Deep venous thrombosis on:
[Wikipedia]
[Google]
[Amazon]
Deep vein thrombosis (DVT) is a type of
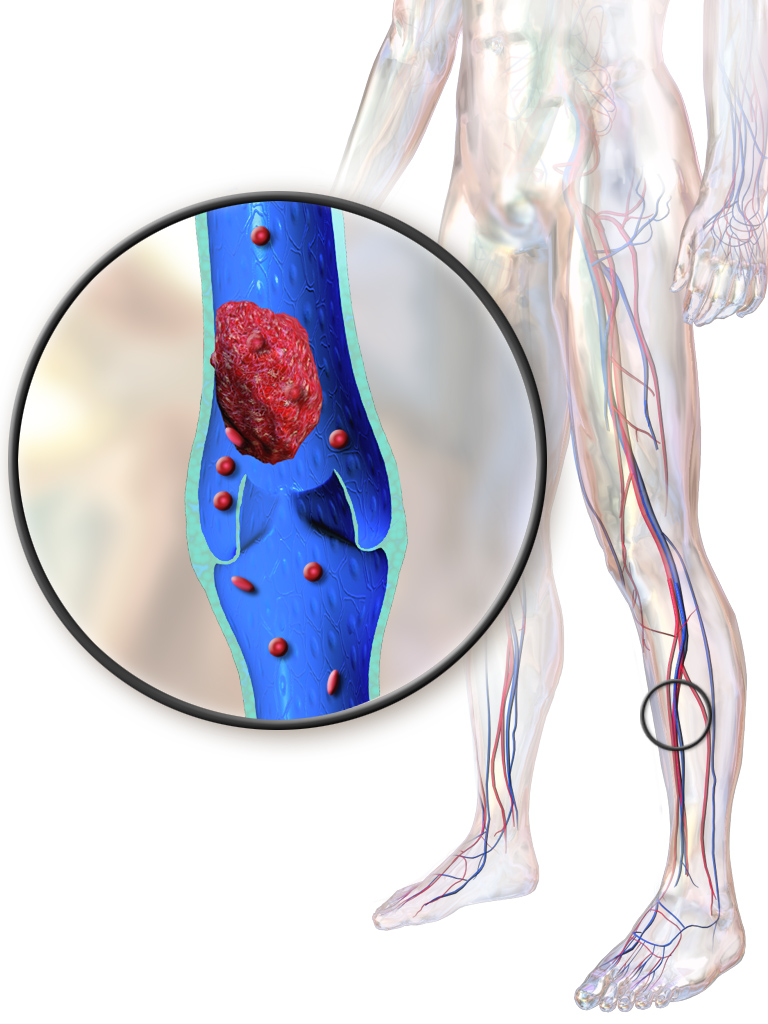
 Symptoms classically affect a leg and typically develop over hours or days, though they can develop suddenly or over a matter of weeks. The legs are primarily affected, with 4–10% of DVT occurring in the arms. Despite the signs and symptoms being highly variable, the typical symptoms are pain, swelling, and redness. However, these symptoms might not manifest in the lower limbs of those unable to walk. In those who are able to walk, DVT can reduce one's ability to do so. The pain can be described as throbbing and can worsen with weight-bearing, prompting one to bear more weight with the unaffected leg. Additional signs and symptoms include tenderness, pitting edema (''see image''), dilation of surface veins, warmth, discoloration, a "pulling sensation", and even cyanosis (a blue or purplish discoloration) with fever. DVT can also exist without causing any symptoms. Signs and symptoms help in determining the likelihood of DVT, but they are not used alone for diagnosis.
At times, DVT can cause symptoms in both arms or both legs, as with bilateral DVT. Rarely, a clot in the
Symptoms classically affect a leg and typically develop over hours or days, though they can develop suddenly or over a matter of weeks. The legs are primarily affected, with 4–10% of DVT occurring in the arms. Despite the signs and symptoms being highly variable, the typical symptoms are pain, swelling, and redness. However, these symptoms might not manifest in the lower limbs of those unable to walk. In those who are able to walk, DVT can reduce one's ability to do so. The pain can be described as throbbing and can worsen with weight-bearing, prompting one to bear more weight with the unaffected leg. Additional signs and symptoms include tenderness, pitting edema (''see image''), dilation of surface veins, warmth, discoloration, a "pulling sensation", and even cyanosis (a blue or purplish discoloration) with fever. DVT can also exist without causing any symptoms. Signs and symptoms help in determining the likelihood of DVT, but they are not used alone for diagnosis.
At times, DVT can cause symptoms in both arms or both legs, as with bilateral DVT. Rarely, a clot in the
File:SaddlePE.PNG, alt=A computed tomography image depicting PE in the pulmonary arteries, A CT image with red arrows indicating PE (grey) in the
 DVT and PE are the two manifestations of the cardiovascular disease venous thromboembolism (VTE). VTE can occur as DVT only, DVT with PE, or PE only. About two-thirds of VTE manifests as DVT only, with one-third manifesting as PE with or without DVT. VTE, along with superficial vein thrombosis, are common types of venous thrombosis.
DVT is classified as acute when the clots are developing or have recently developed, whereas chronic DVT persists more than 28 days. Differences between these two types of DVT can be seen with ultrasound. An episode of VTE after an initial one is classified as recurrent. Bilateral DVT refers to clots in both limbs while unilateral means only a single limb is affected.
DVT in the legs is proximal when above the knee and distal (or calf) when below the knee. DVT below the popliteal vein, a proximal vein behind the knee, is classified as distal
DVT and PE are the two manifestations of the cardiovascular disease venous thromboembolism (VTE). VTE can occur as DVT only, DVT with PE, or PE only. About two-thirds of VTE manifests as DVT only, with one-third manifesting as PE with or without DVT. VTE, along with superficial vein thrombosis, are common types of venous thrombosis.
DVT is classified as acute when the clots are developing or have recently developed, whereas chronic DVT persists more than 28 days. Differences between these two types of DVT can be seen with ultrasound. An episode of VTE after an initial one is classified as recurrent. Bilateral DVT refers to clots in both limbs while unilateral means only a single limb is affected.
DVT in the legs is proximal when above the knee and distal (or calf) when below the knee. DVT below the popliteal vein, a proximal vein behind the knee, is classified as distal
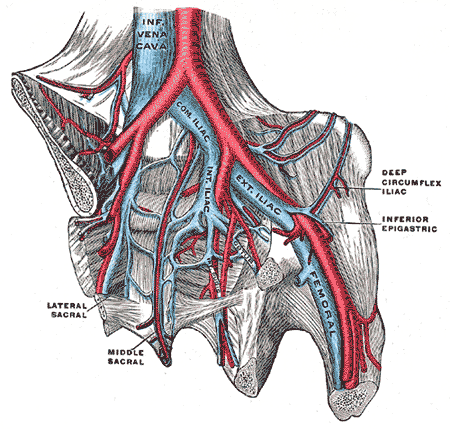
and has limited clinical significance compared to proximal DVT. Calf DVT makes up about half of DVTs. Iliofemoral DVT has been described as involving either the iliac or
 Traditionally, the three factors of
Traditionally, the three factors of  Dozens of genetic risk factors have been identified, and they account for approximately 50 to 60% of the variability in VTE rates. As such,
Dozens of genetic risk factors have been identified, and they account for approximately 50 to 60% of the variability in VTE rates. As such,
 Blood has a natural tendency to clot when blood vessels are damaged (
Blood has a natural tendency to clot when blood vessels are damaged ( In arterial thrombosis, blood vessel wall damage is required, as it initiates
In arterial thrombosis, blood vessel wall damage is required, as it initiates
DVTUS.PNG, An ultrasound with a blood clot visible in the left common femoral vein. (The common femoral vein is distal to the external iliac vein.)
Ultrasonography of deep vein thrombosis of the femoral vein -annotated.jpg,
"NICE Guideline 158: Venous thromboembolic diseases: diagnosis, management and thrombophilia testing
London, 26 March 2020. It is not recommended practice to obtain
"NICE Interventional procedures guidance 651: Percutaneous mechanical thrombectomy for acute deep vein thrombosis of the leg
London, 12 June 2019. Catheter-directed thrombolysis with thrombectomy against iliofemoral DVT has been associated with a reduction in the severity of post-thrombotic syndrome at an estimated cost-effectiveness ratio of about $138,000 per gained
File:Gray966.png, The first rib, which is removed in a first rib resection surgery, is labeled 1 in this image
File:A-case-of-Paget-Schroetter-syndrome-(PSS)-in-a-young-judo-tutor-a-case-report-13256 2016 848 Fig1 HTML.jpg, A venogram before catheter-directed thrombolysis for Paget–Schroetter syndrome, a rare and severe arm DVT shown here in a judo practitioner, with highly restricted blood flow shown in the vein
File:A-case-of-Paget-Schroetter-syndrome-(PSS)-in-a-young-judo-tutor-a-case-report-13256 2016 848 Fig2 HTML.jpg, After treatment with catheter-directed thrombolysis, blood flow in the axillary and subclavian vein were significantly improved. Afterwards, a first rib resection allowed decompression. This reduces the risk of recurrent DVT and other
 The placement of an
The placement of an
 Major orthopedic surgery—
Major orthopedic surgery—
 Travelling "is an often cited yet relatively uncommon" cause of VTE. Suggestions for at-risk long-haul travelers include calf exercises, frequent walking, and aisle seating in airplanes to ease walking. See section 6.0, Long-Distance Travel Graduated compression stockings have sharply reduced the levels of asymptomatic DVT in airline passengers, but the effect on symptomatic DVT, PE, or mortality is unknown, as none of the individuals studied developed these outcomes. However, graduated compression stockings are not suggested for long-haul travelers (>4 hours) without risk factors for VTE. Likewise, neither aspirin nor anticoagulants are suggested in the general population undertaking long-haul travel. Those with significant VTE risk factors undertaking long-haul travel are suggested to use either graduated compression stockings or LMWH for VTE prevention. If neither of these two methods are feasible, then aspirin is suggested.
Travelling "is an often cited yet relatively uncommon" cause of VTE. Suggestions for at-risk long-haul travelers include calf exercises, frequent walking, and aisle seating in airplanes to ease walking. See section 6.0, Long-Distance Travel Graduated compression stockings have sharply reduced the levels of asymptomatic DVT in airline passengers, but the effect on symptomatic DVT, PE, or mortality is unknown, as none of the individuals studied developed these outcomes. However, graduated compression stockings are not suggested for long-haul travelers (>4 hours) without risk factors for VTE. Likewise, neither aspirin nor anticoagulants are suggested in the general population undertaking long-haul travel. Those with significant VTE risk factors undertaking long-haul travel are suggested to use either graduated compression stockings or LMWH for VTE prevention. If neither of these two methods are feasible, then aspirin is suggested.
 Being on blood thinners because of DVT can be life-changing because it can prevent lifestyle activities such as contact or winter sports to prevent bleeding after potential injuries. Head injuries prompting brain bleeds are of particular concern. This has caused NASCAR driver
Being on blood thinners because of DVT can be life-changing because it can prevent lifestyle activities such as contact or winter sports to prevent bleeding after potential injuries. Head injuries prompting brain bleeds are of particular concern. This has caused NASCAR driver
 The book '' Sushruta Samhita'', an Ayurvedic text published around 600–900 BC, contains what has been cited as the first description of DVT. In 1271, DVT symptoms in the leg of a 20-year-old male were described in a French manuscript, which has been cited as the first case or the first Western reference to DVT.
In 1856, German physician and pathologist
The book '' Sushruta Samhita'', an Ayurvedic text published around 600–900 BC, contains what has been cited as the first description of DVT. In 1271, DVT symptoms in the leg of a 20-year-old male were described in a French manuscript, which has been cited as the first case or the first Western reference to DVT.
