Diathermy on:
[Wikipedia]
[Google]
[Amazon]
Diathermy is electrically induced heat or the use of high-frequency electromagnetic currents as a form of physical therapy and in surgical procedures. The earliest observations on the reactions of high-frequency electromagnetic currents upon the human organism were made by
Jacques Arsene d'Arsonval
Ancient and noble French family names, Jacques, Jacq, or James are believed to originate from the Middle Ages in the historic northwest Brittany region in France, and have since spread around the world over the centuries. To date, there are over ...
. The field was pioneered in 1907 by German physician Karl Franz Nagelschmidt, who coined the term ''diathermy'' from the Greek words ''dia'' and θέρμη ''therma'', literally meaning "heating through" (adj., diather´mal, diather´mic).
Diathermy is commonly used for muscle relaxation, and to induce deep heating in tissue for therapeutic purposes in medicine. It is used in physical therapy to deliver moderate heat directly to pathologic lesions in the deeper tissues of the body.
Diathermy is produced by three techniques: ultrasound
Ultrasound is sound waves with frequencies higher than the upper audible limit of human hearing. Ultrasound is not different from "normal" (audible) sound in its physical properties, except that humans cannot hear it. This limit varies ...
(''ultrasonic diathermy''), short-wave radio frequencies in the range 1–100 MHz (''shortwave diathermy'') or microwave
Microwave is a form of electromagnetic radiation with wavelengths ranging from about one meter to one millimeter corresponding to frequencies between 300 MHz and 300 GHz respectively. Different sources define different frequency ra ...
s typically in the 915 MHz or 2.45 GHz bands (''microwave diathermy''), the methods differing mainly in their penetration capability. It exerts physical effects and elicits a spectrum of physiological responses.
The same techniques are also used to create higher tissue temperatures to destroy neoplasm
A neoplasm () is a type of abnormal and excessive growth of tissue. The process that occurs to form or produce a neoplasm is called neoplasia. The growth of a neoplasm is uncoordinated with that of the normal surrounding tissue, and persists ...
s (cancer and tumors), warts, and infected tissues; this is called hyperthermia treatment
Hyperthermia therapy ''(or hyperthermia, or thermotherapy)'' is a type of medical treatment in which body tissue is exposed to temperatures above body temperature, in the region of 40–45 °C (104–113 °F). Hyperthermia is usually ...
. In surgery diathermy is used to cauterize
Cauterization (or cauterisation, or cautery) is a medical practice or technique of burning a part of a body to remove or close off a part of it. It destroys some tissue in an attempt to mitigate bleeding and damage, remove an undesired growth, o ...
blood vessels to prevent excessive bleeding. The technique is particularly valuable in neurosurgery and surgery of the eye.
History
The idea that high-frequency electromagnetic currents could have therapeutic effects was explored independently around the same time (1890–1891) by French physician and biophysicistJacques Arsene d'Arsonval
Ancient and noble French family names, Jacques, Jacq, or James are believed to originate from the Middle Ages in the historic northwest Brittany region in France, and have since spread around the world over the centuries. To date, there are over ...
and Serbian American engineer Nikola Tesla
Nikola Tesla ( ; ,"Tesla"
''
''
J. W. Hand,"Biophysics and Technology of Electromagnetic Hyperthermia" in d'Arsonval had been studying medical applications for electricity in the 1880s and performed the first systematic studies in 1890 of the effect of alternating current on the body, and discovered that frequencies above 10 kHz did not cause the physiological reaction of electric shock, but warming., translated by J. H. Kellogg He also developed the three methods that have been used to apply high-frequency current to the body: contact electrodes, capacitive plates, and inductive coils.
Nikola Tesla
Nikola Tesla ( ; ,"Tesla"
''
''
By 1900 application of high-frequency current to the body was used experimentally to treat a wide variety of medical conditions in the new medical field of ''
electrotherapy
Electrotherapy is the use of electrical energy as a medical treatment. In medicine, the term ''electrotherapy'' can apply to a variety of treatments, including the use of electrical devices such as deep brain stimulators for neurological dise ...
''. In 1899 Austrian chemist von Zaynek determined the rate of heat production in tissue as a function of frequency and current density, and first proposed using high-frequency currents for deep heating therapy. In 1908 German physician Karl Franz Nagelschmidt coined the term ''diathermy'', and performed the first extensive experiments on patients. Nagelschmidt is considered the founder of the field. He wrote the first textbook on diathermy in 1913, which revolutionized the field.
