The lungs are the primary
organs of the
respiratory system
The respiratory system (also respiratory apparatus, ventilatory system) is a biological system consisting of specific organs and structures used for gas exchange in animals and plants. The anatomy and physiology that make this happen varies grea ...
in many animals, including humans. In
mammal
A mammal () is a vertebrate animal of the Class (biology), class Mammalia (). Mammals are characterised by the presence of milk-producing mammary glands for feeding their young, a broad neocortex region of the brain, fur or hair, and three ...
s and most other
tetrapod
A tetrapod (; from Ancient Greek :wiktionary:τετρα-#Ancient Greek, τετρα- ''(tetra-)'' 'four' and :wiktionary:πούς#Ancient Greek, πούς ''(poús)'' 'foot') is any four-Limb (anatomy), limbed vertebrate animal of the clade Tetr ...
s, two lungs are located near the
backbone on either side of the
heart
The heart is a muscular Organ (biology), organ found in humans and other animals. This organ pumps blood through the blood vessels. The heart and blood vessels together make the circulatory system. The pumped blood carries oxygen and nutrie ...
. Their function in the respiratory system is to extract oxygen from the atmosphere and transfer it into the bloodstream, and to release
carbon dioxide
Carbon dioxide is a chemical compound with the chemical formula . It is made up of molecules that each have one carbon atom covalent bond, covalently double bonded to two oxygen atoms. It is found in a gas state at room temperature and at norma ...
from the bloodstream into the atmosphere, in a process of
gas exchange. Respiration is driven by different muscular systems in different species. Mammals, reptiles and birds use their musculoskeletal systems to support and foster breathing. In early tetrapods, air was driven into the lungs by the pharyngeal muscles via
buccal pumping, a mechanism still seen in amphibians. In humans, the primary muscle that drives breathing is the
diaphragm. The lungs also provide airflow that makes
vocalisation including
speech
Speech is the use of the human voice as a medium for language. Spoken language combines vowel and consonant sounds to form units of meaning like words, which belong to a language's lexicon. There are many different intentional speech acts, suc ...
possible.
Humans have two lungs, a right lung and a left lung. They are situated within the thoracic cavity of the
chest. The right lung is bigger than the left, and the left lung shares space in the chest with the heart. The lungs together weigh approximately 1.3 kilograms (2.9 lb), and the right is heavier. The lungs are part of the
lower respiratory tract that begins at the
trachea
The trachea (: tracheae or tracheas), also known as the windpipe, is a cartilaginous tube that connects the larynx to the bronchi of the lungs, allowing the passage of air, and so is present in almost all animals' lungs. The trachea extends from ...
and branches into the
bronchi and
bronchioles, which receive air
breathed in via the
conducting zone. These divide until air reaches microscopic
alveoli, where gas exchange takes place. Together, the lungs contain approximately 2,400 kilometers (1,500 mi) of airways and 300 to 500 million alveoli. Each lung is enclosed within a
pleural sac of two
pleurae which allows the inner and outer walls to slide over each other whilst breathing takes place, without much friction. The inner
visceral pleura divides each lung as
fissures into sections called lobes. The right lung has three lobes and the left has two. The lobes are further divided into
bronchopulmonary segments and lobules. The lungs have a unique blood supply, receiving deoxygenated blood sent from the heart to receive oxygen (the
pulmonary circulation) and a separate supply of oxygenated blood (the
bronchial circulation).
The tissue of the lungs can be affected by several
respiratory diseases including
pneumonia and
lung cancer. Chronic diseases such as
chronic obstructive pulmonary disease and
emphysema can be related to smoking or exposure to harmful substances. Diseases such as bronchitis can also affect the respiratory tract. Medical terms related to the lung often begin with pulmo-, from the Latin pulmonarius (of the lungs) as in pulmonology, or with pneumo- (from Greek πνεύμων "lung") as in pneumonia.
In
embryonic development
In developmental biology, animal embryonic development, also known as animal embryogenesis, is the developmental stage of an animal embryo. Embryonic development starts with the fertilization of an egg cell (ovum) by a sperm, sperm cell (spermat ...
, the lungs begin to develop as an outpouching of the
foregut, a tube which goes on to form the upper part of the
digestive system
The human digestive system consists of the gastrointestinal tract plus the accessory organs of digestion (the tongue, salivary glands, pancreas, liver, and gallbladder). Digestion involves the breakdown of food into smaller and smaller compone ...
. When the lungs are formed the
fetus
A fetus or foetus (; : fetuses, foetuses, rarely feti or foeti) is the unborn offspring of a viviparous animal that develops from an embryo. Following the embryonic development, embryonic stage, the fetal stage of development takes place. Pren ...
is held in the fluid-filled
amniotic sac
The amniotic sac, also called the bag of waters or the membranes, is the sac in which the embryo and later fetus develops in amniotes. It is a thin but tough transparent pair of biological membrane, membranes that hold a developing embryo (and l ...
and so they do not function to breathe. Blood is also diverted from the lungs through the
ductus arteriosus.
At birth however, air begins to pass through the lungs, and the diversionary duct closes so that the lungs can begin to respire. The lungs only fully develop in early childhood.
Structure
Anatomy
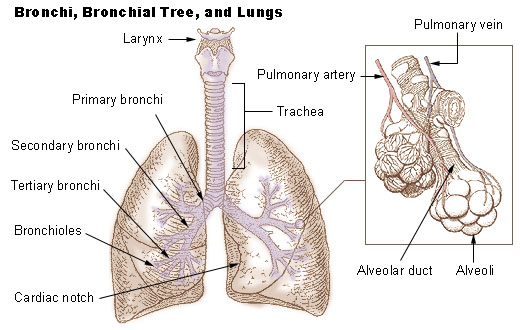
In humans, the lungs are located in the
chest on either side of the
heart
The heart is a muscular Organ (biology), organ found in humans and other animals. This organ pumps blood through the blood vessels. The heart and blood vessels together make the circulatory system. The pumped blood carries oxygen and nutrie ...
in the
rib cage. They are conical in shape with a narrow rounded apex at the top, and a broad concave base that rests on the convex surface of the
diaphragm.
The apex of the lung extends into the root of the neck, reaching shortly above the level of the
sternal end of the
first rib. The lungs stretch from close to the
backbone in the rib cage to the front of the
chest and downwards from the lower part of the trachea to the diaphragm.
The left lung shares space with the heart, and has an indentation in its border called the cardiac notch of the left lung to accommodate this.
The front and outer sides of the lungs face the ribs, which make light indentations on their surfaces. The medial surfaces of the lungs face towards the centre of the chest, and lie against the heart,
great vessels, and the
carina where the trachea divides into the two main bronchi.
The cardiac impression is an indentation formed on the surfaces of the lungs where they rest against the heart.
Both lungs have a central recession called the
hilum, where the
blood vessel
Blood vessels are the tubular structures of a circulatory system that transport blood throughout many Animal, animals’ bodies. Blood vessels transport blood cells, nutrients, and oxygen to most of the Tissue (biology), tissues of a Body (bi ...
s and
airways pass into the lungs making up the
root of the lung.
There are also
bronchopulmonary lymph nodes on the hilum.
The lungs are surrounded by the
pulmonary pleurae
The pleurae (: pleura) are the two flattened closed sacs filled with pleural fluid, each ensheathing each lung and lining their surrounding tissues, locally appearing as two opposing layers of serous membrane separating the lungs from the medias ...
. The pleurae are two
serous membranes; the outer
parietal pleura lines the inner wall of the
rib cage and the inner
visceral pleura directly lines the surface of the lungs. Between the pleurae is a
potential space called the
pleural cavity containing a thin layer of lubricating
pleural fluid.
Lobes
Each lung is divided into sections called lobes by the infoldings of the visceral pleura as fissures. Lobes are divided into segments, and segments have further divisions as lobules. There are three lobes in the right lung and two lobes in the left lung.