In 1856, German physician and pathologist  Multiple pharmacological therapies for DVT were introduced in the 20th century: oral anticoagulants in the 1940s, subcutaneous injections of LDUH in 1962 and subcutaneous injections of LMWH in 1982. 1974 was when vascular inflammation and venous thrombosis were first proposed to be interrelated. For around 50 years, a months-long warfarin (Coumadin) regimen was the mainstay of pharmacological treatment. To avoid the blood monitoring required with warfarin and the injections required by heparin and heparin-like medicines, direct oral anticoagulants (DOACs) were developed. In the late 2000s to early 2010s, DOACs—including rivaroxaban (Xarelto), apixaban (Eliquis), and dabigatran (Pradaxa)—came to the market. ''The New York Times'' described a "furious battle" among the three makers of these drugs "for the prescription pads of doctors".
Multiple pharmacological therapies for DVT were introduced in the 20th century: oral anticoagulants in the 1940s, subcutaneous injections of LDUH in 1962 and subcutaneous injections of LMWH in 1982. 1974 was when vascular inflammation and venous thrombosis were first proposed to be interrelated. For around 50 years, a months-long warfarin (Coumadin) regimen was the mainstay of pharmacological treatment. To avoid the blood monitoring required with warfarin and the injections required by heparin and heparin-like medicines, direct oral anticoagulants (DOACs) were developed. In the late 2000s to early 2010s, DOACs—including rivaroxaban (Xarelto), apixaban (Eliquis), and dabigatran (Pradaxa)—came to the market. ''The New York Times'' described a "furious battle" among the three makers of these drugs "for the prescription pads of doctors".
venous thrombosis
Venous thrombosis is blockage of a vein caused by a thrombus (blood clot). A common form of venous thrombosis is deep vein thrombosis (DVT), when a blood clot forms in the deep veins. If a thrombus breaks off (embolizes) and flows to the lungs to ...
involving the formation of a blood clot
A thrombus (plural thrombi), colloquially called a blood clot, is the final product of the blood coagulation step in hemostasis. There are two components to a thrombus: aggregated platelets and red blood cells that form a plug, and a mesh of ...
in a deep vein
A deep vein is a vein that is deep in the body. This contrasts with superficial veins that are close to the body's surface.
Deep veins are almost always beside an artery with the same name (e.g. the femoral vein is beside the femoral artery). ...
, most commonly in the legs or pelvis. A minority of DVTs occur in the arms. Symptoms can include pain, swelling, redness, and enlarged veins in the affected area, but some DVTs have no symptoms. The most common life-threatening concern with DVT is the potential for a clot to embolize
An embolism is the lodging of an embolus, a blockage-causing piece of material, inside a blood vessel. The embolus may be a blood clot (thrombus), a fat globule (fat embolism), a bubble of air or other gas (gas embolism), amniotic fluid (amnio ...
(detach from the veins), travel as an embolus
An embolus (; plural emboli; from the Greek ἔμβολος "wedge", "plug") is an unattached mass that travels through the bloodstream and is capable of creating blockages. When an embolus occludes a blood vessel, it is called an embolism or emb ...
through the right side of the heart, and become lodged in a pulmonary artery
A pulmonary artery is an artery in the pulmonary circulation that carries deoxygenated blood from the right side of the heart to the lungs. The largest pulmonary artery is the ''main pulmonary artery'' or ''pulmonary trunk'' from the heart, and ...
that supplies blood to the lungs. This is called a pulmonary embolism
Pulmonary embolism (PE) is a blockage of an artery in the lungs by a substance that has moved from elsewhere in the body through the bloodstream ( embolism). Symptoms of a PE may include shortness of breath, chest pain particularly upon breathin ...
(PE). DVT and PE comprise the cardiovascular disease of venous thromboembolism (VTE). About two-thirds of VTE manifests as DVT only, with one-third manifesting as PE with or without DVT. The most frequent long-term DVT complication is post-thrombotic syndrome
Post-thrombotic syndrome (PTS), also called postphlebitic syndrome and venous stress disorder is a medical condition that may occur as a long-term complication of deep vein thrombosis (DVT).
Signs and symptoms
Signs and symptoms of PTS in the leg ...
, which can cause pain, swelling, a sensation of heaviness, itching, and in severe cases, ulcers
An ulcer is a discontinuity or break in a bodily membrane that impedes normal function of the affected organ. According to Robbins's pathology, "ulcer is the breach of the continuity of skin, epithelium or mucous membrane caused by sloughing o ...
. Recurrent VTE occurs in about 30% of those in the ten years following an initial VTE.
The mechanism behind DVT formation typically involves some combination of decreased blood flow, increased tendency to clot, changes to the blood vessel wall, and inflammation. Risk factors include recent surgery, older age, active cancer
Cancer is a group of diseases involving abnormal cell growth with the potential to invade or spread to other parts of the body. These contrast with benign tumors, which do not spread. Possible signs and symptoms include a lump, abnormal b ...
, obesity
Obesity is a medical condition, sometimes considered a disease, in which excess body fat has accumulated to such an extent that it may negatively affect health. People are classified as obese when their body mass index (BMI)—a person's ...
, infection, inflammatory diseases, antiphospholipid syndrome
Antiphospholipid syndrome, or antiphospholipid antibody syndrome (APS or APLS), is an autoimmune, hypercoagulable state caused by antiphospholipid antibodies. APS provokes blood clots (thrombosis) in both arteries and veins as well as pregnancy-r ...
, personal history and family history
Genealogy () is the study of families, family history, and the tracing of their lineages. Genealogists use oral interviews, historical records, genetic analysis, and other records to obtain information about a family and to demonstrate kin ...
of VTE, trauma, injuries, lack of movement, hormonal birth control
Hormonal contraception refers to birth control methods that act on the endocrine system. Almost all methods are composed of steroid hormones, although in India one selective estrogen receptor modulator is marketed as a contraceptive. The origina ...
, pregnancy
Pregnancy is the time during which one or more offspring develops (gestation, gestates) inside a woman, woman's uterus (womb). A multiple birth, multiple pregnancy involves more than one offspring, such as with twins.
Pregnancy usually occur ...
, and the period following birth. VTE has a strong genetic component, accounting for approximately 50 to 60% of the variability in VTE rates. Genetic factors include non-O blood type, deficiencies of antithrombin
Antithrombin (AT) is a small glycoprotein that inactivates several enzymes of the coagulation system. It is a 432-amino-acid protein produced by the liver. It contains three disulfide bonds and a total of four possible glycosylation sites. α-A ...
, protein C
Protein C, also known as autoprothrombin IIA and blood coagulation factor XIX, is a zymogen, that is, an inactive enzyme. The activated form plays an important role in regulating anticoagulation, inflammation, and cell death and maintainin ...
, and protein S
Protein S (also known as PROS) is a vitamin K-dependent plasma glycoprotein synthesized in the liver. In the circulation, Protein S exists in two forms: a free form and a complex form bound to complement protein C4b-binding protein (C4BP). In huma ...
and the mutations of factor V Leiden
Factor V Leiden (rs6025 or ''F5'' p.R506Q) is a variant (mutated form) of human factor V (one of several substances that helps blood clot), which causes an increase in blood clotting (hypercoagulability). Due to this mutation, protein C, an anticoa ...
and prothrombin G20210A
Prothrombin G20210A is a genetic condition that increases the risk of blood clots including from deep vein thrombosis, and of pulmonary embolism. One copy of the mutation increases the risk of a blood clot from 1 in 1,000 per year to 2.5 in 1,000. ...
. In total, dozens of genetic risk factors have been identified.
People suspected of having DVT can be assessed using a prediction rule such as the Wells score. A D-dimer test can also be used to assist with excluding the diagnosis or to signal a need for further testing. Diagnosis is most commonly confirmed by ultrasound
Ultrasound is sound waves with frequencies higher than the upper audible limit of human hearing. Ultrasound is not different from "normal" (audible) sound in its physical properties, except that humans cannot hear it. This limit varies ...
of the suspected veins. VTE becomes much more common with age. The condition is rare in children, but occurs in almost 1% of those ≥ age 85 annually. Asian, Asian-American, Native American, and Hispanic individuals have a lower VTE risk than Whites or Blacks. Populations in Asia have VTE rates at 15 to 20% of what is seen in Western countries.
Using blood thinners is the standard treatment. Typical medications include rivaroxaban, apixaban, and warfarin
Warfarin, sold under the brand name Coumadin among others, is a medication that is used as an anticoagulant (blood thinner). It is commonly used to prevent blood clots such as deep vein thrombosis and pulmonary embolism, and to prevent st ...
. Beginning warfarin treatment requires an additional non-oral anticoagulant, often injections of heparin. Guyatt et al. 2012, p. 20S: 2.4. Prevention of VTE for the general population includes avoiding obesity and maintaining an active lifestyle. Preventive efforts following low-risk surgery include early and frequent walking. Riskier surgeries generally prevent VTE with a blood thinner or aspirin
Aspirin, also known as acetylsalicylic acid (ASA), is a nonsteroidal anti-inflammatory drug (NSAID) used to reduce pain, fever, and/or inflammation, and as an antithrombotic. Specific inflammatory conditions which aspirin is used to treat inc ...
combined with intermittent pneumatic compression Intermittent pneumatic compression is a therapeutic technique used in medical devices that include an air pump and inflatable auxiliary sleeves, gloves or boots in a system designed to improve venous circulation in the limbs of patients who have ede ...
.
Signs and symptoms
 Symptoms classically affect a leg and typically develop over hours or days, though they can develop suddenly or over a matter of weeks. The legs are primarily affected, with 4–10% of DVT occurring in the arms. Despite the signs and symptoms being highly variable, the typical symptoms are pain, swelling, and redness. However, these symptoms might not manifest in the lower limbs of those unable to walk. In those who are able to walk, DVT can reduce one's ability to do so. The pain can be described as throbbing and can worsen with weight-bearing, prompting one to bear more weight with the unaffected leg. Additional signs and symptoms include tenderness, pitting edema (''see image''), dilation of surface veins, warmth, discoloration, a "pulling sensation", and even cyanosis (a blue or purplish discoloration) with fever. DVT can also exist without causing any symptoms. Signs and symptoms help in determining the likelihood of DVT, but they are not used alone for diagnosis.
At times, DVT can cause symptoms in both arms or both legs, as with bilateral DVT. Rarely, a clot in the
Symptoms classically affect a leg and typically develop over hours or days, though they can develop suddenly or over a matter of weeks. The legs are primarily affected, with 4–10% of DVT occurring in the arms. Despite the signs and symptoms being highly variable, the typical symptoms are pain, swelling, and redness. However, these symptoms might not manifest in the lower limbs of those unable to walk. In those who are able to walk, DVT can reduce one's ability to do so. The pain can be described as throbbing and can worsen with weight-bearing, prompting one to bear more weight with the unaffected leg. Additional signs and symptoms include tenderness, pitting edema (''see image''), dilation of surface veins, warmth, discoloration, a "pulling sensation", and even cyanosis (a blue or purplish discoloration) with fever. DVT can also exist without causing any symptoms. Signs and symptoms help in determining the likelihood of DVT, but they are not used alone for diagnosis.
At times, DVT can cause symptoms in both arms or both legs, as with bilateral DVT. Rarely, a clot in the inferior vena cava
The inferior vena cava is a large vein that carries the deoxygenated blood from the lower and middle body into the right atrium of the heart. It is formed by the joining of the right and the left common iliac veins, usually at the level of th ...
can cause both legs to swell. Superficial vein thrombosis
Superficial vein thrombosis (SVT) is a blood clot formed in a superficial vein, a vein near the surface of the body. Usually there is thrombophlebitis, which is an inflammatory reaction around a thrombosed vein, presenting as a painful induration ...
, also known as superficial thrombophlebitis, is the formation of a blood clot (thrombus) in a vein close to the skin. It can co-occur with DVT and can be felt as a "palpable cord". Migratory thrombophlebitis
The Trousseau sign of malignancy or Trousseau's syndrome is a medical sign involving episodes of vessel inflammation due to blood clot (thrombophlebitis) which are recurrent or appearing in different locations over time (thrombophlebitis migrans o ...
