific proteome
a
the Human Protein Atlas
gynob.com, with quotes from Williams Obstetrics, 18th Edition, F. Gary Cunningham, M.D., Paul C. MacDonald, M.D., Norman F. Grant, M.D., Appleton & Lange, Publishers. {{Authority control Vertebrate developmental biology Embryology of cardiovascular system Organs (anatomy) Reproductive system Microbiomes Human female endocrine system
hormones
A hormone (from the Greek participle , "setting in motion") is a class of signaling molecules in multicellular organisms that are sent to distant organs or tissues by complex biological processes to regulate physiology and behavior. Hormones a ...
that regulate both maternal and fetal physiology
Physiology (; ) is the science, scientific study of function (biology), functions and mechanism (biology), mechanisms in a life, living system. As a branches of science, subdiscipline of biology, physiology focuses on how organisms, organ syst ...
during pregnancy
Pregnancy is the time during which one or more offspring gestation, gestates inside a woman's uterus. A multiple birth, multiple pregnancy involves more than one offspring, such as with twins.
Conception (biology), Conception usually occurs ...
. The placenta connects to the fetus via the umbilical cord
In Placentalia, placental mammals, the umbilical cord (also called the navel string, birth cord or ''funiculus umbilicalis'') is a conduit between the developing embryo or fetus and the placenta. During prenatal development, the umbilical cord i ...
, and on the opposite aspect to the maternal uterus
The uterus (from Latin ''uterus'', : uteri or uteruses) or womb () is the hollow organ, organ in the reproductive system of most female mammals, including humans, that accommodates the embryonic development, embryonic and prenatal development, f ...
in a species
A species () is often defined as the largest group of organisms in which any two individuals of the appropriate sexes or mating types can produce fertile offspring, typically by sexual reproduction. It is the basic unit of Taxonomy (biology), ...
-dependent manner. In humans, a thin layer of maternal decidual ( endometrial) tissue comes away with the placenta when it is expelled from the uterus following birth (sometimes incorrectly referred to as the 'maternal part' of the placenta). Placentas are a defining characteristic of placental mammals, but are also found in marsupials and some non-mammals with varying levels of development.
Mammalian
A mammal () is a vertebrate animal of the Class (biology), class Mammalia (). Mammals are characterised by the presence of milk-producing mammary glands for feeding their young, a broad neocortex region of the brain, fur or hair, and three ...
placentas probably first evolved about 150 million to 200 million years ago. The protein syncytin, found in the outer barrier of the placenta (the syncytiotrophoblast) between mother and fetus, has a certain RNA signature in its genome that has led to the hypothesis that it originated from an ancient retrovirus: essentially a virus
A virus is a submicroscopic infectious agent that replicates only inside the living Cell (biology), cells of an organism. Viruses infect all life forms, from animals and plants to microorganisms, including bacteria and archaea. Viruses are ...
that helped pave the transition from egg-laying to live-birth.
The word ''placenta'' comes from the Latin
Latin ( or ) is a classical language belonging to the Italic languages, Italic branch of the Indo-European languages. Latin was originally spoken by the Latins (Italic tribe), Latins in Latium (now known as Lazio), the lower Tiber area aroun ...
word for a type of cake, from Greek πλακόεντα/πλακοῦντα ''plakóenta/plakoúnta'', accusative of πλακόεις/πλακούς ''plakóeis/plakoús'', "flat, slab-like", with reference to its round, flat appearance in humans. The classical plural is ''placentae'', but the form ''placentas'' is more common in modern English.
Evolution and phylogenetic diversity
The placenta has evolved independently multiple times, probably starting infish
A fish (: fish or fishes) is an aquatic animal, aquatic, Anamniotes, anamniotic, gill-bearing vertebrate animal with swimming fish fin, fins and craniate, a hard skull, but lacking limb (anatomy), limbs with digit (anatomy), digits. Fish can ...