Fissures
The fissures are formed in early
prenatal development
Prenatal development () involves the development of the embryo and of the fetus during a viviparous animal's gestation. Prenatal development starts with fertilization, in the germinal stage of embryonic development, and continues in fetal de ...
by invaginations of the visceral pleura that divide the lobar bronchi, and section the lungs into lobes that helps in their expansion.
The right lung is divided into three lobes by a horizontal fissure, and an oblique fissure. The left lung is divided into two lobes by an oblique fissure which is closely aligned with the oblique fissure in the right lung. In the right lung the upper horizontal fissure, separates the upper (superior) lobe from the middle lobe. The lower, oblique fissure separates the lower lobe from the middle and upper lobes.
in the fissures are fairly common being either incompletely formed or present as an extra fissure as in the
azygos fissure, or absent. Incomplete fissures are responsible for
interlobar collateral ventilation, airflow between lobes which is unwanted in some
lung volume reduction procedures.
Segments
The primary bronchi enter the lungs at the hilum and initially branch into
secondary bronchi also known as lobar bronchi that supply air to each lobe of the lung. The lobar bronchi branch into
tertiary bronchi also known as segmental bronchi and these supply air to the further divisions of the lobes known as
bronchopulmonary segments. Each bronchopulmonary segment has its own (segmental) bronchus and
arterial supply. Segments for the left and right lung are shown in the table.
The segmental anatomy is useful clinically for localising disease processes in the lungs.
A segment is a discrete unit that can be surgically removed without seriously affecting surrounding tissue.
Right lung
The right lung has both more lobes and segments than the left. It is divided into three lobes, an upper, middle, and a lower lobe by two fissures, one oblique and one horizontal.
The upper, horizontal fissure, separates the upper from the middle lobe. It begins in the lower oblique fissure near the posterior border of the lung, and, running horizontally forward, cuts the anterior border on a level with the
sternal end of the fourth
costal cartilage; on the
mediastinal surface it may be traced back to the
hilum.
The lower, oblique fissure, separates the lower from the middle and upper lobes and is closely aligned with the oblique fissure in the left lung.
The mediastinal surface of the right lung is indented by a number of nearby structures. The heart sits in an impression called the cardiac impression. Above the hilum of the lung is an arched groove for the
azygos vein, and above this is a wide groove for the
superior vena cava and right
brachiocephalic vein; behind this, and close to the top of the lung is a groove for the
brachiocephalic artery. There is a groove for the
oesophagus
The esophagus (American English), oesophagus (British English), or œsophagus ( archaic spelling) ( see spelling difference) all ; : ((o)e)(œ)sophagi or ((o)e)(œ)sophaguses), colloquially known also as the food pipe, food tube, or gullet, ...
behind the hilum and the
pulmonary ligament, and near the lower part of the oesophageal groove is a deeper groove for the
inferior vena cava
The inferior vena cava is a large vein that carries the deoxygenated blood from the lower and middle body into the right atrium of the heart. It is formed by the joining of the right and the left common iliac veins, usually at the level of the ...
before it enters the heart.
[Alt URL]
/ref>
The weight of the right lung varies between individuals, with a standard reference range in men of
Left lung
The left lung is divided into two lobes, an upper and a lower lobe, by the oblique fissure, which extends from the costal to the mediastinal surface of the lung both above and below the hilum.
Illustrations
File:CT-Thorax-5.0-B70f-Lungs.jpg, Chest CT (axial lung window)
File:COR-2-STND-CHEST-LUNGS.jpg, Chest CT (coronal lung window)
File:CT-Thorax-5.0-B70f.ogg, Chest CT (axial lung window)
File:COR-2-STND-CHEST.ogg, Chest CT (coronal lung window)
File:Meet the lungs.webm, "Meet the lungs" from Khan Academy
File:MP1 Pulmonology.webm, Pulmonology video
File:Lobes of the Lung ogg.mov (1).ogg, 3D anatomy of the lung lobes and fissures.
Microanatomy
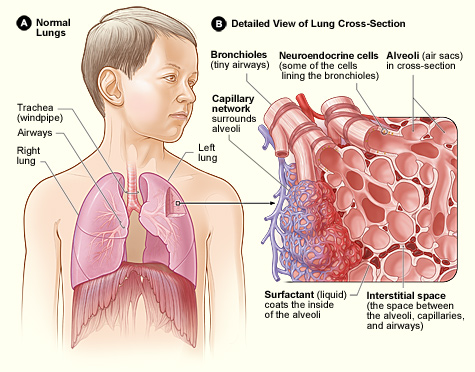 The lungs are part of the lower respiratory tract, and accommodate the bronchial airways when they branch from the trachea. The bronchial airways terminate in alveoli which make up the functional tissue ( parenchyma) of the lung, and veins, arteries, nerves, and
The lungs are part of the lower respiratory tract, and accommodate the bronchial airways when they branch from the trachea. The bronchial airways terminate in alveoli which make up the functional tissue ( parenchyma) of the lung, and veins, arteries, nerves, and lymphatic vessel
The lymphatic vessels (or lymph vessels or lymphatics) are thin-walled vessels (tubes), structured like blood vessels, that carry lymph. As part of the lymphatic system, lymph vessels are complementary to the cardiovascular system. Lymph vessel ...
s.
Connective tissue

 The connective tissue of the lungs is made up of
The connective tissue of the lungs is made up of elastic
Elastic is a word often used to describe or identify certain types of elastomer, Elastic (notion), elastic used in garments or stretch fabric, stretchable fabrics.
Elastic may also refer to:
Alternative name
* Rubber band, ring-shaped band of rub ...
and collagen fibres that are interspersed between the capillaries and the alveolar walls. Elastin
Elastin is a protein encoded by the ''ELN'' gene in humans and several other animals. Elastin is a key component in the extracellular matrix of gnathostomes (jawed vertebrates). It is highly Elasticity (physics), elastic and present in connective ...
is the key protein
Proteins are large biomolecules and macromolecules that comprise one or more long chains of amino acid residue (biochemistry), residues. Proteins perform a vast array of functions within organisms, including Enzyme catalysis, catalysing metab ...
of the extracellular matrix and is the main component of the elastic fibres.[
]
Respiratory epithelium
All of the lower respiratory tract including the trachea, bronchi, and bronchioles is lined with respiratory epithelium. This is a ciliated epithelium interspersed with goblet cell
Goblet cells are simple columnar epithelial cells that secrete gel-forming mucins, like mucin 2 in the lower gastrointestinal tract, and mucin 5AC in the respiratory tract. The goblet cells mainly use the merocrine method of secretion, secre ...
s which produce mucin
Mucins () are a family of high molecular weight, heavily glycosylated proteins ( glycoconjugates) produced by epithelial tissues in most animals. Mucins' key characteristic is their ability to form gels; therefore they are a key component in ...
the main component of mucus, ciliated cells, basal cells, and in the terminal bronchioles– club cells with actions similar to basal cells, and macrophage
Macrophages (; abbreviated MPhi, φ, MΦ or MP) are a type of white blood cell of the innate immune system that engulf and digest pathogens, such as cancer cells, microbes, cellular debris and foreign substances, which do not have proteins that ...
s. The epithelial cells, and the submucosal glands throughout the respiratory tract secrete airway surface liquid (ASL), the composition of which is tightly regulated and determines how well mucociliary clearance works.
Pulmonary neuroendocrine cells are found throughout the respiratory epithelium including the alveolar epithelium,
Bronchial airways
In the bronchi there are incomplete tracheal rings of cartilage and smaller plates of cartilage that keep them open.