(Trousseau's syndrome) is a noted finding in those with pancreatic cancer and is associated with DVT.
Acute complications
Apulmonary embolism
Pulmonary embolism (PE) is a blockage of an artery in the lungs by a substance that has moved from elsewhere in the body through the bloodstream ( embolism). Symptoms of a PE may include shortness of breath, chest pain particularly upon breathin ...
(PE) occurs when a blood clot from a deep vein
A deep vein is a vein that is deep in the body. This contrasts with superficial veins that are close to the body's surface.
Deep veins are almost always beside an artery with the same name (e.g. the femoral vein is beside the femoral artery). ...
(a DVT) detaches from a vein ( embolizes), travels through the right side of the heart, and becomes lodged as an embolus
An embolus (; plural emboli; from the Greek ἔμβολος "wedge", "plug") is an unattached mass that travels through the bloodstream and is capable of creating blockages. When an embolus occludes a blood vessel, it is called an embolism or emb ...
in a pulmonary artery
A pulmonary artery is an artery in the pulmonary circulation that carries deoxygenated blood from the right side of the heart to the lungs. The largest pulmonary artery is the ''main pulmonary artery'' or ''pulmonary trunk'' from the heart, and ...
that supplies deoxygenated blood to the lungs for oxygenation. Up to one-fourth of PE cases are thought to result in sudden death. When not fatal, PE can cause symptoms such as sudden onset shortness of breath
Shortness of breath (SOB), also medically known as dyspnea (in AmE) or dyspnoea (in BrE), is an uncomfortable feeling of not being able to breathe well enough. The American Thoracic Society defines it as "a subjective experience of breathing di ...
or chest pain, coughing up blood (hemoptysis
Hemoptysis is the coughing up of blood or blood-stained mucus from the bronchi, larynx, trachea, or lungs. In other words, it is the airway bleeding. This can occur with lung cancer, infections such as tuberculosis, bronchitis, or pneumonia, a ...
), and fainting ( syncope). The chest pain can be pleuritic
Pleurisy, also known as pleuritis, is inflammation of the membranes that surround the lungs and line the chest cavity (pleurae). This can result in a sharp chest pain while breathing. Occasionally the pain may be a constant dull ache. Other sym ...
(worsened by deep breaths) and can vary based upon where the embolus is lodged in the lungs. An estimated 30–50% of those with PE have detectable DVT by compression ultrasound.
A rare and massive DVT that causes significant obstruction and discoloration (including cyanosis) is phlegmasia cerulea dolens. It is life-threatening, limb-threatening, and carries a risk of venous gangrene. Phlegmasia cerulea dolens can occur in the arm but more commonly affects the leg. If found in the setting of acute compartment syndrome
Compartment syndrome is a condition in which increased pressure within one of the body's anatomical compartments results in insufficient blood supply to tissue within that space. There are two main types: acute and chronic. Compartments of the ...
, an urgent fasciotomy is warranted to protect the limb. Superior vena cava syndrome is a rare complication of arm DVT.
DVT is thought to be able to cause a stroke in the presence of a heart defect
A congenital heart defect (CHD), also known as a congenital heart anomaly and congenital heart disease, is a defect in the structure of the heart or great vessels that is present at birth. A congenital heart defect is classed as a cardiovascular ...
. This is called a paradoxical embolism
An embolus, is described as a free-floating mass, located inside blood vessels that can travel from one site in the blood stream to another. An embolus can be made up of solid (like a blood clot), liquid (like amniotic fluid), or gas (like air). O ...
because the clot abnormally travels from the pulmonary circuit to the systemic circuit while inside the heart. The defect
A defect is a physical, functional, or aesthetic attribute of a product or service that exhibits that the product or service failed to meet one of the desired specifications. Defect, defects or defected may also refer to:
Examples
* Angular defec ...
of a patent foramen ovale
Atrial septal defect (ASD) is a congenital heart defect in which blood flows between the atria (upper chambers) of the heart. Some flow is a normal condition both pre-birth and immediately post-birth via the foramen ovale; however, when this d ...
is thought to allow clots to travel through the interatrial septum
The interatrial septum is the wall of tissue that separates the right and left atria of the heart.
Structure
The interatrial septum is a that lies between the left atrium and right atrium of the human heart. The interatrial septum lies at angl ...
from the right atrium
The atrium ( la, ātrium, , entry hall) is one of two upper chambers in the heart that receives blood from the circulatory system. The blood in the atria is pumped into the heart ventricles through the atrioventricular valves.
There are two at ...
into the left atrium.
pulmonary arteries
A pulmonary artery is an artery in the pulmonary circulation that carries deoxygenated blood from the right side of the heart to the lungs. The largest pulmonary artery is the ''main pulmonary artery'' or ''pulmonary trunk'' from the heart, and ...
(white)
File:PCD2016.jpg, alt=Image showing marked discoloration of a leg with phlegmasia cerulea dolens, A case of phlegmasia cerulea dolens in the left leg
Patent-foramen-ovale-en.png, alt=A drawing depicting a patent foramen ovale, A depiction of a patent foramen ovale
Differential diagnosis
In most suspected cases, DVT is ruled out after evaluation.Cellulitis
Cellulitis is usually a bacterial infection involving the inner layers of the skin. It specifically affects the dermis and subcutaneous fat. Signs and symptoms include an area of redness which increases in size over a few days. The borders of ...
is a frequent mimic of DVT, with its triad of pain, swelling, and redness. Symptoms concerning for DVT are more often due to other causes, including cellulitis, ruptured Baker's cyst, hematoma, lymphedema
Lymphedema, also known as lymphoedema and lymphatic edema, is a condition of localized swelling caused by a compromised lymphatic system. The lymphatic system functions as a critical portion of the body's immune system and returns interstitial fl ...
, and chronic venous insufficiency
Chronic venous insufficiency (CVI) is a medical condition in which blood pools in the veins, straining the walls of the vein. The most common cause of CVI is superficial venous reflux which is a treatable condition. As functional venous valves ar ...
. Other differential diagnoses
In healthcare, a differential diagnosis (abbreviated DDx) is a method of analysis of a patient's history and physical examination to arrive at the correct diagnosis. It involves distinguishing a particular disease or condition from others that p ...
include tumors, venous or arterial aneurysm
An aneurysm is an outward bulging, likened to a bubble or balloon, caused by a localized, abnormal, weak spot on a blood vessel wall. Aneurysms may be a result of a hereditary condition or an acquired disease. Aneurysms can also be a nidus ( ...
s, connective tissue disorder
A connective tissue disease (collagenosis) is any disease that has the connective tissues of the body as a target of pathology. Connective tissue is any type of biological tissue with an extensive extracellular matrix that supports, binds togeth ...
s, superficial vein thrombosis
Superficial vein thrombosis (SVT) is a blood clot formed in a superficial vein, a vein near the surface of the body. Usually there is thrombophlebitis, which is an inflammatory reaction around a thrombosed vein, presenting as a painful induration ...
, muscle vein thrombosis, and varicose veins
Varicose veins, also known as varicoses, are a medical condition in which superficial veins become enlarged and twisted. These veins typically develop in the legs, just under the skin. Varicose veins usually cause few symptoms. However, some indiv ...
.
Classification
 DVT and PE are the two manifestations of the cardiovascular disease venous thromboembolism (VTE). VTE can occur as DVT only, DVT with PE, or PE only. About two-thirds of VTE manifests as DVT only, with one-third manifesting as PE with or without DVT. VTE, along with superficial vein thrombosis, are common types of venous thrombosis.
DVT is classified as acute when the clots are developing or have recently developed, whereas chronic DVT persists more than 28 days. Differences between these two types of DVT can be seen with ultrasound. An episode of VTE after an initial one is classified as recurrent. Bilateral DVT refers to clots in both limbs while unilateral means only a single limb is affected.
DVT in the legs is proximal when above the knee and distal (or calf) when below the knee. DVT below the popliteal vein, a proximal vein behind the knee, is classified as distal
DVT and PE are the two manifestations of the cardiovascular disease venous thromboembolism (VTE). VTE can occur as DVT only, DVT with PE, or PE only. About two-thirds of VTE manifests as DVT only, with one-third manifesting as PE with or without DVT. VTE, along with superficial vein thrombosis, are common types of venous thrombosis.
DVT is classified as acute when the clots are developing or have recently developed, whereas chronic DVT persists more than 28 days. Differences between these two types of DVT can be seen with ultrasound. An episode of VTE after an initial one is classified as recurrent. Bilateral DVT refers to clots in both limbs while unilateral means only a single limb is affected.
DVT in the legs is proximal when above the knee and distal (or calf) when below the knee. DVT below the popliteal vein, a proximal vein behind the knee, is classified as distaland has limited clinical significance compared to proximal DVT. Calf DVT makes up about half of DVTs. Iliofemoral DVT has been described as involving either the iliac or
common femoral vein
In the human body, the femoral vein is a blood vessel that accompanies the femoral artery in the femoral sheath. It begins at the adductor hiatus (an opening in the adductor magnus muscle) as the continuation of the popliteal vein. It ends at th ...
; elsewhere, it has been defined as involving at a minimum the common iliac vein
In human anatomy, the common iliac veins are formed by the external iliac veins and internal iliac veins. The left and right common iliac veins come together in the abdomen at the level of the fifth lumbar vertebra, forming the inferior vena c ...
, which is near the top of the pelvis.
DVT can be classified into provoked and unprovoked categories. For example, DVT that occurs in association with cancer or surgery can be classified as provoked. However, the European Society of Cardiology
The European Society of Cardiology (ESC) is an independent non-profit, non-governmental professional association that works to advance the prevention, diagnosis and management of diseases of the heart and blood vessels, and improve scientific un ...
in 2019 urged for this dichotomy to be abandoned to encourage more personalized risk assessments for recurrent VTE. The distinction between these categories is not always clear.
Causes
 Traditionally, the three factors of
Traditionally, the three factors of Virchow's triad
Virchow's triad or the triad of Virchow () describes the three broad categories of factors that are thought to contribute to thrombosis.
*Hypercoagulability
*Hemodynamic changes (stasis, turbulence)
*Endothelial injury/dysfunction
It is named a ...
—venous stasis
Venostasis, or venous stasis, is a condition of slow blood flow in the veins, usually of the legs.
Presentation Complications
Potential complications of venous stasis are:
* Venous ulcers
* Blood clot formation in veins (venous thrombosis), that ...
, hypercoagulability
Thrombophilia (sometimes called hypercoagulability or a prothrombotic state) is an abnormality of blood coagulation that increases the risk of thrombosis (blood clots in blood vessels). Such abnormalities can be identified in 50% of people who ...
, and changes in the endothelial
The endothelium is a single layer of squamous endothelial cells that line the interior surface of blood vessels and lymphatic vessels. The endothelium forms an interface between circulating blood or lymph in the lumen and the rest of the vessel ...
blood vessel lining—contribute to VTE and were used to explain its formation. More recently, inflammation
Inflammation (from la, inflammatio) is part of the complex biological response of body tissues to harmful stimuli, such as pathogens, damaged cells, or irritants, and is a protective response involving immune cells, blood vessels, and molec ...
has been identified as playing a clear causal role. Other related causes include activation of immune system
The immune system is a network of biological processes that protects an organism from diseases. It detects and responds to a wide variety of pathogens, from viruses to parasitic worms, as well as cancer cells and objects such as wood splint ...
components, the state of microparticles in the blood, the concentration of oxygen, and possible platelet
Platelets, also called thrombocytes (from Greek θρόμβος, "clot" and κύτος, "cell"), are a component of blood whose function (along with the coagulation factors) is to react to bleeding from blood vessel injury by clumping, thereby i ...
activation. Various risk factors contribute to VTE, including genetic and environmental factors, though many with multiple risk factors never develop it.