, where it originated multiple times, including the genus '' Poeciliopsis.'' Placentation has also evolved in some reptile
Reptiles, as commonly defined, are a group of tetrapods with an ectothermic metabolism and Amniotic egg, amniotic development. Living traditional reptiles comprise four Order (biology), orders: Testudines, Crocodilia, Squamata, and Rhynchocepha ...
s.
The mammalian placenta evolved more than 100 million years ago and was a critical factor in the explosive diversification of placental mammals. Although all mammalian placentas have the same functions, there are important differences in structure and function in different groups of mammals. For example, human, bovine, equine and canine placentas are very different at both the gross and the microscopic levels. Placentas of these species also differ in their ability to provide maternal immunoglobulins to the fetus.
Structure
Placental mammals, including humans, have a chorioallantoic placenta that forms from the chorion and allantois. In humans, the placenta averages 22 cm (9 inch) in length and 2–2.5 cm (0.8–1 inch) in thickness, with the center being the thickest, and the edges being the thinnest. It typically weighs approximately 500 grams (just over 1 lb). It has a dark reddish-blue or crimson color. It connects to the fetus by anumbilical cord
In Placentalia, placental mammals, the umbilical cord (also called the navel string, birth cord or ''funiculus umbilicalis'') is a conduit between the developing embryo or fetus and the placenta. During prenatal development, the umbilical cord i ...
of approximately 55–60 cm (22–24 inch) in length, which contains two umbilical arteries and one umbilical vein. The umbilical cord inserts into the chorionic plate (has an eccentric attachment). Vessels branch out over the surface of the placenta and further divide to form a network covered by a thin layer of cells. This results in the formation of villous tree structures. On the maternal side, these villous tree structures are grouped into lobules called cotyledons. In humans, the placenta usually has a disc shape, but size varies vastly between different mammalian species.
The placenta occasionally takes a form in which it comprises several distinct parts connected by blood vessels. The parts, called lobes, may number two, three, four, or more. Such placentas are described as bilobed/bilobular/bipartite, trilobed/trilobular/tripartite, and so on. If there is a clearly discernible main lobe and auxiliary lobe, the latter is called a ''succenturiate placenta''. Sometimes the blood vessels connecting the lobes get in the way of fetal presentation during labor, which is called '' vasa previa''.
Gene and protein expression
About 20,000 protein coding genes are expressed in human cells and 70% of these genes are expressed in the normal mature placenta. Some 350 of these genes are more specifically expressed in the placenta and fewer than 100 genes are highly placenta specific. The corresponding specific proteins are mainly expressed introphoblast
The trophoblast (from Greek language, Greek : to feed; and : germinator) is the outer layer of cells of the blastocyst. Trophoblasts are present four days after Human fertilization, fertilization in humans. They provide nutrients to the embryo an ...
s and have functions related to pregnancy
Pregnancy is the time during which one or more offspring gestation, gestates inside a woman's uterus. A multiple birth, multiple pregnancy involves more than one offspring, such as with twins.
Conception (biology), Conception usually occurs ...
. Examples of proteins with elevated expression in placenta compared to other organs and tissues are PEG10 and the cancer testis antigen PAGE4 and expressed in cytotrophoblasts, CSH1 and KISS1 expressed in syncytiotrophoblasts, and PAPPA2 and PRG2 expressed in extravillous trophoblasts.
Physiology
Development

trophoblast
The trophoblast (from Greek language, Greek : to feed; and : germinator) is the outer layer of cells of the blastocyst. Trophoblasts are present four days after Human fertilization, fertilization in humans. They provide nutrients to the embryo an ...
s, cells that form the outer layer of the placenta. This outer layer is divided into two further layers: the underlying cytotrophoblast layer and the overlying syncytiotrophoblast layer. The syncytiotrophoblast is a multinucleated continuous cell layer that covers the surface of the placenta. It forms as a result of differentiation and fusion of the underlying cytotrophoblasts, a process that continues throughout placental development. The syncytiotrophoblast contributes to the barrier function of the placenta.
The placenta grows throughout pregnancy
Pregnancy is the time during which one or more offspring gestation, gestates inside a woman's uterus. A multiple birth, multiple pregnancy involves more than one offspring, such as with twins.