Respiratory zone
The conducting zone of the respiratory tract ends at the terminal bronchioles when they branch into the respiratory bronchioles. This marks the beginning of the terminal respiratory unit called the acinus which includes the respiratory bronchioles, the alveolar ducts, alveolar sacs, and alveoli.[ A primary pulmonary lobule is the part of the lung distal to the respiratory bronchiole.][ The lobule is supplied by a terminal bronchiole that branches into respiratory bronchioles. The respiratory bronchioles supply the alveoli in each acinus and is accompanied by a pulmonary artery branch. Each lobule is enclosed by an interlobular septum. Each acinus is incompletely separated by an intralobular septum.][ The walls of the alveoli are extremely thin allowing a fast rate of ]diffusion
Diffusion is the net movement of anything (for example, atoms, ions, molecules, energy) generally from a region of higher concentration to a region of lower concentration. Diffusion is driven by a gradient in Gibbs free energy or chemical p ...
. The alveoli have interconnecting small air passages in their walls known as the pores of Kohn.[
]
Alveoli

 Alveoli consist of two types of alveolar cell and an
Alveoli consist of two types of alveolar cell and an alveolar macrophage
An alveolar macrophage, pulmonary macrophage, (or dust cell, or dust eater) is a type of macrophage, a phagocytosis#Professional phagocytic cells, professional phagocyte, found in the airways and at the level of the pulmonary alveolus, alveoli in ...
. The two types of cell are known as type I and type II cellssquamous
Epithelium or epithelial tissue is a thin, continuous, protective layer of cells with little extracellular matrix. An example is the epidermis, the outermost layer of the skin. Epithelial ( mesothelial) tissues line the outer surfaces of man ...
"), and Type II cells generally cluster in the corners of the alveoli and have a cuboidal shape.alveolar macrophage
An alveolar macrophage, pulmonary macrophage, (or dust cell, or dust eater) is a type of macrophage, a phagocytosis#Professional phagocytic cells, professional phagocyte, found in the airways and at the level of the pulmonary alveolus, alveoli in ...
s have an important role in the immune system
The immune system is a network of biological systems that protects an organism from diseases. It detects and responds to a wide variety of pathogens, from viruses to bacteria, as well as Tumor immunology, cancer cells, Parasitic worm, parasitic ...
. They remove substances which deposit in the alveoli including loose red blood cells that have been forced out from blood vessels.
Microbiota
There is a large presence of microorganism
A microorganism, or microbe, is an organism of microscopic scale, microscopic size, which may exist in its unicellular organism, single-celled form or as a Colony (biology)#Microbial colonies, colony of cells. The possible existence of unseen ...
s in the lungs known as the lung microbiota that interacts with the airway epithelial cells; an interaction of probable importance in maintaining homeostasis. The microbiota is complex and dynamic in healthy people, and altered in diseases such as asthma
Asthma is a common long-term inflammatory disease of the airways of the lungs. It is characterized by variable and recurring symptoms, reversible airflow obstruction, and easily triggered bronchospasms. Symptoms include episodes of wh ...
and COPD. For example significant changes can take place in COPD following infection with rhinovirus
The rhinovirus (from the "nose", , romanized: "of the nose", and the ) is a Positive-sense single stranded RNA virus, positive-sense, single-stranded RNA virus belonging to the genus ''Enterovirus'' in the family ''Picornaviridae''. Rhinoviru ...
.Fungal
A fungus (: fungi , , , or ; or funguses) is any member of the group of eukaryotic organisms that includes microorganisms such as yeasts and molds, as well as the more familiar mushrooms. These organisms are classified as one of the tradit ...
genera
Genus (; : genera ) is a taxonomic rank above species and below family as used in the biological classification of living and fossil organisms as well as viruses. In binomial nomenclature, the genus name forms the first part of the binomial s ...
that are commonly found as mycobiota in the microbiota include '' Candida'', '' Malassezia'', '' Saccharomyces'', and ''Aspergillus
' () is a genus consisting of several hundred mold species found in various climates worldwide.
''Aspergillus'' was first catalogued in 1729 by the Italian priest and biologist Pier Antonio Micheli. Viewing the fungi under a microscope, Miche ...
''.
Respiratory tract
The lower respiratory tract is part of the respiratory system
The respiratory system (also respiratory apparatus, ventilatory system) is a biological system consisting of specific organs and structures used for gas exchange in animals and plants. The anatomy and physiology that make this happen varies grea ...
, and consists of the trachea
The trachea (: tracheae or tracheas), also known as the windpipe, is a cartilaginous tube that connects the larynx to the bronchi of the lungs, allowing the passage of air, and so is present in almost all animals' lungs. The trachea extends from ...
and the structures below this including the lungs.pharynx
The pharynx (: pharynges) is the part of the throat behind the human mouth, mouth and nasal cavity, and above the esophagus and trachea (the tubes going down to the stomach and the lungs respectively). It is found in vertebrates and invertebrates ...
and travels down to a place where it splits (the carina) into a right and left primary bronchus. These supply air to the right and left lungs, splitting progressively into the secondary and tertiary bronchi for the lobes of the lungs, and into smaller and smaller bronchioles until they become the respiratory bronchioles. These in turn supply air through alveolar ducts into the alveoli, where the exchange of gases take place.cilia
The cilium (: cilia; ; in Medieval Latin and in anatomy, ''cilium'') is a short hair-like membrane protrusion from many types of eukaryotic cell. (Cilia are absent in bacteria and archaea.) The cilium has the shape of a slender threadlike proj ...
on the respiratory epithelium lining the passageways,
Blood supply
The lungs have a dual blood supply provided by a bronchial
A bronchus ( ; : bronchi, ) is a passage or airway in the lower respiratory tract that conducts Atmosphere of Earth, air into the lungs. The first or primary bronchi to branch from the trachea at the Carina of trachea, carina are the right main b ...
and a pulmonary circulation.aorta
The aorta ( ; : aortas or aortae) is the main and largest artery in the human body, originating from the Ventricle (heart), left ventricle of the heart, branching upwards immediately after, and extending down to the abdomen, where it splits at ...
. There are usually three arteries, two to the left lung and one to the right, and they branch alongside the bronchi and bronchioles.
Nerve supply
The lungs are supplied by nerves of the autonomic nervous system. Input from the parasympathetic nervous system
The parasympathetic nervous system (PSNS) is one of the three divisions of the autonomic nervous system, the others being the sympathetic nervous system and the enteric nervous system.
The autonomic nervous system is responsible for regulat ...
occurs via the vagus nerve
The vagus nerve, also known as the tenth cranial nerve (CN X), plays a crucial role in the autonomic nervous system, which is responsible for regulating involuntary functions within the human body. This nerve carries both sensory and motor fibe ...
.acetylcholine
Acetylcholine (ACh) is an organic compound that functions in the brain and body of many types of animals (including humans) as a neurotransmitter. Its name is derived from its chemical structure: it is an ester of acetic acid and choline. Par ...
, this causes constriction of the smooth muscle lining the bronchus and bronchioles, and increases the secretions from glands.norepinephrine
Norepinephrine (NE), also called noradrenaline (NA) or noradrenalin, is an organic compound, organic chemical in the catecholamine family that functions in the brain and human body, body as a hormone, neurotransmitter and neuromodulator. The ...
acting on the beta 2 adrenoceptors in the respiratory tract, which causes bronchodilation.respiratory center
The respiratory center is located in the medulla oblongata and pons, in the brainstem. The respiratory center is made up of three major respiratory groups of neurons, two in the medulla and one in the pons. In the medulla they are the dorsal ...
in the brainstem
The brainstem (or brain stem) is the posterior stalk-like part of the brain that connects the cerebrum with the spinal cord. In the human brain the brainstem is composed of the midbrain, the pons, and the medulla oblongata. The midbrain is conti ...
, along the phrenic nerve from the cervical plexus to the diaphragm.
Variation
The lobes of the lung are subject to anatomical variations.
Development
The development of the human lungs arise from the laryngotracheal groove and develop to maturity over several weeks in the foetus and for several years following birth.larynx
The larynx (), commonly called the voice box, is an organ (anatomy), organ in the top of the neck involved in breathing, producing sound and protecting the trachea against food aspiration. The opening of larynx into pharynx known as the laryngeal ...