Acquired risk factors include the strong risk factor of older age, which alters blood composition to favor clotting. Previous VTE, particularly unprovoked VTE, is a strong risk factor. A leftover clot from a prior DVT increases the risk of a subsequent DVT. Major surgery and trauma
Trauma most often refers to:
* Major trauma, in physical medicine, severe physical injury caused by an external source
* Psychological trauma, a type of damage to the psyche that occurs as a result of a severely distressing event
*Traumatic i ...
increase risk because of tissue factor from outside the vascular system entering the blood. Minor injuries, lower limb amputation, hip fracture
A hip fracture is a break that occurs in the upper part of the femur (thigh bone). Symptoms may include pain around the hip, particularly with movement, and shortening of the leg. Usually the person cannot walk.
They most often occur as a res ...
, and long bone fractures are also risks. In orthopedic surgery
Orthopedic surgery or orthopedics ( alternatively spelt orthopaedics), is the branch of surgery concerned with conditions involving the musculoskeletal system. Orthopedic surgeons use both surgical and nonsurgical means to treat musculoskeletal ...
, venous stasis can be temporarily provoked by a cessation of blood flow as part of the procedure. Inactivity and immobilization contribute to venous stasis, as with orthopedic cast
An orthopedic cast, or simply cast, is a shell, frequently made from plaster or fiberglass, that encases a limb (or, in some cases, large portions of the body) to stabilize and hold anatomical structures—most often a broken bone (or bones), in ...
s, paralysis, sitting, long-haul travel, bed rest, hospitalization, catatonia
Catatonia is a complex neuropsychiatric behavioral syndrome that is characterized by abnormal movements, immobility, abnormal behaviors, and withdrawal. The onset of catatonia can be acute or subtle and symptoms can wax, wane, or change during ...
, and in survivors of acute stroke. Conditions that involve compromised blood flow in the veins are May–Thurner syndrome, where a vein of the pelvis is compressed, and venous thoracic outlet syndrome, which includes Paget–Schroetter syndrome, where compression occurs near the base of the neck.
Infections, including sepsis
Sepsis, formerly known as septicemia (septicaemia in British English) or blood poisoning, is a life-threatening condition that arises when the body's response to infection causes injury to its own tissues and organs. This initial stage is follo ...
, COVID-19
Coronavirus disease 2019 (COVID-19) is a contagious disease caused by a virus, the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The first known case was identified in Wuhan, China, in December 2019. The disease quickly ...
, HIV
The human immunodeficiency viruses (HIV) are two species of ''Lentivirus'' (a subgroup of retrovirus) that infect humans. Over time, they cause acquired immunodeficiency syndrome (AIDS), a condition in which progressive failure of the immune ...
, and active tuberculosis
Tuberculosis (TB) is an infectious disease usually caused by '' Mycobacterium tuberculosis'' (MTB) bacteria. Tuberculosis generally affects the lungs, but it can also affect other parts of the body. Most infections show no symptoms, i ...
, increase risk. Chronic inflammatory diseases and some autoimmune diseases, such as inflammatory bowel disease, systemic sclerosis
Systemic scleroderma, or systemic sclerosis, is an autoimmune rheumatic disease characterised by excessive production and accumulation of collagen, called fibrosis, in the skin and internal organs and by injuries to small arteries. There are two ...
, Behçet's syndrome, primary antiphospholipid syndrome
Antiphospholipid syndrome, or antiphospholipid antibody syndrome (APS or APLS), is an autoimmune, hypercoagulable state caused by antiphospholipid antibodies. APS provokes blood clots (thrombosis) in both arteries and veins as well as pregnancy-r ...
, and systemic lupus erythematosus (SLE) increase risk. SLE itself is frequently associated with secondary antiphospholipid syndrome.
Cancer can grow in and around veins, causing venous stasis, and can also stimulate increased levels of tissue factor. Cancers of the blood, lung, pancreas, brain, stomach, and bowel are associated with high VTE risk. Solid tumors such as adenocarcinomas can contribute to both VTE and disseminated intravascular coagulation. In severe cases, this can lead to simultaneous clotting and bleeding. Chemotherapy
Chemotherapy (often abbreviated to chemo and sometimes CTX or CTx) is a type of cancer treatment that uses one or more anti-cancer drugs ( chemotherapeutic agents or alkylating agents) as part of a standardized chemotherapy regimen. Chemothe ...
treatment also increases risk. Obesity increases the potential of blood to clot, as does pregnancy. In the postpartum
The postpartum (or postnatal) period begins after childbirth and is typically considered to end within 6 weeks as the mother's body, including hormone levels and uterus size, returns to a non-pregnant state. The terms puerperium, puerperal pe ...
, placenta
The placenta is a temporary embryonic and later fetal organ that begins developing from the blastocyst shortly after implantation. It plays critical roles in facilitating nutrient, gas and waste exchange between the physically separate mate ...
l tearing releases substances that favor clotting. Oral contraceptives and hormonal replacement therapy increase the risk through a variety of mechanisms, including altered blood coagulation protein levels and reduced fibrinolysis
Fibrinolysis is a process that prevents blood clots from growing and becoming problematic. Primary fibrinolysis is a normal body process, while secondary fibrinolysis is the breakdown of clots due to a medicine, a medical disorder, or some other ...
.
 Dozens of genetic risk factors have been identified, and they account for approximately 50 to 60% of the variability in VTE rates. As such,
Dozens of genetic risk factors have been identified, and they account for approximately 50 to 60% of the variability in VTE rates. As such, family history
Genealogy () is the study of families, family history, and the tracing of their lineages. Genealogists use oral interviews, historical records, genetic analysis, and other records to obtain information about a family and to demonstrate kin ...
of VTE is a risk factor for a first VTE. Factor V Leiden
Factor V Leiden (rs6025 or ''F5'' p.R506Q) is a variant (mutated form) of human factor V (one of several substances that helps blood clot), which causes an increase in blood clotting (hypercoagulability). Due to this mutation, protein C, an anticoa ...
, which makes factor V
Factor V (pronounced factor five) is a protein of the coagulation system, rarely referred to as proaccelerin or labile factor. In contrast to most other coagulation factors, it is not enzymatically active but functions as a cofactor. Deficienc ...
resistant to inactivation by activated protein C
Protein C, also known as autoprothrombin IIA and blood coagulation factor XIX, is a zymogen, that is, an inactive enzyme. The activated form plays an important role in regulating anticoagulation, inflammation, and cell death and maintaini ...
, mildly increases VTE risk by about three times. Deficiencies of three proteins that normally prevent blood from clotting—protein C
Protein C, also known as autoprothrombin IIA and blood coagulation factor XIX, is a zymogen, that is, an inactive enzyme. The activated form plays an important role in regulating anticoagulation, inflammation, and cell death and maintainin ...
, protein S
Protein S (also known as PROS) is a vitamin K-dependent plasma glycoprotein synthesized in the liver. In the circulation, Protein S exists in two forms: a free form and a complex form bound to complement protein C4b-binding protein (C4BP). In huma ...
, and antithrombin
Antithrombin (AT) is a small glycoprotein that inactivates several enzymes of the coagulation system. It is a 432-amino-acid protein produced by the liver. It contains three disulfide bonds and a total of four possible glycosylation sites. α-A ...
—contribute to VTE. These deficiencies in antithrombin, protein C
Protein C, also known as autoprothrombin IIA and blood coagulation factor XIX, is a zymogen, that is, an inactive enzyme. The activated form plays an important role in regulating anticoagulation, inflammation, and cell death and maintainin ...
, and protein S
Protein S (also known as PROS) is a vitamin K-dependent plasma glycoprotein synthesized in the liver. In the circulation, Protein S exists in two forms: a free form and a complex form bound to complement protein C4b-binding protein (C4BP). In huma ...
are rare but strong, or moderately strong, risk factors. They increase risk by about 10 times. Having a non-O blood type roughly doubles VTE risk. Non-O blood type is common globally, making it an important risk factor. Individuals without O blood type have higher blood levels of von Willebrand factor
Von Willebrand factor (VWF) () is a blood glycoprotein involved in hemostasis, specifically, platelet adhesion. It is deficient and/or defective in von Willebrand disease and is involved in many other diseases, including thrombotic thrombocytope ...
and factor VIII
Factor VIII (FVIII) is an essential blood-clotting protein, also known as anti-hemophilic factor (AHF). In humans, factor VIII is encoded by the ''F8'' gene. Defects in this gene result in hemophilia A, a recessive X-linked coagulation disorder ...
than those with O blood type, increasing the likelihood of clotting. Those homozygous
Zygosity (the noun, zygote, is from the Greek "yoked," from "yoke") () is the degree to which both copies of a chromosome or gene have the same genetic sequence. In other words, it is the degree of similarity of the alleles in an organism.
Mo ...
for the common fibrinogen gamma gene variant rs2066865 have about a 1.6 times higher risk of VTE. The genetic variant prothrombin G20210A
Prothrombin G20210A is a genetic condition that increases the risk of blood clots including from deep vein thrombosis, and of pulmonary embolism. One copy of the mutation increases the risk of a blood clot from 1 in 1,000 per year to 2.5 in 1,000. ...
, which increases prothrombin levels, increases risk by about 2.5 times. Additionally, approximately 5% of people have been identified with a background genetic risk comparable to the factor V Leiden and prothrombin G20210A mutations.
Blood alterations including dysfibrinogenemia, low free protein S, activated protein C resistance
Activated protein C resistance (APCR) is a hypercoagulability (an increased tendency of the blood to clot) characterized by a lack of a response to activated protein C (APC), which normally helps prevent blood from clotting excessively. This resul ...
, homocystinuria
Homocystinuria or HCU is an inherited disorder of the metabolism of the amino acid methionine due to a deficiency of cystathionine beta synthase or methionine synthase. It is an inherited autosomal recessive trait, which means a child needs to i ...
, hyperhomocysteinemia
Hyperhomocysteinemia is a medical condition characterized by an abnormally high level of homocysteine in the blood, conventionally described as above 15 μmol/L.
As a consequence of the biochemical reactions in which homocysteine is involved ...
, high fibrinogen
Fibrinogen (factor I) is a glycoprotein complex, produced in the liver, that circulates in the blood of all vertebrates. During tissue and vascular injury, it is converted enzymatically by thrombin to fibrin and then to a fibrin-based blood cl ...
levels, high factor IX
Factor IX (or Christmas factor) () is one of the serine proteases of the coagulation system; it belongs to peptidase family S1. Deficiency of this protein causes haemophilia B. It was discovered in 1952 after a young boy named Stephen Christmas ...
levels, and high factor XI
Factor XI or plasma thromboplastin antecedent is the zymogen form of factor XIa, one of the enzymes of the coagulation cascade. Like many other coagulation factors, it is a serine protease. In humans, Factor XI is encoded by the ''F11'' gene.
...
levels are associated with increased risk. Other associated conditions include heparin-induced thrombocytopenia, catastrophic antiphospholipid syndrome, paroxysmal nocturnal hemoglobinuria
Paroxysmal nocturnal hemoglobinuria (PNH) is a rare, acquired, life-threatening disease of the blood characterized by destruction of red blood cells by the complement system, a part of the body's innate immune system. This destructive process occu ...
, nephrotic syndrome, chronic kidney disease, polycythemia vera
Polycythemia vera is an uncommon myeloproliferative neoplasm (a type of chronic leukemia) in which the bone marrow makes too many red blood cells. It may also result in the overproduction of white blood cells and platelets.
Most of the healt ...
, essential thrombocythemia
Essential thrombocythemia (ET) is a rare chronic blood cancer (myeloproliferative neoplasm) characterised by the thrombocythemia, overproduction of platelets (thrombocytes) by megakaryocytes in the bone marrow. It may, albeit rarely, develop into a ...
, intravenous drug use, and smoking.