Conception (biology), Conception usually occurs ...
. Development of the maternal blood supply to the placenta is complete by the end of the first trimester of pregnancy week 14 (DM).
Placental circulation

Maternal placental circulation
In preparation for implantation of the blastocyst, the endometrium undergoes decidualization. Spiral arteries in the decidua are remodeled so that they become less convoluted and their diameter is increased. The increased diameter and straighter flow path both act to increase maternal blood flow to the placenta. There is relatively high pressure as the maternal blood fills intervillous space through these spiral arteries which bathe the fetal villi in blood, allowing an exchange of gases to take place. In humans and other hemochorial placentals, the maternal blood comes into direct contact with the fetal chorion, though no fluid is exchanged. As the pressure decreases between pulses, the deoxygenated blood flows back through the endometrial veins. Maternal blood flow begins between days 5–12, and is approximately 600–700 ml/min at term.Fetoplacental circulation
Deoxygenated fetal blood passes through umbilical arteries to the placenta. At the junction of umbilical cord and placenta, the umbilical arteries branch radially to form chorionic arteries. Chorionic arteries, in turn, branch into cotyledon arteries. In the villi, these vessels eventually branch to form an extensive arterio-capillary-venous system, bringing the fetal blood extremely close to the maternal blood; but no intermingling of fetal and maternal blood occurs ("placental barrier"). Endothelin and prostanoids cause vasoconstriction in placental arteries, while nitric oxide causes vasodilation. On the other hand, there is no neural vascular regulation, and catecholamines have only little effect. The fetoplacental circulation is vulnerable to persistent hypoxia or intermittent hypoxia and reoxygenation, which can lead to generation of excessive free radicals. This may contribute topre-eclampsia
Pre-eclampsia is a multi-system disorder specific to pregnancy, characterized by the new onset of hypertension, high blood pressure and often a significant amount of proteinuria, protein in the urine or by the new onset of high blood pressure a ...
and other pregnancy complications. It is proposed that melatonin plays a role as an antioxidant in the placenta.
This begins at day 17–22.
Birth
Placental expulsion begins as a physiological separation from the wall of the uterus. The period from just after the child is born until just after the placenta is expelled is called the "third stage of labor". Placental expulsion can be managed actively, for example by givingoxytocin
Oxytocin is a peptide hormone and neuropeptide normally produced in the hypothalamus and released by the posterior pituitary. Present in animals since early stages of evolution, in humans it plays roles in behavior that include Human bonding, ...
via intramuscular injection followed by cord traction to assist in delivering the placenta. Alternatively, it can be managed expectantly, allowing the placenta to be expelled without medical assistance. Blood loss and the risk of postpartum bleeding may be reduced in women offered active management of the third stage of labour, however there may be adverse effects and more research is necessary.
The habit is to cut the cord immediately after birth, but it may be no medical reason to do this; on the contrary, not cutting the cord could sometimes help the baby in its adaptation to extrauterine life, for preterm infants.
Microbiome
The placenta is traditionally thought to be sterile, but recent research suggests that a resident, non-pathogenic, and diverse population of microorganisms may be present in healthy tissue. However, whether these microbes exist or are clinically important is highly controversial and is the subject of active research.Physiology of placenta
Nutrition and gas exchange
The placenta intermediates the transfer of nutrients between mother and fetus. The perfusion of the intervillous spaces of the placenta with maternal blood allows the transfer of nutrients and oxygen from the mother to the fetus and the transfer of waste products andcarbon dioxide
Carbon dioxide is a chemical compound with the chemical formula . It is made up of molecules that each have one carbon atom covalent bond, covalently double bonded to two oxygen atoms. It is found in a gas state at room temperature and at norma ...
back from the fetus to the maternal blood. Nutrient transfer to the fetus can occur via both active and passive transport. Placental nutrient metabolism was found to play a key role in limiting the transfer of some nutrients. Adverse pregnancy situations, such as those involving maternal diabetes or obesity
Obesity is a medical condition, considered by multiple organizations to be a disease, in which excess Adipose tissue, body fat has accumulated to such an extent that it can potentially have negative effects on health. People are classifi ...