, trachea
The trachea (: tracheae or tracheas), also known as the windpipe, is a cartilaginous tube that connects the larynx to the bronchi of the lungs, allowing the passage of air, and so is present in almost all animals' lungs. The trachea extends from ...
, bronchi and lungs that make up the respiratory tract, begin to form during the fourth week of embryogenesis
An embryo ( ) is the initial stage of development for a multicellular organism. In organisms that reproduce sexually, embryonic development is the part of the life cycle that begins just after fertilization of the female egg cell by the male ...
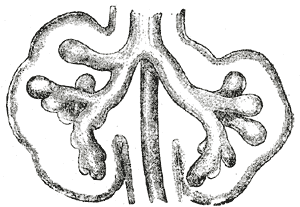 The respiratory tract has a branching structure, and is also known as the respiratory tree.
The respiratory tract has a branching structure, and is also known as the respiratory tree.surface tension
Surface tension is the tendency of liquid surfaces at rest to shrink into the minimum surface area possible. Surface tension (physics), tension is what allows objects with a higher density than water such as razor blades and insects (e.g. Ge ...
at the air-alveolar surface which allows expansion of the alveolar sacs. The alveolar sacs contain the primitive alveoli that form at the end of the alveolar ducts,
and their appearance around the seventh month marks the point at which limited respiration would be possible, and the premature baby could survive.[
]
Vitamin A deficiency
The developing lung is particularly vulnerable to changes in the levels of vitamin A
Vitamin A is a fat-soluble vitamin that is an essential nutrient. The term "vitamin A" encompasses a group of chemically related organic compounds that includes retinol, retinyl esters, and several provitamin (precursor) carotenoids, most not ...
. Vitamin A deficiency has been linked to changes in the epithelial lining of the lung and in the lung parenchyma. This can disrupt the normal physiology of the lung and predispose to respiratory diseases. Severe nutritional deficiency in vitamin A results in a reduction in the formation of the alveolar walls (septa) and to notable changes in the respiratory epithelium; alterations are noted in the extracellular matrix and in the protein content of the basement membrane. The extracellular matrix maintains lung elasticity; the basement membrane is associated with alveolar epithelium and is important in the blood-air barrier. The deficiency is associated with functional defects and disease states. Vitamin A is crucial in the development of the alveoli which continues for several years after birth.
After birth
At birth
Birth is the act or process of bearing or bringing forth offspring, also referred to in technical contexts as parturition. In mammals, the process is initiated by hormones which cause the muscular walls of the uterus to contract, expelling the f ...
, the baby's lungs are filled with fluid secreted by the lungs and are not inflated. After birth the infant's central nervous system
The central nervous system (CNS) is the part of the nervous system consisting primarily of the brain, spinal cord and retina. The CNS is so named because the brain integrates the received information and coordinates and influences the activity o ...
reacts to the sudden change in temperature and environment. This triggers the first breath, within about ten seconds after delivery.
Function
Gas exchange
The major function of the lungs is gas exchange between the lungs and the blood. The alveolar and pulmonary capillary gases equilibrate across the thin blood–air barrier.
Protection
The lungs possess several characteristics which protect against infection. The respiratory tract is lined by respiratory epithelium or respiratory mucosa, with hair-like projections called cilia
The cilium (: cilia; ; in Medieval Latin and in anatomy, ''cilium'') is a short hair-like membrane protrusion from many types of eukaryotic cell. (Cilia are absent in bacteria and archaea.) The cilium has the shape of a slender threadlike proj ...
that beat rhythmically and carry mucus. This mucociliary clearance is an important defence system against air-borne infection.[ The dust particles and bacteria in the inhaled air are caught in the mucosal surface of the airways, and are moved up towards the pharynx by the rhythmic upward beating action of the cilia.]defensin
Defensins are small cysteine-rich cationic proteins across cellular life, including vertebrate and invertebrate animals, plants, and fungi. They are host defense peptides, with members displaying either direct Antimicrobial, antimicrobial activit ...
s, antiproteases, and antioxidants.macrophage
Macrophages (; abbreviated MPhi, φ, MΦ or MP) are a type of white blood cell of the innate immune system that engulf and digest pathogens, such as cancer cells, microbes, cellular debris and foreign substances, which do not have proteins that ...
s, immune cells which engulf and destroy debris and microbes that enter the lung in a process known as phagocytosis
Phagocytosis () is the process by which a cell (biology), cell uses its plasma membrane to engulf a large particle (≥ 0.5 μm), giving rise to an internal compartment called the phagosome. It is one type of endocytosis. A cell that performs ph ...
; and dendritic cells which present antigens to activate components of the adaptive immune system
The adaptive immune system (AIS), also known as the acquired immune system, or specific immune system is a subsystem of the immune system that is composed of specialized cells, organs, and processes that eliminate pathogens specifically. The ac ...
such as T cell
T cells (also known as T lymphocytes) are an important part of the immune system and play a central role in the adaptive immune response. T cells can be distinguished from other lymphocytes by the presence of a T-cell receptor (TCR) on their cell ...
s and B cells.mouth
A mouth also referred to as the oral is the body orifice through which many animals ingest food and animal communication#Auditory, vocalize. The body cavity immediately behind the mouth opening, known as the oral cavity (or in Latin), is also t ...
and behind the mouth in the oropharynx, and larger particles are trapped in nasal hair after inhalation.
Other
In addition to their function in respiration, the lungs have a number of other functions. They are involved in maintaining homeostasis
In biology, homeostasis (British English, British also homoeostasis; ) is the state of steady internal physics, physical and chemistry, chemical conditions maintained by organism, living systems. This is the condition of optimal functioning fo ...
, helping in the regulation of blood pressure
Blood pressure (BP) is the pressure of Circulatory system, circulating blood against the walls of blood vessels. Most of this pressure results from the heart pumping blood through the circulatory system. When used without qualification, the term ...
as part of the renin–angiotensin system
The renin–angiotensin system (RAS), or renin–angiotensin–aldosterone system (RAAS), is a hormone system that regulates blood pressure, fluid, and electrolyte balance, and systemic vascular resistance.
When renal blood flow is reduced, ...
. The inner lining of the blood vessels secretes angiotensin-converting enzyme
Angiotensin-converting enzyme (), or ACE, is a central component of the renin–angiotensin system (RAS), which controls blood pressure by regulating the volume of fluids in the body. It converts the hormone angiotensin I to the active vasocon ...
(ACE) an enzyme
An enzyme () is a protein that acts as a biological catalyst by accelerating chemical reactions. The molecules upon which enzymes may act are called substrate (chemistry), substrates, and the enzyme converts the substrates into different mol ...
that catalyses the conversion of angiotensin I to angiotensin II
Angiotensin is a peptide hormone that causes vasoconstriction and an increase in blood pressure. It is part of the renin–angiotensin system, which regulates blood pressure. Angiotensin also stimulates the release of aldosterone from the ...
.carbon dioxide
Carbon dioxide is a chemical compound with the chemical formula . It is made up of molecules that each have one carbon atom covalent bond, covalently double bonded to two oxygen atoms. It is found in a gas state at room temperature and at norma ...
when breathing.stroke
Stroke is a medical condition in which poor cerebral circulation, blood flow to a part of the brain causes cell death. There are two main types of stroke: brain ischemia, ischemic, due to lack of blood flow, and intracranial hemorrhage, hemor ...
s.speech
Speech is the use of the human voice as a medium for language. Spoken language combines vowel and consonant sounds to form units of meaning like words, which belong to a language's lexicon. There are many different intentional speech acts, suc ...
by providing air and airflow for the creation of vocal sounds,paralanguage
Paralanguage, also known as vocalics, is a component of meta-communication that may modify meaning, give nuanced meaning, or convey emotion, by using suprasegmental techniques such as prosody, pitch, volume, intonation, etc. It is sometimes d ...
communications such as sighs and gasps.