Some risk factors influence the location of DVT within the body. In isolated distal DVT, the profile of risk factors appears distinct from proximal DVT. Transient factors, such as surgery and immobilization, appear to dominate, whereas thrombophilias and age do not seem to increase risk. Common risk factors for having an upper extremity DVT include having an existing foreign body (such as a central venous catheter, a pacemaker, or a triple-lumen PICC line), cancer, and recent surgery.
Pathophysiology
 Blood has a natural tendency to clot when blood vessels are damaged (
Blood has a natural tendency to clot when blood vessels are damaged (hemostasis
In biology, hemostasis or haemostasis is a process to prevent and stop bleeding, meaning to keep blood within a damaged blood vessel (the opposite of hemostasis is hemorrhage). It is the first stage of wound healing. This involves coagulation, ...
) to minimize blood loss. Clotting is activated by the coagulation cascade and the clearing of clots that are no longer needed is accomplished by the process of fibrinolysis
Fibrinolysis is a process that prevents blood clots from growing and becoming problematic. Primary fibrinolysis is a normal body process, while secondary fibrinolysis is the breakdown of clots due to a medicine, a medical disorder, or some other ...
. Reductions in fibrinolysis or increases in coagulation can increase the risk of DVT.
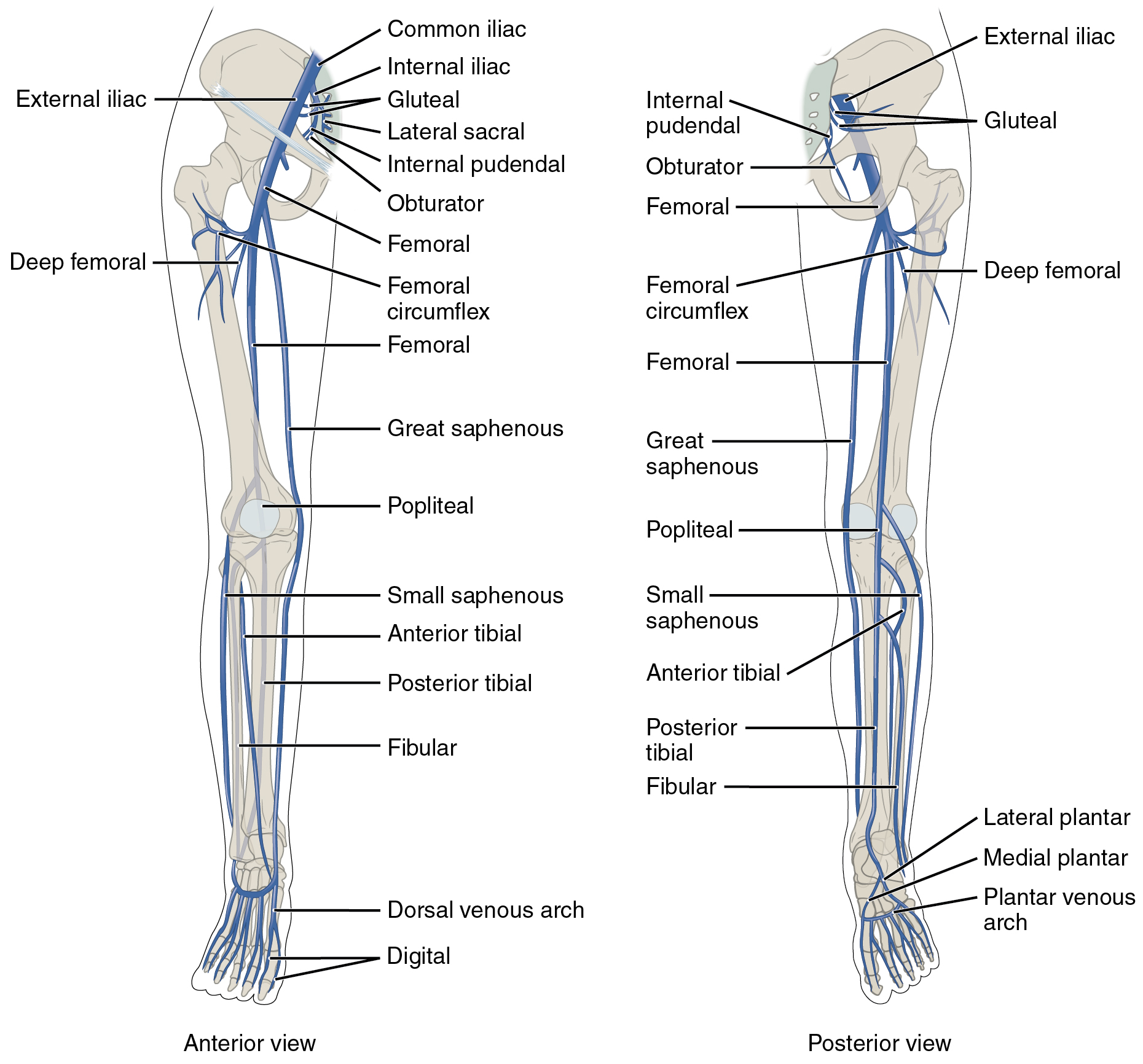
DVT often develops in the calf veins and "grows" in the direction of venous flow, towards the heart. DVT most frequently affects veins in the leg or pelvis including the popliteal vein
The popliteal vein is a vein of the lower limb. It is formed from the anterior tibial vein and the posterior tibial vein. It travels medial to the popliteal artery, and becomes the femoral vein. It drains blood from the leg. It can be assess ...
(behind the knee), femoral vein
In the human body, the femoral vein is a blood vessel that accompanies the femoral artery in the femoral sheath. It begins at the adductor hiatus (an opening in the adductor magnus muscle) as the continuation of the popliteal vein. It ends a ...
(of the thigh), and iliac veins of the pelvis. Extensive lower-extremity DVT can even reach into the inferior vena cava
The inferior vena cava is a large vein that carries the deoxygenated blood from the lower and middle body into the right atrium of the heart. It is formed by the joining of the right and the left common iliac veins, usually at the level of th ...
(in the abdomen). Upper extremity DVT most commonly affects the subclavian, axillary, and jugular vein
The jugular veins are veins that take deoxygenated blood from the head back to the heart via the superior vena cava. The internal jugular vein descends next to the internal carotid artery and continues posteriorly to the sternocleidomastoid mu ...
s.
The process of fibrinolysis, where DVT clots can be dissolved back into the blood, acts to temper the process of thrombus growth. This is the preferred process. Aside from the potentially deadly process of embolization, a clot can resolve through organization, which can damage the valves of veins, cause vein fibrosis, and result in non-compliant veins. Organization of a thrombus into the vein can occur at the third stage of its pathological
Pathology is the study of the causes and effects of disease or injury. The word ''pathology'' also refers to the study of disease in general, incorporating a wide range of biology research fields and medical practices. However, when used in th ...
development, in which collagen becomes the characteristic component. The first pathological stage is marked by red blood cells, and the second is characterized by medium-textured fibrin.
 In arterial thrombosis, blood vessel wall damage is required, as it initiates
In arterial thrombosis, blood vessel wall damage is required, as it initiates coagulation
Coagulation, also known as clotting, is the process by which blood changes from a liquid to a gel, forming a blood clot. It potentially results in hemostasis, the cessation of blood loss from a damaged vessel, followed by repair. The mechanis ...
, but clotting in the veins mostly occurs without any such mechanical damage. The beginning of venous thrombosis is thought to arise from "activation of endothelial cells, platelets, and leukocytes, with initiation of inflammation and formation of microparticles that trigger the coagulation system" via tissue factor. Vein wall inflammation is likely the inciting event. Importantly, the activated endothelium of veins interacts with circulating white blood cells (leukocytes). While leukocytes normally help prevent blood from clotting (as does normal endothelium), upon stimulation, leukocytes facilitate clotting. Neutrophils are recruited early in the process of venous thrombi formation. They release pro-coagulant granules and neutrophil extracellular traps
Neutrophil extracellular traps (NETs) are networks of extracellular fibers, primarily composed of DNA from neutrophils, which bind pathogens. Neutrophils are the immune system's first line of defense against infection and have conventionally be ...
(NETs) or their components, which play a role in venous thrombi formation. NET components are pro-thrombotic through both the intrinsic and extrinsic coagulation pathways. NETs provide "a scaffold for adhesion" of platelets, red blood cells, and multiple factors that potentiate platelet activation. In addition to the pro-coagulant activities of neutrophils, multiple stimuli cause monocytes to release tissue factor. Monocytes are also recruited early in the process.
Tissue factor, via the tissue factor–factor VIIa
Coagulation factor VII (, formerly known as proconvertin) is one of the proteins that causes blood to clot in the coagulation cascade, and in humans is coded for by the gene ''F7''. It is an enzyme of the serine protease class. Once bound to tiss ...
complex, activates the extrinsic pathway of coagulation and leads to conversion of prothrombin to thrombin, followed by fibrin deposition. Fresh venous clots are red blood cell
Red blood cells (RBCs), also referred to as red cells, red blood corpuscles (in humans or other animals not having nucleus in red blood cells), haematids, erythroid cells or erythrocytes (from Greek ''erythros'' for "red" and ''kytos'' for "holl ...
and fibrin rich. Platelets and white blood cells are also components. Platelets are not as prominent in venous clots as they are in arterial ones, but they can play a role. In cancer, tissue factor is produced by cancer cells. Cancer also produces unique substances that stimulate factor Xa
Factor X, also known by the eponym Stuart–Prower factor, is an enzyme () of the coagulation cascade. It is a serine endopeptidase (protease group S1, PA clan). Factor X is synthesized in the liver and requires vitamin K for its synthesis.
Fa ...
, cytokines that promote endothelial dysfunction
In vascular diseases, endothelial dysfunction is a systemic pathological state of the endothelium. Along with acting as a semi-permeable membrane, the endothelium is responsible for maintaining vascular tone and regulating oxidative stress by ...
, and plasminogen activator inhibitor-1
Plasminogen activator inhibitor-1 (PAI-1) also known as endothelial plasminogen activator inhibitor or serpin E1 is a protein that in humans is encoded by the ''SERPINE1'' gene. Elevated PAI-1 is a risk factor for thrombosis and atherosclerosis
P ...
, which inhibits the breakdown of clots (fibrinolysis).
Often, DVT begins in the valves of veins. The blood flow pattern in the valves can cause low oxygen concentrations in the blood (hypoxemia
Hypoxemia is an abnormally low level of oxygen in the blood. More specifically, it is oxygen deficiency in arterial blood. Hypoxemia has many causes, and often causes hypoxia as the blood is not supplying enough oxygen to the tissues of the bod ...
) of a valve sinus. Hypoxemia, which is worsened by venous stasis, activates pathways—ones that include hypoxia-inducible factor-1 and early-growth-response protein 1. Hypoxemia also results in the production of reactive oxygen species
In chemistry, reactive oxygen species (ROS) are highly reactive chemicals formed from diatomic oxygen (). Examples of ROS include peroxides, superoxide, hydroxyl radical, singlet oxygen, and alpha-oxygen.
The reduction of molecular oxygen () p ...
, which can activate these pathways, as well as nuclear factor-κB, which regulates hypoxia-inducible factor-1 transcription. Hypoxia-inducible factor-1 and early-growth-response protein 1 contribute to monocyte association with endothelial proteins, such as P-selectin
P-selectin is a type-1 transmembrane protein that in humans is encoded by the SELP gene.
P-selectin functions as a cell adhesion molecule (CAM) on the surfaces of activated endothelial cells, which line the inner surface of blood vessels, and act ...
, prompting monocytes to release tissue factor-filled microvesicles
Microvesicles (ectosomes, or microparticles) are a type of extracellular vesicle (EV) that are released from the cell membrane. In multicellular organisms, microvesicles and other EVs are found both in tissues (in the interstitial space between c ...
, which presumably begin clotting after binding to the endothelial surface.