Until the 1920s noisy spark-discharge Tesla coil
A Tesla coil is an electrical resonant transformer circuit designed by inventor Nikola Tesla in 1891. It is used to produce high-voltage, low- current, high-frequency alternating-current electricity. Tesla experimented with a number of differen ...
and Oudin coil
An Oudin coil, also called an Oudin oscillator or Oudin resonator, is a resonant transformer circuit that generates very high tension, high frequency alternating current (AC) electricity at low current levels, used in the obsolete forms of elec ...
machines were used. These were limited to frequencies of 0.1–2 MHz, called "longwave" diathermy. The current was applied directly to the body with contact electrodes, which could cause skin burns. In the 1920s the development of vacuum tube
A vacuum tube, electron tube, valve (British usage), or tube (North America), is a device that controls electric current flow in a high vacuum between electrodes to which an electric potential difference has been applied.
The type known as ...
machines allowed frequencies to be increased to 10–300 MHz, called "shortwave" diathermy. The energy was applied to the body with inductive coils of wire or capacitive plates insulated from the body, which reduced the risk of burns. By the 1940s microwave
Microwave is a form of electromagnetic radiation with wavelengths ranging from about one meter to one millimeter corresponding to frequencies between 300 MHz and 300 GHz respectively. Different sources define different frequency ra ...
s were being used experimentally.
Uses
Physical therapy
The three forms of diathermy employed by physical therapists areultrasound
Ultrasound is sound waves with frequencies higher than the upper audible limit of human hearing. Ultrasound is not different from "normal" (audible) sound in its physical properties, except that humans cannot hear it. This limit varies ...
, short wave and microwave
Microwave is a form of electromagnetic radiation with wavelengths ranging from about one meter to one millimeter corresponding to frequencies between 300 MHz and 300 GHz respectively. Different sources define different frequency ra ...
. The application of moderate heat by diathermy increases blood flow and speeds up metabolism and the rate of ion diffusion across cellular membranes. The fibrous tissues in tendons, joint capsules, and scars are more easily stretched when subjected to heat, thus facilitating the relief of stiffness of joints and promoting relaxation of the muscles and decrease of muscle spasms.
Ultrasound
Ultrasound diathermy employs high-frequency acoustic vibrations which, when propelled through the tissues, are converted into heat. This type of diathermy is especially useful in the delivery of heat to selected musculatures and structures because there is a difference in the sensitivity of various fibers to the acoustic vibrations; some are more absorptive and some are more reflective. For example, in subcutaneous fat, relatively little energy is converted into heat, but in muscle tissues there is a much higher rate of conversion to heat. The therapeutic ultrasound apparatus generates a high-frequency alternating current, which is then converted into acoustic vibrations. The apparatus is moved slowly across the surface of the part being treated. Ultrasound is a very effective agent for the application of heat, but it should be used only by a therapist who is fully aware of its potential hazards and the contraindications for its use.Short wave
Short wave diathermy machines use two condenser plates that are placed on either side of the body part to be treated. Another mode of application is by induction coils that are pliable and can be molded to fit the part of the body under treatment. As the high-frequency waves travel through the body tissues between the condensers or the coils, they are converted into heat. The degree of heat and depth of penetration depend in part on the absorptive and resistance properties of the tissues that the waves encounter. Short wave diathermy operations use theISM band
The ISM radio bands are portions of the radio spectrum reserved internationally for industrial, scientific and medical (ISM) purposes, excluding applications in telecommunications.
Examples of applications for the use of radio frequency (RF) ener ...
frequencies of 13.56, 27.12, and 40.68 megahertz. Most commercial machines operate at a frequency of 27.12 MHz, a wavelength of approximately 11 meters.
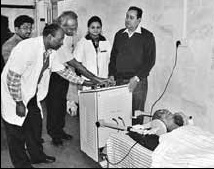
Short wave diathermy usually is prescribed for treatment of deep muscles and joints that are covered with a heavy soft-tissue mass, for example, the hip. In some instances short wave diathermy may be applied to localize deep inflammatory processes, as in pelvic inflammatory disease. Short wave diathermy can also be used for hyperthermia therapy, as an adjuvant to radiation in cancer treatment. Typically, hyperthermia would be added twice a week before radiation, as shown in the photograph from a 2010 clinical trial at Mahavir Cancer Sansthan
Mahavira (Sanskrit: महावीर) also known as Vardhaman, was the 24th ''tirthankara'' (supreme preacher) of Jainism. He was the spiritual successor of the 23rd ''tirthankara'' Parshvanatha. Mahavira was born in the early part of the 6 ...
in Patna, India. 