Research suggests a role of the lungs in the production of blood platelets.
Gene and protein expression
About 20,000 protein coding genes are expressed in human cells and almost 75% of these genes are expressed in the normal lung. A little less than 200 of these genes are more specifically expressed in the lung with less than 20 genes being highly lung specific. The highest expression of lung specific proteins are different surfactant
Surfactants are chemical compounds that decrease the surface tension or interfacial tension between two liquids, a liquid and a gas, or a liquid and a solid. The word ''surfactant'' is a Blend word, blend of "surface-active agent",
coined in ...
proteins,[ such as SFTPA1, SFTPB and SFTPC, and napsin, expressed in type II pneumocytes. Other proteins with elevated expression in the lung are the dynein protein DNAH5 in ciliated cells, and the secreted SCGB1A1 protein in mucus-secreting ]goblet cell
Goblet cells are simple columnar epithelial cells that secrete gel-forming mucins, like mucin 2 in the lower gastrointestinal tract, and mucin 5AC in the respiratory tract. The goblet cells mainly use the merocrine method of secretion, secre ...
s of the airway mucosa.
Clinical significance
Lungs can be affected by a number of diseases and disorders. Pulmonology
Pulmonology (, , from Latin ''pulmō, -ōnis'' "lung" and the Greek suffix "study of"), pneumology (, built on Greek πνεύμων "lung") or pneumonology () is a medical specialty that deals with diseases involving the respiratory tract. ...
is the medical speciality that deals with respiratory diseases involving the lungs and respiratory system
The respiratory system (also respiratory apparatus, ventilatory system) is a biological system consisting of specific organs and structures used for gas exchange in animals and plants. The anatomy and physiology that make this happen varies grea ...
.surgery
Surgery is a medical specialty that uses manual and instrumental techniques to diagnose or treat pathological conditions (e.g., trauma, disease, injury, malignancy), to alter bodily functions (e.g., malabsorption created by bariatric surgery s ...
of the lungs including lung volume reduction surgery, lobectomy, pneumectomy and lung transplantation.
Inflammation and infection
Inflammatory conditions of the lung tissue are pneumonia, of the respiratory tract are bronchitis
Bronchitis is inflammation of the bronchi (large and medium-sized airways) in the lungs that causes coughing. Bronchitis usually begins as an infection in the nose, ears, throat, or sinuses. The infection then makes its way down to the bronchi. ...
and bronchiolitis, and of the pleurae surrounding the lungs pleurisy
Pleurisy, also known as pleuritis, is inflammation of the membranes that surround the lungs and line the chest cavity (Pulmonary pleurae, pleurae). This can result in a sharp chest pain while breathing. Occasionally the pain may be a constant d ...
. Inflammation is usually caused by infection
An infection is the invasion of tissue (biology), tissues by pathogens, their multiplication, and the reaction of host (biology), host tissues to the infectious agent and the toxins they produce. An infectious disease, also known as a transmis ...
s due to bacteria
Bacteria (; : bacterium) are ubiquitous, mostly free-living organisms often consisting of one Cell (biology), biological cell. They constitute a large domain (biology), domain of Prokaryote, prokaryotic microorganisms. Typically a few micr ...
or virus
A virus is a submicroscopic infectious agent that replicates only inside the living Cell (biology), cells of an organism. Viruses infect all life forms, from animals and plants to microorganisms, including bacteria and archaea. Viruses are ...
es. When the lung tissue is inflamed due to other causes it is called pneumonitis. One major cause of bacterial pneumonia is tuberculosis
Tuberculosis (TB), also known colloquially as the "white death", or historically as consumption, is a contagious disease usually caused by ''Mycobacterium tuberculosis'' (MTB) bacteria. Tuberculosis generally affects the lungs, but it can al ...
.immunodeficiency
Immunodeficiency, also known as immunocompromise, is a state in which the immune system's ability to fight infectious diseases and cancer is compromised or entirely absent. Most cases are acquired ("secondary") due to extrinsic factors that aff ...
and can include a fungal infection by '' Aspergillus fumigatus'' that can lead to an aspergilloma forming in the lung.cilia
The cilium (: cilia; ; in Medieval Latin and in anatomy, ''cilium'') is a short hair-like membrane protrusion from many types of eukaryotic cell. (Cilia are absent in bacteria and archaea.) The cilium has the shape of a slender threadlike proj ...
in the respiratory epithelium. However, chronic exposure has the effect of desensitising the ciliary response which reduces mucociliary clearance (MCC). MCC is an innate defense system protecting against pollutants and pathogens, and when this is disrupted the numbers of alveolar macrophage
An alveolar macrophage, pulmonary macrophage, (or dust cell, or dust eater) is a type of macrophage, a phagocytosis#Professional phagocytic cells, professional phagocyte, found in the airways and at the level of the pulmonary alveolus, alveoli in ...
s are decreased. A subsequent inflammatory response is the release of cytokine
Cytokines () are a broad and loose category of small proteins (~5–25 kDa) important in cell signaling.
Cytokines are produced by a broad range of cells, including immune cells like macrophages, B cell, B lymphocytes, T cell, T lymphocytes ...
s. Another consequence is the susceptibility to infection.
Blood-supply changes
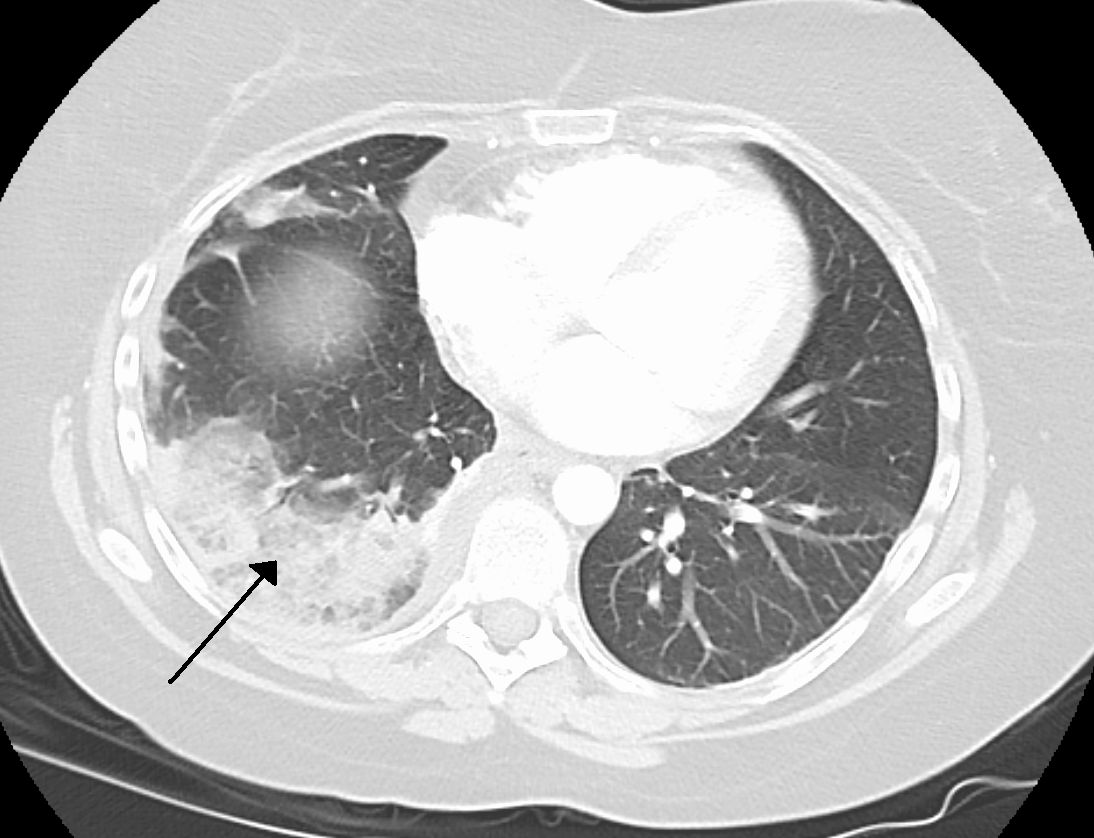 A pulmonary embolism is a blood clot that becomes lodged in the pulmonary arteries. The majority of emboli arise because of deep vein thrombosis in the legs. Pulmonary emboli may be investigated using a ventilation/perfusion scan, a CT scan of the arteries of the lung, or blood tests such as the D-dimer.