D-dimers are a fibrin degradation product
Fibrin degradation products (FDPs), also known as fibrin split products, are components of the blood produced by clot degeneration.
Clotting, also called coagulation, at the wound site produces a mass of fibrin threads called a net that remains in ...
, a natural byproduct of fibrinolysis that is typically found in the blood. An elevated level can result from plasmin
Plasmin is an important enzyme () present in blood that degrades many blood plasma proteins, including fibrin clots. The degradation of fibrin is termed fibrinolysis. In humans, the plasmin protein (in the zymogen form of plasminogen) is encode ...
dissolving a clot—or other conditions. Hospitalized patients often have elevated levels for multiple reasons. Anticoagulation, the standard treatment for DVT, prevents further clot growth and PE, but does not act directly on existing clots.
Diagnosis
A clinical probability assessment using the Wells score (see column in the table below) to determine if a potential DVT is "likely" or "unlikely" is typically the first step of the diagnostic process. The score is used in suspected first lower extremity DVT (without any PE symptoms) in primary care and outpatient settings, including the emergency department. The numerical result (possible score −2 to 9) is most commonly grouped into either "unlikely" or "likely" categories. A Wells score of two or more means DVT is considered "likely" (about a 28% chance), while those with a lower score are considered "unlikely" to have DVT (about a 6% chance). In those unlikely to have DVT, a diagnosis is excluded by a negative D-dimer blood test. In people with likely DVT,ultrasound
Ultrasound is sound waves with frequencies higher than the upper audible limit of human hearing. Ultrasound is not different from "normal" (audible) sound in its physical properties, except that humans cannot hear it. This limit varies ...
is the standard imaging
Imaging is the representation or reproduction of an object's form; especially a visual representation (i.e., the formation of an image).
Imaging technology is the application of materials and methods to create, preserve, or duplicate images.
...
used to confirm or exclude a diagnosis. Imaging is also needed for hospital inpatients with suspected DVT and those initially categorized as unlikely to have DVT but who have a positive D-dimer test.
While the Wells score is the predominant and most studied clinical prediction rule for DVT, it does have drawbacks. The Wells score requires a subjective assessment regarding the likelihood of an alternate diagnosis and performs less well in the elderly and those with a prior DVT. The Dutch Primary Care Rule has also been validated for use. It contains only objective criteria but requires obtaining a D-dimer value. With this prediction rule, three points or less means a person is at low risk for DVT. A result of four or more points indicates an ultrasound is needed. Instead of using a prediction rule, experienced physicians can make a DVT pre-test probability assessment using clinical assessment and gestalt, but prediction rules are more reliable.
Compression ultrasonography for suspected deep vein thrombosis is the standard diagnostic method, and it is highly sensitive for detecting an initial DVT. A compression ultrasound is considered positive when the vein walls of normally compressible veins do not collapse under gentle pressure. Clot visualization is sometimes possible, but is not required. Three compression ultrasound scanning techniques can be used, with two of the three methods requiring a second ultrasound some days later to rule out the diagnosis. Whole-leg ultrasound is the option that does not require a repeat ultrasound, but proximal compression ultrasound is frequently used because distal DVT is only rarely clinically significant. Ultrasound methods including duplex and color flow Doppler can be used to further characterize the clot and Doppler ultrasound is especially helpful in the non-compressible iliac veins.
CT scan venography, MRI venography, or a non-contrast MRI are also diagnostic possibilities. The gold standard
A gold standard is a monetary system in which the standard economic unit of account is based on a fixed quantity of gold. The gold standard was the basis for the international monetary system from the 1870s to the early 1920s, and from the l ...
for judging imaging methods is contrast venography
Venography (also called phlebography or ascending phlebography) is a procedure in which an x-ray of the veins, a venogram, is taken after a special dye is injected into the bone marrow or veins. The dye has to be injected constantly via a catheter ...
, which involves injecting a peripheral vein of the affected limb with a contrast agent and taking X-rays, to reveal whether the venous supply has been obstructed. Because of its cost, invasiveness, availability, and other limitations, this test is rarely performed.
Doppler ultrasonography
Doppler ultrasonography is medical ultrasonography that employs the Doppler effect to perform imaging of the movement of tissues and body fluids (usually blood), and their relative velocity to the probe. By calculating the frequency shift of ...
showing absence of flow and hyperechogenic content in a clotted femoral vein
In the human body, the femoral vein is a blood vessel that accompanies the femoral artery in the femoral sheath. It begins at the adductor hiatus (an opening in the adductor magnus muscle) as the continuation of the popliteal vein. It ends a ...
(labeled subsartorial) distal to the branching point of the deep femoral vein. When compared to this clot, clots that instead obstruct the common femoral vein (proximal to this branching point) cause more severe effects due to impacting a significantly larger portion of the leg.
Iliac vein deep vein thrombosis.JPEG, An abdominal CT scan demonstrating an iliofemoral DVT, with the clot in the right common iliac vein of the pelvis
Management
Treatment for DVT is warranted when the clots are either proximal, distal and symptomatic, or upper extremity and symptomatic. Providing anticoagulation, or blood-thinning medicine, is the typical treatment after patients are checked to make sure they are not subject tobleeding
Bleeding, hemorrhage, haemorrhage or blood loss, is blood escaping from the circulatory system from damaged blood vessels. Bleeding can occur internally, or externally either through a natural opening such as the mouth, nose, ear, urethra, vag ...
. However, treatment varies depending upon the location of DVT. For example, in cases of isolated distal DVT, ultrasound surveillance (a second ultrasound after 2 weeks to check for proximal clots), might be used instead of anticoagulation. Although, those with isolated distal DVT at a high-risk of VTE recurrence are typically anticoagulated as if they had proximal DVT. Those at a low-risk for recurrence might receive a four to six week course of anticoagulation, lower doses, or no anticoagulation at all. In contrast, those with proximal DVT should receive at least 3 months of anticoagulation.
Some anticoagulants can be taken by mouth, and these oral medicines include warfarin
Warfarin, sold under the brand name Coumadin among others, is a medication that is used as an anticoagulant (blood thinner). It is commonly used to prevent blood clots such as deep vein thrombosis and pulmonary embolism, and to prevent st ...
(a vitamin K antagonist
Vitamin K antagonists (VKA) are a group of substances that reduce blood clotting by reducing the action of vitamin K. The term "vitamin K antagonist" is technically a misnomer, as the drugs do not directly antagonise the action of vitamin K in t ...
), rivaroxaban (a factor Xa inhibitor), apixaban (a factor Xa inhibitor), dabigatran
Dabigatran, sold under the brand name Pradaxa among others, is an anticoagulant used to treat and prevent blood clots and to prevent stroke in people with atrial fibrillation. Specifically it is used to prevent blood clots following hip or kn ...
(a direct thrombin inhibitor Direct thrombin inhibitors (DTIs) are a class of medication that act as anticoagulants (delaying blood clotting) by directly inhibiting the enzyme thrombin (factor IIa). Some are in clinical use, while others are undergoing clinical development. Sev ...
), and edoxaban
Edoxaban, sold under the brand name Lixiana among others, is an anticoagulant medication and a direct factor Xa inhibitor. It is taken by mouth.
Compared with warfarin it has fewer drug interactions.
It was developed by Daiichi Sankyo an ...
(a factor Xa inhibitor). Other anticoagulants cannot be taken by mouth. These parenteral (non-oral) medicines include low-molecular-weight heparin, fondaparinux, and unfractionated heparin. Some oral medicines are sufficient when taken alone, while others require the use of an additional parenteral blood thinner. Rivaroxaban and apixaban are the typical first-line medicines, and they are sufficient when taken orally. Rivaroxaban is taken once daily, and apixaban is taken twice daily. Warfarin, dabigatran, and edoxaban require the use of a parenteral anticoagulant to initiate oral anticoagulant therapy. When warfarin is initiated for VTE treatment, a 5-day minimum of a parenteral anticoagulant together with warfarin is given, which is followed by warfarin-only therapy. Warfarin is taken to maintain an international normalized ratio (INR) of 2.0–3.0, with 2.5 as the target. The benefit of taking warfarin declines as the duration of treatment extends, and the risk of bleeding increases with age. Periodic INR monitoring is not necessary when first-line direct oral anticoagulants are used. Overall, anticoagulation therapy is complex and many circumstances can affect how these therapies are managed.
The duration of anticoagulation therapy (whether it will last 4 to 6 weeks, 6 to 12 weeks, 3 to 6 months, or indefinitely) is a key factor in clinical decision making. When proximal DVT is provoked by surgery or trauma a 3-month course of anticoagulation is standard. When a first VTE is proximal DVT that is either unprovoked or associated with transient non-surgical risk factor, low-dose anticoagulation beyond 3 to 6 months might be used. In those with an annual risk of VTE in excess of 9%, as after an unprovoked episode, extended anticoagulation is a possibility. Those who finish warfarin treatment after idiopathic VTE with an elevated D-dimer level show an increased risk of recurrent VTE (about 9% vs about 4% for normal results), and this result might be used in clinical decision making. Thrombophilia test results rarely play a role in the length of treatment.
Treatment for acute leg DVT is suggested to continue at home for uncomplicated DVT instead of hospitalization. Factors that favor hospitalization include severe symptoms or additional medical issues. Early walking is suggested over bedrest. Graduated compression stockings—which apply higher pressure at the ankles and a lower pressure around the knees can be trialed for symptomatic management of acute DVT symptoms, but they are not recommended for reducing the risk of post-thrombotic syndrome
Post-thrombotic syndrome (PTS), also called postphlebitic syndrome and venous stress disorder is a medical condition that may occur as a long-term complication of deep vein thrombosis (DVT).
Signs and symptoms
Signs and symptoms of PTS in the leg ...
, as the potential benefit of using them for this goal "may be uncertain". Nor are compression stockings likely to reduce VTE recurrence. They are, however, recommended in those with isolated distal DVT.
If someone decides to stop anticoagulation after an unprovoked VTE instead of being on lifelong anticoagulation, aspirin can be used to reduce the risk of recurrence, but it is only about 33% as effective as anticoagulation in preventing recurrent VTE. Statin
Statins, also known as HMG-CoA reductase inhibitors, are a class of lipid-lowering medications that reduce illness and mortality in those who are at high risk of cardiovascular disease. They are the most common cholesterol-lowering drugs.
Low ...
s have also been investigated for their potential to reduce recurrent VTE rates, with some studies suggesting effectiveness.
Investigations for cancer
An unprovoked VTE might signal the presence of an unknown cancer, as it is an underlying condition in up to 10% of unprovoked cases. A thorough clinical assessment is needed and should include aphysical examination
In a physical examination, medical examination, or clinical examination, a medical practitioner examines a patient for any possible medical signs or symptoms of a medical condition. It generally consists of a series of questions about the pati ...
, a review of medical history
The medical history, case history, or anamnesis (from Greek: ἀνά, ''aná'', "open", and μνήσις, ''mnesis'', "memory") of a patient is information gained by a physician by asking specific questions, either to the patient or to other peo ...
, and universal cancer screening
Cancer screening aims to detect cancer before symptoms appear. This may involve blood tests, urine tests, DNA tests, other tests, or medical imaging. The benefits of screening in terms of cancer prevention, early detection and subsequent treatment ...
done in people of that age. A review of prior imaging is considered worthwhile, as is "reviewing baseline blood test results including full blood count
A complete blood count (CBC), also known as a full blood count (FBC), is a set of medical laboratory tests that provide information about the cells in a person's blood. The CBC indicates the counts of white blood cells, red blood cells and plat ...