, can increase or decrease levels of nutrient transporters in the placenta potentially resulting in overgrowth or restricted growth of the fetus.
Excretion
Waste products excreted from the fetus such asurea
Urea, also called carbamide (because it is a diamide of carbonic acid), is an organic compound with chemical formula . This amide has two Amine, amino groups (–) joined by a carbonyl functional group (–C(=O)–). It is thus the simplest am ...
, uric acid
Uric acid is a heterocyclic compound of carbon, nitrogen, oxygen, and hydrogen with the Chemical formula, formula C5H4N4O3. It forms ions and salts known as urates and acid urates, such as ammonium acid urate. Uric acid is a product of the meta ...
, and creatinine are transferred to the maternal blood by diffusion
Diffusion is the net movement of anything (for example, atoms, ions, molecules, energy) generally from a region of higher concentration to a region of lower concentration. Diffusion is driven by a gradient in Gibbs free energy or chemical p ...
across the placenta.
Immunity
The placenta functions as a selective barrier between maternal and fetal cells, preventing maternal blood, proteins and microbes (includingbacteria
Bacteria (; : bacterium) are ubiquitous, mostly free-living organisms often consisting of one Cell (biology), biological cell. They constitute a large domain (biology), domain of Prokaryote, prokaryotic microorganisms. Typically a few micr ...
and most viruses
A virus is a submicroscopic infectious agent that replicates only inside the living cells of an organism. Viruses infect all life forms, from animals and plants to microorganisms, including bacteria and archaea. Viruses are found in almo ...
) from crossing the maternal-fetal barrier.
Deterioration in placental functioning, referred to as placental insufficiency, may be related to mother-to-child transmission of some infectious diseases.
A very small number of viruses including '' rubella virus'', '' Zika virus'' and '' cytomegalovirus'' (CMV) can travel across the placental barrier, generally taking advantage of conditions at certain gestational periods as the placenta develops. CMV and Zika travel from the maternal bloodstream via placental cells to the fetal bloodstream.
Beginning as early as 13 weeks of gestation, and increasing linearly, with the largest transfer occurring in the third trimester, IgG antibodies can pass through the human placenta, providing protection to the fetus ''in utero''.
This passive immunity lingers for several months after birth, providing the newborn with a carbon copy of the mother's long-term humoral immunity to see the infant through the crucial first months of extrauterine life. IgM antibodies, because of their larger size, cannot cross the placenta, one reason why infections acquired during pregnancy can be particularly hazardous for the fetus.
Hormonal regulation
* The first hormone released by the placenta is called the human chorionic gonadotropin (hCG) hormone. This is responsible for stopping the process at the end of menses when the corpus luteum ceases activity and atrophies. If hCG did not interrupt this process, it would lead to spontaneous abortion of the fetus. The corpus luteum also produces and releases progesterone andestrogen
Estrogen (also spelled oestrogen in British English; see spelling differences) is a category of sex hormone responsible for the development and regulation of the female reproductive system and secondary sex characteristics. There are three ...
, and hCG stimulates it to increase the amount that it releases. hCG is the indicator of pregnancy that pregnancy tests look for. These tests will work when menses has not occurred or after implantation has happened on days seven to ten. hCG may also have an anti-antibody effect, protecting it from being rejected by the mother's body. hCG also assists the male fetus by stimulating the testes to produce testosterone, which is the hormone needed to allow the sex organs of the male to grow.
* Progesterone helps the embryo implant by assisting passage through the fallopian tubes. It also affects the fallopian tubes and the uterus
The uterus (from Latin ''uterus'', : uteri or uteruses) or womb () is the hollow organ, organ in the reproductive system of most female mammals, including humans, that accommodates the embryonic development, embryonic and prenatal development, f ...
by stimulating an increase in secretions necessary for fetal nutrition. Progesterone, like hCG, is necessary to prevent spontaneous abortion because it prevents contractions of the uterus and is necessary for implantation.