A pulmonary embolism is a blood clot that becomes lodged in the pulmonary arteries. The majority of emboli arise because of deep vein thrombosis in the legs. Pulmonary emboli may be investigated using a ventilation/perfusion scan, a CT scan of the arteries of the lung, or blood tests such as the D-dimer.chest X-ray
A chest radiograph, chest X-ray (CXR), or chest film is a Projectional radiography, projection radiograph of the chest used to diagnose conditions affecting the chest, its contents, and nearby structures. Chest radiographs are the most common fi ...
or CT scan
A computed tomography scan (CT scan), formerly called computed axial tomography scan (CAT scan), is a medical imaging technique used to obtain detailed internal images of the body. The personnel that perform CT scans are called radiographers or ...
, and may require the insertion of a surgical drain until the underlying cause is identified and treated.
Obstructive lung diseases
Asthma
Asthma is a common long-term inflammatory disease of the airways of the lungs. It is characterized by variable and recurring symptoms, reversible airflow obstruction, and easily triggered bronchospasms. Symptoms include episodes of wh ...
, bronchiectasis, and chronic obstructive pulmonary disease (COPD) that includes chronic bronchitis, and emphysema, are all obstructive lung diseases characterised by airway obstruction. This limits the amount of air that is able to enter alveoli because of constriction of the bronchial tree, due to inflammation. Obstructive lung diseases are often identified because of symptoms and diagnosed with pulmonary function tests such as spirometry.
Many obstructive lung diseases are managed by avoiding triggers (such as dust mites or smoking
Smoking is a practice in which a substance is combusted, and the resulting smoke is typically inhaled to be tasted and absorbed into the bloodstream of a person. Most commonly, the substance used is the dried leaves of the tobacco plant, whi ...
), with symptom control such as bronchodilators, and with suppression of inflammation (such as through corticosteroid
Corticosteroids are a class of steroid hormones that are produced in the adrenal cortex of vertebrates, as well as the synthetic analogues of these hormones. Two main classes of corticosteroids, glucocorticoids and mineralocorticoids, are invo ...
s) in severe cases. A common cause of chronic bronchitis, and emphysema, is smoking; and common causes of bronchiectasis include severe infections and cystic fibrosis
Cystic fibrosis (CF) is a genetic disorder inherited in an autosomal recessive manner that impairs the normal clearance of Sputum, mucus from the lungs, which facilitates the colonization and infection of the lungs by bacteria, notably ''Staphy ...
. The definitive cause of asthma
Asthma is a common long-term inflammatory disease of the airways of the lungs. It is characterized by variable and recurring symptoms, reversible airflow obstruction, and easily triggered bronchospasms. Symptoms include episodes of wh ...
is not yet known, but it has been linked to other atopic diseases.elastin
Elastin is a protein encoded by the ''ELN'' gene in humans and several other animals. Elastin is a key component in the extracellular matrix of gnathostomes (jawed vertebrates). It is highly Elasticity (physics), elastic and present in connective ...
in the lung's connective tissue that can also result in emphysema. Elastase is inhibited by the acute-phase protein
Acute-phase proteins (APPs) are a class of proteins whose concentrations in blood plasma either increase (positive acute-phase proteins) or decrease (negative acute-phase proteins) in response to inflammation. This response is called the ''acute-p ...
, alpha-1 antitrypsin, and when there is a deficiency in this, emphysema can develop. With persistent stress from smoking, the airway basal cells become disarranged and lose their regenerative ability needed to repair the epithelial barrier. The disorganised basal cells are seen to be responsible for the major airway changes that are characteristic of COPD, and with continued stress can undergo a malignant transformation. Studies have shown that the initial development of emphysema is centred on the early changes in the airway epithelium of the small airways.
Restrictive lung diseases
Some types of chronic lung diseases are classified as restrictive lung disease, because of a restriction in the amount of lung tissue involved in respiration. These include pulmonary fibrosis which can occur when the lung is inflamed for a long period of time. Fibrosis in the lung replaces functioning lung tissue with fibrous connective tissue. This can be due to a large variety of occupational lung diseases such as Coalworker's pneumoconiosis, autoimmune diseases or more rarely to a reaction to medication
Medication (also called medicament, medicine, pharmaceutical drug, medicinal product, medicinal drug or simply drug) is a drug used to medical diagnosis, diagnose, cure, treat, or preventive medicine, prevent disease. Drug therapy (pharmaco ...
.mechanical ventilation
Mechanical ventilation or assisted ventilation is the Medicine, medical term for using a ventilator, ventilator machine to fully or partially provide artificial ventilation. Mechanical ventilation helps move air into and out of the lungs, wit ...
to ensure an adequate supply of air.
Cancers
Lung cancer can either arise directly from lung tissue or as a result of metastasis
Metastasis is a pathogenic agent's spreading from an initial or primary site to a different or secondary site within the host's body; the term is typically used when referring to metastasis by a cancerous tumor. The newly pathological sites, ...
from another part of the body. There are two main types of primary tumour described as either small-cell or non-small-cell lung carcinomas. The major risk factor for cancer is smoking
Smoking is a practice in which a substance is combusted, and the resulting smoke is typically inhaled to be tasted and absorbed into the bloodstream of a person. Most commonly, the substance used is the dried leaves of the tobacco plant, whi ...
. Once a cancer is identified it is staged using scans such as a CT scan
A computed tomography scan (CT scan), formerly called computed axial tomography scan (CAT scan), is a medical imaging technique used to obtain detailed internal images of the body. The personnel that perform CT scans are called radiographers or ...
and a sample of tissue from a biopsy is taken. Cancers may be treated surgically by removing the tumour, the use of radiotherapy
Radiation therapy or radiotherapy (RT, RTx, or XRT) is a treatment using ionizing radiation, generally provided as part of cancer therapy to either kill or control the growth of malignant cells. It is normally delivered by a linear particle ...
, chemotherapy
Chemotherapy (often abbreviated chemo, sometimes CTX and CTx) is the type of cancer treatment that uses one or more anti-cancer drugs (list of chemotherapeutic agents, chemotherapeutic agents or alkylating agents) in a standard chemotherapy re ...
or a combination, or with the aim of symptom control.
Congenital disorders
Congenital disorders include cystic fibrosis
Cystic fibrosis (CF) is a genetic disorder inherited in an autosomal recessive manner that impairs the normal clearance of Sputum, mucus from the lungs, which facilitates the colonization and infection of the lungs by bacteria, notably ''Staphy ...
, pulmonary hypoplasia (an incomplete development of the lungs)
Pleural space pressure
A pneumothorax (collapsed lung) is an abnormal collection of air in the pleural space that causes an uncoupling of the lung from the chest wall.
Examination
As part of a physical examination
In a physical examination, medical examination, clinical examination, or medical checkup, a medical practitioner examines a patient for any possible medical signs or symptoms of a Disease, medical condition. It generally consists of a series of ...
in response to respiratory symptoms of shortness of breath
Shortness of breath (SOB), known as dyspnea (in AmE) or dyspnoea (in BrE), is an uncomfortable feeling of not being able to breathe well enough. The American Thoracic Society defines it as "a subjective experience of breathing discomfort that con ...