, renal
The kidneys are two reddish-brown bean-shaped organs found in vertebrates. They are located on the left and right in the retroperitoneal space, and in adult humans are about in length. They receive blood from the paired renal arteries; bloo ...
and hepatic function, PT and APTT."National Institute for Health and Care Excellence"NICE Guideline 158: Venous thromboembolic diseases: diagnosis, management and thrombophilia testing
London, 26 March 2020. It is not recommended practice to obtain
tumor markers
A tumor marker is a biomarker found in blood, urine, or body tissues that can be elevated by the presence of one or more types of cancer. There are many different tumor markers, each indicative of a particular disease process, and they are used ...
or a CT of the abdomen and pelvis in asymptomatic individuals. NICE
Nice ( , ; Niçard dialect, Niçard: , classical norm, or , nonstandard, ; it, Nizza ; lij, Nissa; grc, Νίκαια; la, Nicaea) is the prefecture of the Alpes-Maritimes departments of France, department in France. The Nice urban unit, agg ...
recommends that further investigations are unwarranted in those without relevant signs or symptoms.
Interventions
Thrombolysis
Thrombolysis, also called fibrinolytic therapy, is the breakdown (lysis) of blood clots formed in blood vessels, using medication. It is used in ST elevation myocardial infarction, stroke, and in cases of severe venous thromboembolism (massive ...
is the injection of an enzyme into the veins to dissolve blood clots, and while this treatment has been proven effective against the life-threatening emergency clots of stroke and heart attacks, randomized controlled trials have not established a net benefit in those with acute proximal DVT. Drawbacks of catheter-directed thrombolysis (the preferred method of administering the clot-busting enzyme) include a risk of bleeding, complexity, and the cost of the procedure. Although, while anticoagulation is the preferred treatment for DVT, thrombolysis is a treatment option for those with the severe DVT form of phlegmasia cerula dorens (''bottom left image'') and in some younger patients with DVT affecting the iliac and common femoral veins. Of note, a variety of contraindications to thrombolysis exist. In 2020, NICE kept their 2012 recommendations that catheter-directed thrombolysis should be considered in those with iliofemoral DVT who have "symptoms lasting less than 14 days, good functional status, a life expectancy of 1 year or more, and a low risk of bleeding."
A mechanical thrombectomy device can remove DVT clots, particularly in acute iliofemoral DVT (DVT of the major veins in the pelvis), but there is limited data on its efficacy. It is usually combined with thrombolysis, and sometimes temporary IVC filters are placed to protect against PE during the procedure.National Institute for Health and Care Excellence"NICE Interventional procedures guidance 651: Percutaneous mechanical thrombectomy for acute deep vein thrombosis of the leg
London, 12 June 2019. Catheter-directed thrombolysis with thrombectomy against iliofemoral DVT has been associated with a reduction in the severity of post-thrombotic syndrome at an estimated cost-effectiveness ratio of about $138,000 per gained
QALY
The quality-adjusted life year (QALY) is a generic measure of disease burden, including both the quality and the quantity of life lived. It is used in economic evaluation to assess the value of medical interventions. One QALY equates to one year ...
. Phlegmasia cerulea dolens might be treated with catheter-directed thrombolysis and/or thrombectomy.
In DVT in the arm, the first (topmost) rib can be surgically removed as part of the typical treatment when the DVT is due to thoracic outlet syndrome or Paget–Schroetter syndrome. This treatment involves initial anticoagulation followed by thrombolysis of the subclavian vein and staged first rib resection to relieve the thoracic outlet compression and prevent recurrent DVT.
sequelae
A sequela (, ; usually used in the plural, sequelae ) is a pathological condition resulting from a disease, injury, therapy, or other trauma. Derived from the Latin word, meaning “sequel”, it is used in the medical field to mean a complication ...
from thoracic outlet compression.
 The placement of an
The placement of an inferior vena cava filter
An inferior vena cava filter is a medical device made of metal that is implanted by vascular surgeons or interventional radiologists into the inferior vena cava to
prevent a life-threatening pulmonary embolism (PE) or venous thromboembolism (VT ...
(IVC filter) is possible when either the standard treatment for acute DVT, anticoagulation, is absolutely contraindicated (not possible), or if someone develops a PE despite being anticoagulated. However, a 2020 NICE review found "little good evidence" for their use. A 2018 study associated IVC filter placement with a 50% reduction in PE, a 70% increase in DVT, and an 18% increase in 30 day mortality when compared to no IVC placement. Other studies including a systematic review and meta-analysis did not find a difference in mortality with IVC placement. If someone develops a PE despite being anticoagulated, care should be given to optimize anticoagulation treatment and address other related concerns before considering IVC filter placement.
Field of medicine
Patients with a history of DVT might be managed byprimary care
Primary care is the day-to-day healthcare given by a health care provider. Typically this provider acts as the first contact and principal point of continuing care for patients within a healthcare system, and coordinates other specialist care ...
, general internal medicine, hematology, cardiology
Cardiology () is a branch of medicine that deals with disorders of the heart and the cardiovascular system. The field includes medical diagnosis and treatment of congenital heart defects, coronary artery disease, heart failure, valvular h ...
, vascular surgery, or vascular medicine
Angiology (from Greek , ''angeīon'', "vessel"; and , ''-logia'') is the medical specialty dedicated to studying the circulatory system and of the lymphatic system, i.e., arteries, veins and lymphatic vessels.
In the UK, this field is more oft ...
. Patients suspected of having an acute DVT are often referred to the emergency department for evaluation. Interventional radiology is the specialty that typically places and retrieves IVC filters, and vascular surgery might do catheter directed thrombosis for some severe DVTs.
Prevention
For the prevention of blood clots in the general population, incorporating leg exercises while sitting down for long periods, or having breaks from a sitting position and walking around, having an active lifestyle, and maintaining a healthy body weight are recommended. Walking increases blood flow through the leg veins. Excess body weight is modifiable unlike most risk factors, and interventions or lifestyle modifications that help someone who is overweight or obese lose weight reduce DVT risk. Avoiding both smoking and aWestern pattern diet
The Western pattern diet is a modern dietary pattern that is generally characterized by high intakes of pre-packaged foods, refined grains, red meat, processed meat, high-sugar drinks, candy and sweets, fried foods, conventionally-raised anim ...
are thought to reduce risk. Statins have been investigated for primary prevention (prevention of a first VTE), and the JUPITER trial, which used rosuvastatin, has provided some tentative evidence of effectiveness. Of the statins, rosuvastatin appears to be the only one with the potential to reduce VTE risk. If so, it appears to reduce risk by about 15%. However, the number needed to treat
The number needed to treat (NNT) or number needed to treat for an additional beneficial outcome (NNTB) is an epidemiological measure used in communicating the effectiveness of a health-care intervention, typically a treatment with medication. The ...
to prevent one initial VTE is about 2000, limiting its applicability.
Hospital (non-surgical) patients
Acutely ill hospitalized patients are suggested to receive a parenteral anticoagulant, although the potential net benefit is uncertain. Critically ill hospitalized patients are recommended to either receive unfractionated heparin or low-molecular weight heparin instead of foregoing these medicines.After surgery
 Major orthopedic surgery—
Major orthopedic surgery—total hip replacement
Hip replacement is a surgical procedure in which the hip joint is replaced by a prosthetic implant, that is, a hip prosthesis. Hip replacement surgery can be performed as a total replacement or a hemi (half) replacement. Such joint replacement ...
, total knee replacement, or hip fracture surgery—has a high risk of causing VTE. If prophylaxis is not used after these surgeries, symptomatic VTE has about a 4% chance of developing within 35 days. Following major orthopedic surgery, a blood thinner or aspirin is typically paired with intermittent pneumatic compression Intermittent pneumatic compression is a therapeutic technique used in medical devices that include an air pump and inflatable auxiliary sleeves, gloves or boots in a system designed to improve venous circulation in the limbs of patients who have ede ...
, which is the preferred mechanical prophylaxis over graduated compression stockings.
Options for VTE prevention in people following non-orthopedic surgery include early walking, mechanical prophylaxis, and blood thinners (low-molecular-weight heparin and low-dose-unfractionated heparin) depending upon the risk of VTE, risk of major bleeding, and person's preferences. After low-risk surgeries, early and frequent walking is the best preventive measure.
Pregnancy
The risk of VTE is increased in pregnancy by about four to five times because of a more hypercoagulable state that protects against fatalpostpartum hemorrhage
Postpartum bleeding or postpartum hemorrhage (PPH) is often defined as the loss of more than 500 ml or 1,000 ml of blood following childbirth. Some have added the requirement that there also be signs or symptoms of low blood volume fo ...
. Preventive measures for pregnancy-related VTE were suggested by the American Society of Hematology in 2018. Warfarin, a common vitamin K antagonist, can cause birth defects and is not used for prevention during pregnancy.
Travelers
 Travelling "is an often cited yet relatively uncommon" cause of VTE. Suggestions for at-risk long-haul travelers include calf exercises, frequent walking, and aisle seating in airplanes to ease walking. See section 6.0, Long-Distance Travel Graduated compression stockings have sharply reduced the levels of asymptomatic DVT in airline passengers, but the effect on symptomatic DVT, PE, or mortality is unknown, as none of the individuals studied developed these outcomes. However, graduated compression stockings are not suggested for long-haul travelers (>4 hours) without risk factors for VTE. Likewise, neither aspirin nor anticoagulants are suggested in the general population undertaking long-haul travel. Those with significant VTE risk factors undertaking long-haul travel are suggested to use either graduated compression stockings or LMWH for VTE prevention. If neither of these two methods are feasible, then aspirin is suggested.
Travelling "is an often cited yet relatively uncommon" cause of VTE. Suggestions for at-risk long-haul travelers include calf exercises, frequent walking, and aisle seating in airplanes to ease walking. See section 6.0, Long-Distance Travel Graduated compression stockings have sharply reduced the levels of asymptomatic DVT in airline passengers, but the effect on symptomatic DVT, PE, or mortality is unknown, as none of the individuals studied developed these outcomes. However, graduated compression stockings are not suggested for long-haul travelers (>4 hours) without risk factors for VTE. Likewise, neither aspirin nor anticoagulants are suggested in the general population undertaking long-haul travel. Those with significant VTE risk factors undertaking long-haul travel are suggested to use either graduated compression stockings or LMWH for VTE prevention. If neither of these two methods are feasible, then aspirin is suggested.
Prognosis
DVT is most frequently a disease of older age that occurs in the context of nursing homes, hospitals, and active cancer. It is associated with a 30-daymortality rate
Mortality rate, or death rate, is a measure of the number of deaths (in general, or due to a specific cause) in a particular population, scaled to the size of that population, per unit of time. Mortality rate is typically expressed in units of d ...
of about 6%, with PE being the cause of most of these deaths. Proximal DVT is frequently associated with PE, unlike distal DVT, which is rarely if ever associated with PE. Around 56% of those with proximal DVT also have PE, although a chest CT is not needed simply because of the presence of DVT. If proximal DVT is left untreated, in the following 3 months approximately half of people will experience symptomatic PE.
Another frequent complication of proximal DVT, and the most frequent chronic complication, is post-thrombotic syndrome, where individuals have chronic venous symptoms. Symptoms can include pain, itching, swelling, paresthesia, a sensation of heaviness, and in severe cases, leg ulcers. After proximal DVT, an estimated 20–50% of people develop the syndrome, with 5–10% experiencing severe symptoms. Post-thrombotic syndrome can also be a complication of distal DVT, though to a lesser extent than with proximal DVT.
In the 10 years following an initial VTE, about 30% of people will have a recurrence. VTE recurrence in those with prior DVT is more likely to recur as DVT than PE. Cancer and unprovoked DVT are strong risk factors for recurrence. After initial proximal unprovoked DVT with and without PE, 16–17% of people will have recurrent VTE in the 2 years after they complete their course of anticoagulants. VTE recurrence is less common in distal DVT than proximal DVT. In upper extremity DVT, annual VTE recurrence is about 2–4%. After surgery, a provoked proximal DVT or PE has an annual recurrence rate of only 0.7%.