* Estrogen
Estrogen (also spelled oestrogen in British English; see spelling differences) is a category of sex hormone responsible for the development and regulation of the female reproductive system and secondary sex characteristics. There are three ...
is a crucial hormone in the process of proliferation. This involves the enlargement of the breasts and uterus, allowing for growth of the fetus and production of milk. Estrogen is also responsible for increased blood supply towards the end of pregnancy through vasodilation. The levels of estrogen during pregnancy can increase so that they are thirty times what a non-pregnant woman mid-cycles estrogen level would be.
* Human placental lactogen (hPL) is a hormone used in pregnancy to develop fetal metabolism and general growth and development. Human placental lactogen works with growth hormone to stimulate insulin-like growth factor production and regulating intermediary metabolism. In the fetus, hPL acts on lactogenic receptors to modulate embryonic development, metabolism and stimulate production of IGF, insulin
Insulin (, from Latin ''insula'', 'island') is a peptide hormone produced by beta cells of the pancreatic islets encoded in humans by the insulin (''INS)'' gene. It is the main Anabolism, anabolic hormone of the body. It regulates the metabol ...
, surfactant and adrenocortical hormones. hPL values increase with multiple pregnancies, intact molar pregnancy, diabetes and Rh incompatibility. They are decreased with toxemia, choriocarcinoma, and Placental insufficiency.
Immunological barrier
The placenta and fetus may be regarded as a foreign body inside the mother and must be protected from the normal immune response of the mother that would cause it to be rejected. The placenta and fetus are thus treated as sites of immune privilege, with immune tolerance. For this purpose, the placenta uses several mechanisms : * It secretes neurokinin B-containing phosphocholine molecules. This is the same mechanism used by parasiticnematode
The nematodes ( or ; ; ), roundworms or eelworms constitute the phylum Nematoda. Species in the phylum inhabit a broad range of environments. Most species are free-living, feeding on microorganisms, but many are parasitic. Parasitic worms (h ...
s to avoid detection by the immune system of their host.
* There is presence of small lymphocytic suppressor cells in the fetus that inhibit maternal cytotoxic T cells by inhibiting the response to interleukin 2.
However, the placental barrier is not the sole means of evading the immune system, as foreign fetal cells also persist in the maternal circulation, on the other side of the placental barrier.
DNA methylation
Thetrophoblast
The trophoblast (from Greek language, Greek : to feed; and : germinator) is the outer layer of cells of the blastocyst. Trophoblasts are present four days after Human fertilization, fertilization in humans. They provide nutrients to the embryo an ...
is the outer layer of cells of the blastocyst (see day 9 in Figure, above, showing the initial stages of human embryogenesis). Placental trophoblast cells have a unique genome-wide DNA methylation pattern determined by de novo methyltransferases during embryogenesis
An embryo ( ) is the initial stage of development for a multicellular organism. In organisms that reproduce sexually, embryonic development is the part of the life cycle that begins just after fertilization of the female egg cell by the male ...
. This methylation pattern is principally required to regulate placental development and function, which in turn is critical for embryo survival.
Other
The placenta also provides a reservoir of blood for the fetus, delivering blood to it in case of hypotension and vice versa, comparable to a capacitor.
Clinical significance
Numerous pathologies can affect the placenta. * Placenta accreta, when the placenta implants too deeply, all the way to the actual muscle of uterine wall (without penetrating it) * Placenta praevia, when the placement of the placenta is too close to or blocks thecervix
The cervix (: cervices) or cervix uteri is a dynamic fibromuscular sexual organ of the female reproductive system that connects the vagina with the uterine cavity. The human female cervix has been documented anatomically since at least the time ...
* Placental abruption, premature detachment of the placenta
* Placentitis
Placentitis is an inflammation of the placenta. The main forms of placentitis are:
*Villitis, inflammation of chorionic villi.
*Intervillositis, inflammation of the intervillous space.
It may be caused by vertically transmitted infections.
Beca ...
, inflammation of the placenta, such as by TORCH infections.