, and cough
A cough is a sudden expulsion of air through the large breathing passages which can help clear them of fluids, irritants, foreign particles and Microorganism, microbes. As a protective reflex, coughing can be repetitive with the cough reflex fol ...
, a lung examination may be carried out. This exam includes palpation and auscultation
Auscultation (based on the Latin verb ''auscultare'' "to listen") is listening to the internal sounds of the body, usually using a stethoscope. Auscultation is performed for the purposes of examining the circulatory system, circulatory and resp ...
. The areas of the lungs that can be listened to using a stethoscope are called the lung fields, and these are the posterior, lateral, and anterior lung fields. The posterior fields can be listened to from the back and include: the lower lobes (taking up three quarters of the posterior fields); the anterior fields taking up the other quarter; and the lateral fields under the axilla
The axilla (: axillae or axillas; also known as the armpit, underarm or oxter) is the area on the human body directly under the shoulder joint. It includes the axillary space, an anatomical space within the shoulder girdle between the arm a ...
e, the left axilla for the lingual, the right axilla for the middle right lobe. The anterior fields can also be auscultated from the front. An area known as the triangle of auscultation is an area of thinner musculature on the back which allows improved listening.asthma
Asthma is a common long-term inflammatory disease of the airways of the lungs. It is characterized by variable and recurring symptoms, reversible airflow obstruction, and easily triggered bronchospasms. Symptoms include episodes of wh ...
and COPD.
Function testing
Lung function testing is carried out by evaluating a person's capacity to inhale and exhale in different circumstances.
Culinary uses
Mammal lung is one of the main types of offal, or pluck, alongside the heart
The heart is a muscular Organ (biology), organ found in humans and other animals. This organ pumps blood through the blood vessels. The heart and blood vessels together make the circulatory system. The pumped blood carries oxygen and nutrie ...
and trachea
The trachea (: tracheae or tracheas), also known as the windpipe, is a cartilaginous tube that connects the larynx to the bronchi of the lungs, allowing the passage of air, and so is present in almost all animals' lungs. The trachea extends from ...
, and is consumed as a foodstuff around the world in dishes such as Scottish haggis
Haggis ( ) is a savoury pudding containing sheep's offal, pluck (heart, liver, and lungs), Mincing, minced with chopped onion, oatmeal, suet, spices, and salt, mixed with Stock (food), stock, and cooked while traditionally encased in the anima ...
. The United States Food and Drug Administration
The United States Food and Drug Administration (FDA or US FDA) is a List of United States federal agencies, federal agency of the United States Department of Health and Human Services, Department of Health and Human Services. The FDA is respo ...
legally prohibits the sale of animal lungs due to concerns such as fungal spores or cross-contamination with other organs, although this has been criticised as unfounded.[Davies, Madeline]
"Here’s Why It’s Illegal to Sell Animal Lungs for Consumption in the U.S."
'' Eater'', 10 November 2021. Retrieved 26 January 2023.
Other animals
Birds
 The lungs of birds are relatively small, but are connected to eight or nine air sacs that extend through much of the body, and are in turn connected to air spaces within the bones. On inhalation, air travels through the trachea of a bird into the air sacs. Air then travels continuously from the air sacs at the back, through the lungs, which are relatively fixed in size, to the air sacs at the front. From here, the air is exhaled. These fixed size lungs are called "circulatory lungs", as distinct from the "bellows-type lungs" found in most other animals.
The lungs of birds are relatively small, but are connected to eight or nine air sacs that extend through much of the body, and are in turn connected to air spaces within the bones. On inhalation, air travels through the trachea of a bird into the air sacs. Air then travels continuously from the air sacs at the back, through the lungs, which are relatively fixed in size, to the air sacs at the front. From here, the air is exhaled. These fixed size lungs are called "circulatory lungs", as distinct from the "bellows-type lungs" found in most other animals.
Reptiles
The lungs of most reptiles have a single bronchus running down the centre, from which numerous branches reach out to individual pockets throughout the lungs. These pockets are similar to alveoli in mammals, but much larger and fewer in number. These give the lung a sponge-like texture. In tuatara
The tuatara (''Sphenodon punctatus'') is a species of reptile endemic to New Zealand. Despite its close resemblance to lizards, it is actually the only extant member of a distinct lineage, the previously highly diverse order Rhynchocephal ...
s, snake
Snakes are elongated limbless reptiles of the suborder Serpentes (). Cladistically squamates, snakes are ectothermic, amniote vertebrates covered in overlapping scales much like other members of the group. Many species of snakes have s ...
s, and some lizard
Lizard is the common name used for all Squamata, squamate reptiles other than snakes (and to a lesser extent amphisbaenians), encompassing over 7,000 species, ranging across all continents except Antarctica, as well as most Island#Oceanic isla ...
s, the lungs are simpler in structure, similar to that of typical amphibians.crocodilians
Crocodilia () is an order of semiaquatic, predatory reptiles that are known as crocodilians. They first appeared during the Late Cretaceous and are the closest living relatives of birds. Crocodilians are a type of crocodylomorph pseudosuchi ...
and monitor lizards have lungs similar to those of birds, providing a unidirectional airflow and even possessing air sacs. The now extinct pterosaurs
Pterosaurs are an extinct clade of flying reptiles in the Order (biology), order Pterosauria. They existed during most of the Mesozoic: from the Late Triassic to the end of the Cretaceous (228 million to 66 million years ago). Pterosau ...
have seemingly even further refined this type of lung, extending the airsacs into the wing membranes and, in the case of lonchodectids, '' Tupuxuara'', and azhdarchoids, the hindlimbs.
Reptilian lungs typically receive air via expansion and contraction of the ribs driven by axial muscles and buccal pumping. Crocodilian
Crocodilia () is an Order (biology), order of semiaquatic, predatory reptiles that are known as crocodilians. They first appeared during the Late Cretaceous and are the closest living relatives of birds. Crocodilians are a type of crocodylomorp ...
s also rely on the hepatic piston method, in which the liver is pulled back by a muscle anchored to the pubic bone (part of the pelvis) called the diaphragmaticus,Boyle's law
Boyle's law, also referred to as the Boyle–Mariotte law or Mariotte's law (especially in France), is an empirical gas laws, gas law that describes the relationship between pressure and volume of a confined gas. Boyle's law has been stated as:
...
. Turtle
Turtles are reptiles of the order (biology), order Testudines, characterized by a special turtle shell, shell developed mainly from their ribs. Modern turtles are divided into two major groups, the Pleurodira (side necked turtles) and Crypt ...
s, which are unable to move their ribs, instead use their forelimbs and pectoral girdle to force air in and out of the lungs.
Amphibians
 The lungs of most
The lungs of most frog
A frog is any member of a diverse and largely semiaquatic group of short-bodied, tailless amphibian vertebrates composing the order (biology), order Anura (coming from the Ancient Greek , literally 'without tail'). Frog species with rough ski ...
s and other amphibian
Amphibians are ectothermic, anamniote, anamniotic, tetrapod, four-limbed vertebrate animals that constitute the class (biology), class Amphibia. In its broadest sense, it is a paraphyletic group encompassing all Tetrapod, tetrapods, but excl ...
s are simple and balloon-like, with gas exchange limited to the outer surface of the lung. This is not very efficient, but amphibians have low metabolic demands and can also quickly dispose of carbon dioxide by diffusion across their skin in water, and supplement their oxygen supply by the same method. Amphibians employ a positive pressure system to get air to their lungs, forcing air down into the lungs by buccal pumping. This is distinct from most higher vertebrates, who use a breathing system driven by negative pressure where the lungs are inflated by expanding the rib cage.tetrapod
A tetrapod (; from Ancient Greek :wiktionary:τετρα-#Ancient Greek, τετρα- ''(tetra-)'' 'four' and :wiktionary:πούς#Ancient Greek, πούς ''(poús)'' 'foot') is any four-Limb (anatomy), limbed vertebrate animal of the clade Tetr ...
s are amphibians. The majority of salamander species are lungless salamanders, which respirate through their skin and tissues lining their mouth. This necessarily restricts their size: all are small and rather thread-like in appearance, maximising skin surface relative to body volume.caecilian
Caecilians (; ) are a group of limbless, vermiform (worm-shaped) or serpentine (snake-shaped) amphibians with small or sometimes nonexistent eyes. They mostly live hidden in soil or in streambeds, and this cryptic lifestyle renders caecilians ...