Epidemiology
About 1.5 out of 1000 adults a year have a first VTE in high-income countries. The condition becomes much more common with age. VTE rarely occurs in children, but when it does, it predominantly affects hospitalized children. Children in North America and the Netherlands have VTE rates that range from 0.07 to 0.49 out of 10,000 children annually. Meanwhile, almost 1% of those aged 85 and above experience VTE each year. About 60% of all VTEs occur in those 70 years of age or older. Incidence is about 18% higher in males than in females, though there are ages when VTE is more prevalent in women. VTE occurs in association with hospitalization or nursing home residence about 60% of the time, active cancer about 20% of the time, and a central venous catheter or transvenous pacemaker about 9% of the time. During pregnancy and after childbirth, acute VTE occurs in about 1.2 of 1000 deliveries. Despite it being relatively rare, it is a leading cause of maternal morbidity and mortality. After surgery with preventive treatment, VTE develops in about 10 of 1000 people after total or partial knee replacement, and in about 5 of 1000 after total or partial hip replacement. About 400,000 Americans develop an initial VTE each year, with 100,000 deaths or more attributable to PE. Asian, Asian-American, Native American, and Hispanic individuals have a lower VTE risk than Whites or Blacks. Populations in Asia have VTE rates at 15 to 20% of what is seen in Western countries, with an increase in incidence seen over time. In North American and European populations, around 4–8% of people have a thrombophilia, most commonly factor V leiden and prothrombin G20210A. For populations in China, Japan, and Thailand, deficiences in protein S, protein C, and antithrombin predominate. Non-O blood type is present in around 50% of the general population and varies with ethnicity, and it is present in about 70% of those with VTE. DVT occurs in the upper extremities in about 4–10% of cases, with an incidence of 0.4–1.0 people out of 10,000 a year. A minority of upper extremity DVTs are due to Paget–Schroetter syndrome, also called effort thrombosis, which occurs in 1–2 people out of 100,000 a year, usually in athletic males around 30 years of age or in those who do significant amounts of overhead manual labor.Social
 Being on blood thinners because of DVT can be life-changing because it can prevent lifestyle activities such as contact or winter sports to prevent bleeding after potential injuries. Head injuries prompting brain bleeds are of particular concern. This has caused NASCAR driver
Being on blood thinners because of DVT can be life-changing because it can prevent lifestyle activities such as contact or winter sports to prevent bleeding after potential injuries. Head injuries prompting brain bleeds are of particular concern. This has caused NASCAR driver Brian Vickers
Brian Lee Vickers (born October 24, 1983) is an American professional stock car and sports car racing driver. He last drove the No. 14 Chevrolet SS for Stewart-Haas Racing as an interim driver in the NASCAR Sprint Cup Series for the injured ...
to forego participation in races. Professional basketball players including NBA players Chris Bosh
Christopher Wesson Bosh (born March 24, 1984) is an American former professional basketball player. A Texas Mr. Basketball in high school, he played one season of college basketball for Georgia Tech before declaring for the 2003 NBA draft. Bo ...
and hall of famer Hakeem Olajuwon have dealt with recurrent blood clots, and Bosh's career was significantly hampered by DVT and PE.
Tennis star Serena Williams
Serena Jameka Williams (born September 26, 1981) is an American inactive professional tennis player. Considered among the greatest tennis players of all time, she was ranked world No. 1 in singles by the Women's Tennis Association (WTA) for ...
was hospitalized in 2011 for PE thought to have originated from DVT. Years later, in 2017, due to her knowledge of DVT and PE, Serena accurately advocated for herself to have a PE diagnosed and treated. During this encounter with VTE, she was hospitalized after a C-section
Caesarean section, also known as C-section or caesarean delivery, is the surgical procedure by which one or more babies are delivered through an incision in the mother's abdomen, often performed because vaginal delivery would put the baby or ...
surgery and was off of blood thinners. After feeling the sudden onset of a PE symptom, shortness of breath, she told her nurse and requested a CT scan and an IV heparin drip, all while gasping for air. She started to receive an ultrasound to look for DVT in the legs, prompting her to express dissatisfaction to the medical staff that they were not looking for clots where she had symptoms (her lungs), and they were not yet treating her presumed PE. After being diagnosed with PE and not DVT, and after receiving heparin by IV, the coughing from the PE caused her C-section surgical site to open and the heparin contributed to bleeding at the site. Serena later received an IVC filter while in the hospital.
Other notable people have been affected by DVT. Former United States (US) President Richard Nixon
Richard Milhous Nixon (January 9, 1913April 22, 1994) was the 37th president of the United States, serving from 1969 to 1974. A member of the Republican Party, he previously served as a representative and senator from California and was ...
had recurrent DVT, and so has former Secretary of State Hillary Clinton
Hillary Diane Rodham Clinton ( Rodham; born October 26, 1947) is an American politician, diplomat, and former lawyer who served as the 67th United States Secretary of State for President Barack Obama from 2009 to 2013, as a United States sen ...
. She was first diagnosed while First Lady in 1998 and again in 2009. Dick Cheney was diagnosed with an episode while Vice President
A vice president, also director in British English, is an officer in government or business who is below the president (chief executive officer) in rank. It can also refer to executive vice presidents, signifying that the vice president is on ...
, and TV show host Regis Philbin
Regis Francis Xavier Philbin (; August 25, 1931 – July 25, 2020)Archived aGhostarchiveand thWayback Machine was an American television presenter, talk show host, game show host, comedian, actor, and singer. Once called "the hardest working ma ...
had DVT after hip-replacement surgery. DVT has also contributed to the deaths of famous people. For example, DVT and PE played a role in rapper Heavy D
Dwight Arrington MyersCuda, Heidi Sigmund Keeping it reel. '' Vibe'' ("born Dwight Arrington Myers")Samuels, Anita M. (January 12' 1996)Heavy D, the C.E.O. ''New York Times'' (May 24, 1967 – November 8, 2011), known professionally as Hea ...
's death at age 44. NBC journalist David Bloom
David Jerome Bloom (May 22, 1963 – April 6, 2003) was an American television journalist (co-anchor of ''Weekend Today'' and reporter) until his sudden death in 2003 after a deep vein thrombosis (DVT) became a pulmonary embolism.
Early an ...
died at age 39 while covering the Iraq War from a PE that was thought to have progressed from a missed DVT, and actor Jimmy Stewart
James Maitland Stewart (May 20, 1908 – July 2, 1997) was an American actor and military pilot. Known for his distinctive drawl and everyman screen persona, Stewart's film career spanned 80 films from 1935 to 1991. With the strong morality h ...
had DVT that progressed to a PE when he was 89.
History
 The book '' Sushruta Samhita'', an Ayurvedic text published around 600–900 BC, contains what has been cited as the first description of DVT. In 1271, DVT symptoms in the leg of a 20-year-old male were described in a French manuscript, which has been cited as the first case or the first Western reference to DVT.
In 1856, German physician and pathologist
The book '' Sushruta Samhita'', an Ayurvedic text published around 600–900 BC, contains what has been cited as the first description of DVT. In 1271, DVT symptoms in the leg of a 20-year-old male were described in a French manuscript, which has been cited as the first case or the first Western reference to DVT.
In 1856, German physician and pathologist Rudolf Virchow
Rudolf Ludwig Carl Virchow (; or ; 13 October 18215 September 1902) was a German physician, anthropologist, pathologist, prehistorian, biologist, writer, editor, and politician. He is known as "the father of modern pathology" and as the founder ...
published his analysis after the insertion of foreign bodies into the jugular veins of dogs, which migrated to the pulmonary arteries. These foreign bodies caused pulmonary emboli, and Virchow was focused on explaining their consequences. He cited three factors, which are now understood as hypercoaguability, stasis, and endothelial injury. It was not until 1950 that this framework was cited as Virchow's triad, but the teaching of Virchow's triad has continued in light of its utility as a theoretical framework and as a recognition of the significant progress Virchow made in expanding the understanding of VTE.
Methods to observe DVT by ultrasound were established in the 1960s. Diagnoses were commonly performed by impedance plethysmography
Impedance cardiography (ICG) is a non-invasive technology measuring total electrical conductivity of the thorax and its changes in time to process continuously a number of cardiodynamic parameters, such as stroke volume (SV), heart rate (HR), car ...
in the 1970s and 1980s, but ultrasound, particularly after utility of probe compression was demonstrated in 1986, became the preferred diagnostic method. Yet, in the mid-1990s, contrast venography and impedance plethysmography were still described as common.
 Multiple pharmacological therapies for DVT were introduced in the 20th century: oral anticoagulants in the 1940s, subcutaneous injections of LDUH in 1962 and subcutaneous injections of LMWH in 1982. 1974 was when vascular inflammation and venous thrombosis were first proposed to be interrelated. For around 50 years, a months-long warfarin (Coumadin) regimen was the mainstay of pharmacological treatment. To avoid the blood monitoring required with warfarin and the injections required by heparin and heparin-like medicines, direct oral anticoagulants (DOACs) were developed. In the late 2000s to early 2010s, DOACs—including rivaroxaban (Xarelto), apixaban (Eliquis), and dabigatran (Pradaxa)—came to the market. ''The New York Times'' described a "furious battle" among the three makers of these drugs "for the prescription pads of doctors".
Multiple pharmacological therapies for DVT were introduced in the 20th century: oral anticoagulants in the 1940s, subcutaneous injections of LDUH in 1962 and subcutaneous injections of LMWH in 1982. 1974 was when vascular inflammation and venous thrombosis were first proposed to be interrelated. For around 50 years, a months-long warfarin (Coumadin) regimen was the mainstay of pharmacological treatment. To avoid the blood monitoring required with warfarin and the injections required by heparin and heparin-like medicines, direct oral anticoagulants (DOACs) were developed. In the late 2000s to early 2010s, DOACs—including rivaroxaban (Xarelto), apixaban (Eliquis), and dabigatran (Pradaxa)—came to the market. ''The New York Times'' described a "furious battle" among the three makers of these drugs "for the prescription pads of doctors".
Economics
VTE costs the US healthcare system about $7 to 10 billion dollars annually. Initial and average DVT costs for a hospitalized US patient is about $10,000 (2015 estimate). In Europe, the costs for an initial VTE hospitalization are significantly less, costing about €2000 to 4000 (2011 estimate). Post-thrombotic syndrome is a significant contributor to DVT follow-up costs. Outpatient treatment significantly reduces costs, and treatment costs for PE exceed those of DVT.Research directions
A 2019 study published in ''Nature Genetics'' reported more than doubling the known genetic loci associated with VTE. In their updated 2018 clinical practice guidelines, the American Society of Hematology identified 29 separate research priorities, most of which related to patients who are acutely or critically ill. Inhibition offactor XI
Factor XI or plasma thromboplastin antecedent is the zymogen form of factor XIa, one of the enzymes of the coagulation cascade. Like many other coagulation factors, it is a serine protease. In humans, Factor XI is encoded by the ''F11'' gene.
...
, P-selectin
P-selectin is a type-1 transmembrane protein that in humans is encoded by the SELP gene.
P-selectin functions as a cell adhesion molecule (CAM) on the surfaces of activated endothelial cells, which line the inner surface of blood vessels, and act ...
, E-selectin
E-selectin, also known as CD62 antigen-like family member E (CD62E), endothelial-leukocyte adhesion molecule 1 (ELAM-1), or leukocyte-endothelial cell adhesion molecule 2 (LECAM2), is a selectin cell adhesion molecule expressed only on endothelial ...
, and a reduction in formation of neutrophil extracellular traps
Neutrophil extracellular traps (NETs) are networks of extracellular fibers, primarily composed of DNA from neutrophils, which bind pathogens. Neutrophils are the immune system's first line of defense against infection and have conventionally be ...
are potential therapies that might treat VTE without increasing bleeding risk.
Notes
References
Cited literature * * {{Vascular diseases Coagulopathies Diseases of veins, lymphatic vessels and lymph nodes Hematology Wikipedia medicine articles ready to translate