Microwave
Microwave diathermy usesmicrowave
Microwave is a form of electromagnetic radiation with wavelengths ranging from about one meter to one millimeter corresponding to frequencies between 300 MHz and 300 GHz respectively. Different sources define different frequency ra ...
s, radio waves which are higher in frequency
Frequency is the number of occurrences of a repeating event per unit of time. It is also occasionally referred to as ''temporal frequency'' for clarity, and is distinct from ''angular frequency''. Frequency is measured in hertz (Hz) which is eq ...
and shorter in wavelength
In physics, the wavelength is the spatial period of a periodic wave—the distance over which the wave's shape repeats.
It is the distance between consecutive corresponding points of the same phase on the wave, such as two adjacent crests, t ...
than the short waves above. Microwaves, which are also used in radar
Radar is a detection system that uses radio waves to determine the distance ('' ranging''), angle, and radial velocity of objects relative to the site. It can be used to detect aircraft, ships, spacecraft, guided missiles, motor vehicles, we ...
, have a frequency above 300 MHz and a wavelength less than one meter. Most, if not all, of the therapeutic effects of microwave therapy are related to the conversion of energy into heat and its distribution throughout the body tissues. This mode of diathermy is considered to be the easiest to use, but the microwaves have a relatively poor depth of penetration.
Microwaves cannot be used in high dosage on edematous tissue, over wet dressings, or near metallic implants in the body because of the danger of local burns. Microwaves and short waves cannot be used on or near persons with implanted electronic cardiac pacemakers.
Hyperthermia
Hyperthermia, also known simply as overheating, is a condition in which an individual's body temperature is elevated beyond normal due to failed thermoregulation. The person's body produces or absorbs more heat than it dissipates. When extreme ...
induced by microwave diathermy raises the temperature of deep tissues from 41 °C to 45 °C using electromagnetic power. The biological mechanism that regulates the relationship between the thermal dose and the healing process of soft tissues with low or high water content or with low or high blood perfusion is still under study. Microwave diathermy treatment at 434 and 915 MHz can be effective in the short-term management of musculo-skeletal injuries.
Hyperthermia is safe if the temperature is kept under 45 °C or 113 °F. The absolute temperature is, however, not sufficient to predict the damage that it may produce.
Microwave diathermy-induced hyperthermia produced short-term pain relief in established supraspinatus tendinopathy.
The physical characteristics of most of the devices used clinically to heat tissues have been proved to be inefficient to reach the necessary therapeutic heating patterns in the range of depth of the damage tissue. The preliminary studies performed with new microwave devices working at 434 MHz have demonstrated encouraging results. Nevertheless, adequately designed prospective-controlled clinical studies need to be completed to confirm the therapeutic effectiveness of hyperthermia with large number of patients, longer-term follow-up and mixed populations.
Microwave diathermy is used in the management of superficial tumours with conventional radiotherapy and chemotherapy
Chemotherapy (often abbreviated to chemo and sometimes CTX or CTx) is a type of cancer treatment that uses one or more anti-cancer drugs ( chemotherapeutic agents or alkylating agents) as part of a standardized chemotherapy regimen. Chemothe ...
. Hyperthermia has been used in oncology for more than 35 years, in addition to radiotherapy, in the management of different tumours. In 1994, hyperthermia was introduced in several countries of the European Union as a modality for use in physical medicine and sports traumatology. Its use has been successfully extended to physical medicine and sports traumatology in Central and Southern Europe.
Surgery
''Surgical diathermy'' is usually better known as "electrosurgery
Electrosurgery is the application of a high-frequency (radio frequency) alternating polarity, electrical current to biological tissue as a means to cut, coagulate, desiccate, or fulgurate tissue.Hainer BL, "Fundamentals of electrosurgery", ''J ...
". (It is also referred to occasionally as "electrocautery
Cauterization (or cauterisation, or cautery) is a medical practice or technique of burning a part of a body to remove or close off a part of it. It destroys some tissue in an attempt to mitigate bleeding and damage, remove an undesired growth, o ...
", but see disambiguation below.) Electrosurgery and surgical diathermy involve the use of high-frequency A.C. electric current in surgery as either a cutting modality, or else to cauterize small blood vessels to stop bleeding. This technique induces localized tissue burning and damage, the zone of which is controlled by the frequency and power of the device.