Society and culture
The placenta often plays an important role in variousculture
Culture ( ) is a concept that encompasses the social behavior, institutions, and Social norm, norms found in human societies, as well as the knowledge, beliefs, arts, laws, Social norm, customs, capabilities, Attitude (psychology), attitudes ...
s, with many societies conducting rituals regarding its disposal. In the Western world
The Western world, also known as the West, primarily refers to various nations and state (polity), states in Western Europe, Northern America, and Australasia; with some debate as to whether those in Eastern Europe and Latin America also const ...
, the placenta is most often incinerated.
Some cultures bury the placenta for various reasons. The Māori of New Zealand
New Zealand () is an island country in the southwestern Pacific Ocean. It consists of two main landmasses—the North Island () and the South Island ()—and List of islands of New Zealand, over 600 smaller islands. It is the List of isla ...
traditionally bury the placenta from a newborn child to emphasize the relationship between humans and the earth. Likewise, the Navajo bury the placenta and umbilical cord at a specially chosen site, particularly if the baby dies during birth. In Cambodia
Cambodia, officially the Kingdom of Cambodia, is a country in Southeast Asia on the Mainland Southeast Asia, Indochinese Peninsula. It is bordered by Thailand to the northwest, Laos to the north, and Vietnam to the east, and has a coastline ...
and Costa Rica
Costa Rica, officially the Republic of Costa Rica, is a country in Central America. It borders Nicaragua to the north, the Caribbean Sea to the northeast, Panama to the southeast, and the Pacific Ocean to the southwest, as well as Maritime bo ...
, burial of the placenta is believed to protect and ensure the health of the baby and the mother. If a mother dies in childbirth, the Aymara of Bolivia
Bolivia, officially the Plurinational State of Bolivia, is a landlocked country located in central South America. The country features diverse geography, including vast Amazonian plains, tropical lowlands, mountains, the Gran Chaco Province, w ...
bury the placenta in a secret place so that the mother's spirit will not return to claim her baby's life.
The placenta is believed by some communities to have power over the lives of the baby or its parents. The Kwakiutl of British Columbia
British Columbia is the westernmost Provinces and territories of Canada, province of Canada. Situated in the Pacific Northwest between the Pacific Ocean and the Rocky Mountains, the province has a diverse geography, with rugged landscapes that ...
bury girls' placentas to give the girl skill in digging clams, and expose boys' placentas to ravens to encourage future prophet
In religion, a prophet or prophetess is an individual who is regarded as being in contact with a divinity, divine being and is said to speak on behalf of that being, serving as an intermediary with humanity by delivering messages or teachings ...
ic visions. In Turkey
Turkey, officially the Republic of Türkiye, is a country mainly located in Anatolia in West Asia, with a relatively small part called East Thrace in Southeast Europe. It borders the Black Sea to the north; Georgia (country), Georgia, Armen ...
, the proper disposal of the placenta and umbilical cord is believed to promote devoutness in the child later in life. In Transylvania
Transylvania ( or ; ; or ; Transylvanian Saxon dialect, Transylvanian Saxon: ''Siweberjen'') is a List of historical regions of Central Europe, historical and cultural region in Central Europe, encompassing central Romania. To the east and ...
and Japan
Japan is an island country in East Asia. Located in the Pacific Ocean off the northeast coast of the Asia, Asian mainland, it is bordered on the west by the Sea of Japan and extends from the Sea of Okhotsk in the north to the East China Sea ...
, interaction with a disposed placenta is thought to influence the parents' future fertility.
Several cultures believe the placenta to be or have been alive, often a relative of the baby. Nepal
Nepal, officially the Federal Democratic Republic of Nepal, is a landlocked country in South Asia. It is mainly situated in the Himalayas, but also includes parts of the Indo-Gangetic Plain. It borders the Tibet Autonomous Region of China Ch ...
ese think of the placenta as a friend of the baby; the orang Asli
The Orang Asli are a Homogeneity and heterogeneity, heterogeneous Indigenous peoples, indigenous population forming a national minority in Malaysia. They are the oldest inhabitants of Peninsular Malaysia.
As of 2017, the Orang Asli accounted f ...
and Malay populations in Malay Peninsula
The Malay Peninsula is located in Mainland Southeast Asia. The landmass runs approximately north–south, and at its terminus, it is the southernmost point of the Asian continental mainland. The area contains Peninsular Malaysia, Southern Tha ...
regard it as the baby's older sibling. Native Hawaiians believe that the placenta is a part of the baby, and traditionally plant it with a tree that can then grow alongside the child. Various cultures in Indonesia
Indonesia, officially the Republic of Indonesia, is a country in Southeast Asia and Oceania, between the Indian Ocean, Indian and Pacific Ocean, Pacific oceans. Comprising over List of islands of Indonesia, 17,000 islands, including Sumatra, ...
, such as Javanese and Malay, believe that the placenta has a spirit and needs to be buried outside the family house. Some Malays would bury the baby's placenta with a pencil (if it is a boy) or a needle and thread (if it is a girl).
In some cultures, the placenta is eaten, a practice known as human placentophagy. In some eastern cultures, such as China
China, officially the People's Republic of China (PRC), is a country in East Asia. With population of China, a population exceeding 1.4 billion, it is the list of countries by population (United Nations), second-most populous country after ...
, the dried placenta (''ziheche'' , literally "purple river car") is thought to be a healthful restorative and is sometimes used in preparations of traditional Chinese medicine
Traditional Chinese medicine (TCM) is an alternative medicine, alternative medical practice drawn from traditional medicine in China. A large share of its claims are pseudoscientific, with the majority of treatments having no robust evidence ...
and various health products. The practice of human placentophagy has become a more recent trend in western cultures and is not without controversy
Controversy (, ) is a state of prolonged public dispute or debate, usually concerning a matter of conflicting opinion or point of view. The word was coined from the Latin '' controversia'', as a composite of ''controversus'' – "turned in an op ...
; its practice being considered cannibalism is debated.
Some cultures have alternative uses for placenta that include the manufacturing of cosmetics, pharmaceuticals and food.
Additional images
Micrograph
A micrograph is an image, captured photographically or digitally, taken through a microscope or similar device to show a magnify, magnified image of an object. This is opposed to a macrograph or photomacrograph, an image which is also taken ...
of a placental infection
An infection is the invasion of tissue (biology), tissues by pathogens, their multiplication, and the reaction of host (biology), host tissues to the infectious agent and the toxins they produce. An infectious disease, also known as a transmis ...
( CMV placentitis)
File:CMV placentitis2.jpg, Micrograph of CMV placentitis
File:Placenta vasculature 3D power doppler 00001.gif, A 3D Power Doppler image of vasculature in 20-week placenta
File:2910 The Placenta-02.jpg, Schematic view of the placenta
File:Human placenta 01.JPG, Maternal side of a whole human placenta, just after birth
File:Human placenta 02.JPG, Fetal side of same placenta
File:Fetal side close-up of freshly delivered placenta.jpeg, Close-up of umbilical attachment to fetal side of freshly delivered placenta
File:Placenta weight by gestational age.svg, Placenta weight by gestational age
File:Ziheche.jpg, ''Ziheche'' (紫河车), dried human placenta used in traditional Chinese medicine
See also
* Caul * Choriovitelline placenta * Pregnancy in fish *Zygote
A zygote (; , ) is a eukaryote, eukaryotic cell (biology), cell formed by a fertilization event between two gametes.
The zygote's genome is a combination of the DNA in each gamete, and contains all of the genetic information of a new individ ...
References
External links
The placenta-specific proteome
a
the Human Protein Atlas
gynob.com, with quotes from Williams Obstetrics, 18th Edition, F. Gary Cunningham, M.D., Paul C. MacDonald, M.D., Norman F. Grant, M.D., Appleton & Lange, Publishers. {{Authority control Vertebrate developmental biology Embryology of cardiovascular system Organs (anatomy) Reproductive system Microbiomes Human female endocrine system