Some sources insist that electrosurgery
Electrosurgery is the application of a high-frequency (radio frequency) alternating polarity, electrical current to biological tissue as a means to cut, coagulate, desiccate, or fulgurate tissue.Hainer BL, "Fundamentals of electrosurgery", ''J ...
be applied to surgery accomplished by high-frequency alternating current (AC) cutting, and that "electrocautery
Cauterization (or cauterisation, or cautery) is a medical practice or technique of burning a part of a body to remove or close off a part of it. It destroys some tissue in an attempt to mitigate bleeding and damage, remove an undesired growth, o ...
" be used only for the practice of cauterization with heated nichrome wires powered by direct current (DC), as in the handheld battery-operated portable cautery tools.
Types
Diathermy used in surgery is of typically two types. *Monopolar, where electric current passes from one electrode near the tissue to be treated to other fixed electrode (indifferent electrode) elsewhere in the body. Usually this type of electrode is placed in contact with buttocks or around the leg. *Bipolar, where both electrodes are mounted on same pen-like device and electric current passes only through the tissue being treated. Advantage of bipolar electrosurgery is that it prevents the flow of current through other tissues of the body and focuses only on the tissue in contact. This is useful inmicrosurgery
Microsurgery is a general term for surgery requiring an operating microscope. The most obvious developments have been procedures developed to allow anastomosis of successively smaller blood vessels and nerves (typically 1 mm in diameter) whic ...
and in patients with a cardiac pacemaker
350px, Image showing the cardiac pacemaker or SA node, the primary pacemaker within the electrical_conduction_system_of_the_heart">SA_node,_the_primary_pacemaker_within_the_electrical_conduction_system_of_the_heart.
The_muscle_contraction.htm ...
.
Diathermy risks
Burns from electrocautery generally arise from a faulty grounding pad or from an outbreak of a fire. Monopolar electrocautery works because radio frequency energy is concentrated by the surgical instrument's small surface area. The electrical circuit is completed by passing current through the patient's body to a conductive pad that is connected to the radio frequency generator. Because the pad's surface area is large relative to the instrument's tip, energy density across the pad is reliably low enough that no tissue injury occurs at the pad site. Electrical shocks and burns are possible, however, if the circuit is interrupted or energy is concentrated in some way. This can happen if the pad surface in contact is small, e.g. if the pad's electrolytic gel is dry, if the pad becomes disconnected from the radio frequency generator, or via a metal implant. Modern electrocautery systems are equipped with sensors to detect high resistance in the circuit that can prevent some injuries. As with all forms of heat applications, care must be taken to avoid burns during diathermy treatments, especially in patients with decreased sensitivity to heat and cold. With electrocautery there have been reported cases of flash fires in the operating theatre related to heat generation meeting chemical flash points, especially in the presence of increased oxygen concentrations associated with anaesthetic. Concerns have also been raised regarding the toxicity of surgical smoke produced by electrocautery. This has been shown to contain chemicals which may cause harm to patients, surgeons and/or operating theatre staff. For patients that have a surgically implantedspinal cord stimulator
A spinal cord stimulator (SCS) or dorsal column stimulator (DCS) is a type of implantable neuromodulation device (sometimes called a "pain pacemaker") that is used to send electrical signals to select areas of the spinal cord (dorsal columns) for ...
(SCS) system, diathermy can cause tissue damage through energy that is transferred into the implanted SCS components resulting in severe injury or death.
Military
Medical diathermy devices were used to cause interference to German radio beams used for targeting nighttime bombing raids in World War II during theBattle of the Beams
The Battle of the Beams was a period early in the Second World War when bombers of the German Air Force ('' Luftwaffe'') used a number of increasingly accurate systems of radio navigation for night bombing in the United Kingdom. British scientif ...
.
See also
*Dielectric heating
Dielectric heating, also known as electronic heating, radio frequency heating, and high-frequency heating, is the process in which a radio frequency (RF) alternating electric field, or radio wave or microwave electromagnetic radiation heats a die ...
* Heat therapy
Heat therapy, also called thermotherapy, is the use of heat in therapy, such as for pain relief and health. It can take the form of a hot cloth, hot water bottle, ultrasound, heating pad, hydrocollator packs, whirlpool baths, cordless FIR h ...
* Pulsed electromagnetic field therapy
Pulsed electromagnetic field therapy (PEMFT, or PEMF therapy), also known as low field magnetic stimulation (LFMS) uses electromagnetic fields in an attempt to heal non-union fractures and depression. By 2007 the FDA had cleared several such sti ...
References
{{Physical therapy and rehabilitation Electric heating Medical equipment