.
The lungs of amphibians typically have a few narrow internal walls ( septa) of soft tissue around the outer walls, increasing the respiratory surface area and giving the lung a honeycomb appearance. In some salamanders, even these are lacking, and the lung has a smooth wall. In caecilians, as in snakes, only the right lung attains any size or development.
Fish
Lungs are found in three groups of fish; the coelacanths, the bichirs and the lungfish. Like in tetrapods, but unlike fish with swim bladder, the opening is at the ventral side of the oesophagus. The coelacanth has a nonfunctional and unpaired vestigial lung surrounded by a fatty organ. Bichirs, the only group of Actinopterygii, ray-finned fish with lungs, have a pair which are hollow unchambered sacs, where the gas-exchange occurs on very flat folds that increase their inner surface area. The lungs of lungfish show more resemblance to tetrapod lungs. There is an elaborate network of parenchymal septa, dividing them into numerous respiration chambers. In the Australian lungfish, there is only a single lung, albeit divided into two lobes. Other lungfish, however, have traditionally been considered having two lungs, but newer research defines paired lungs as bilateral lung buds that arise simultaneously and are both connected directly to the foregut, which is only seen in tetrapods. In all lungfish, including the Australian, the lungs are located in the upper dorsal part of the body, with the connecting duct curving around and above the oesophagus. The blood supply also twists around the oesophagus, suggesting that the lungs originally evolved in the ventral part of the body, as in other vertebrates.
Invertebrates
 A number of invertebrates have lung-like structures that serve a similar respiratory purpose to true vertebrate lungs, but are not evolutionarily related and only arise out of convergent evolution. Some arachnids, such as spiders and scorpions, have structures called book lungs used for atmospheric gas exchange. Some species of spider have four pairs of book lungs but most have two pairs. Scorpions have Spiracle (arthropods), spiracles on their body for the entrance of air to the book lungs.
The coconut crab is terrestrial and uses structures called branchiostegal lungs to breathe air.
A number of invertebrates have lung-like structures that serve a similar respiratory purpose to true vertebrate lungs, but are not evolutionarily related and only arise out of convergent evolution. Some arachnids, such as spiders and scorpions, have structures called book lungs used for atmospheric gas exchange. Some species of spider have four pairs of book lungs but most have two pairs. Scorpions have Spiracle (arthropods), spiracles on their body for the entrance of air to the book lungs.
The coconut crab is terrestrial and uses structures called branchiostegal lungs to breathe air.
Evolutionary origins
The lungs of today's terrestrial vertebrates and the gas bladders of today's fish are believed to have evolved from simple sacs, as outpocketings of the oesophagus
The esophagus (American English), oesophagus (British English), or œsophagus ( archaic spelling) ( see spelling difference) all ; : ((o)e)(œ)sophagi or ((o)e)(œ)sophaguses), colloquially known also as the food pipe, food tube, or gullet, ...
, that allowed early fish to gulp air under oxygen-poor conditions.tetrapod
A tetrapod (; from Ancient Greek :wiktionary:τετρα-#Ancient Greek, τετρα- ''(tetra-)'' 'four' and :wiktionary:πούς#Ancient Greek, πούς ''(poús)'' 'foot') is any four-Limb (anatomy), limbed vertebrate animal of the clade Tetr ...
s. Thus, the lungs of vertebrates are homology (biology), homologous to the gas bladders of fish (but not to their gills).
See also
* Atelectasis
* Drowning
* Interstitial lung disease
* Liquid breathing
* Lung abscess
* Lung-on-a-chip
* Secarecytosis
* List of terms of lung size and activity
* Tobacco
* Vaping
* Smoking
References
Further reading
Dr D.R. Johnson: Introductory anatomy, respiratory system
, leeds.ac.uk
sln.fi.edu
people.eku.edu
External links
Lung at the Human Protein Atlas
{{DEFAULTSORT:Human Lung
Lung,
Human anatomy by organ
Respiratory system anatomy
Articles containing video clips
 In humans, the lungs are located in the chest on either side of the
In humans, the lungs are located in the chest on either side of the  The lungs are part of the lower respiratory tract, and accommodate the bronchial airways when they branch from the trachea. The bronchial airways terminate in alveoli which make up the functional tissue ( parenchyma) of the lung, and veins, arteries, nerves, and
The lungs are part of the lower respiratory tract, and accommodate the bronchial airways when they branch from the trachea. The bronchial airways terminate in alveoli which make up the functional tissue ( parenchyma) of the lung, and veins, arteries, nerves, and 
 The connective tissue of the lungs is made up of
The connective tissue of the lungs is made up of 
 Alveoli consist of two types of alveolar cell and an
Alveoli consist of two types of alveolar cell and an  The respiratory tract has a branching structure, and is also known as the respiratory tree. In the embryo this structure is developed in the process of branching morphogenesis, and is generated by the repeated splitting of the tip of the branch. In the development of the lungs (as in some other organs) the epithelium forms branching tubes. The lung has a left-right symmetry and each bud known as a bronchial bud grows out as a tubular epithelium that becomes a bronchus. Each bronchus branches into bronchioles. The branching is a result of the tip of each tube bifurcating. The branching process forms the bronchi, bronchioles, and ultimately the alveoli. The four genes mostly associated with branching morphogenesis in the lung are the intercellular signalling protein – sonic hedgehog (SHH), fibroblast growth factors FGF10 and FGFR2b, and bone morphogenetic protein BMP4. FGF10 is seen to have the most prominent role. FGF10 is a paracrine signalling molecule needed for epithelial branching, and SHH inhibits FGF10. The development of the alveoli is influenced by a different mechanism whereby continued bifurcation is stopped and the distal tips become dilated to form the alveoli.
At the end of the fourth week, the lung bud divides into two, the right and left primary bronchial buds on each side of the trachea. During the fifth week, the right bud branches into three secondary bronchial buds and the left branches into two secondary bronchial buds. These give rise to the lobes of the lungs, three on the right and two on the left. Over the following week, the secondary buds branch into tertiary buds, about ten on each side. From the sixth week to the sixteenth week, the major elements of the lungs appear except the alveoli. From week 16 to week 26, the bronchi enlarge and lung tissue becomes highly vascularised. Bronchioles and alveolar ducts also develop. By week 26, the terminal bronchioles have formed which branch into two respiratory bronchioles. During the period covering the 26th week until birth the important blood–air barrier is established. Specialised type I alveolar cells where gas exchange will take place, together with the type II alveolar cells that secrete pulmonary surfactant, appear. The surfactant reduces the
The respiratory tract has a branching structure, and is also known as the respiratory tree. In the embryo this structure is developed in the process of branching morphogenesis, and is generated by the repeated splitting of the tip of the branch. In the development of the lungs (as in some other organs) the epithelium forms branching tubes. The lung has a left-right symmetry and each bud known as a bronchial bud grows out as a tubular epithelium that becomes a bronchus. Each bronchus branches into bronchioles. The branching is a result of the tip of each tube bifurcating. The branching process forms the bronchi, bronchioles, and ultimately the alveoli. The four genes mostly associated with branching morphogenesis in the lung are the intercellular signalling protein – sonic hedgehog (SHH), fibroblast growth factors FGF10 and FGFR2b, and bone morphogenetic protein BMP4. FGF10 is seen to have the most prominent role. FGF10 is a paracrine signalling molecule needed for epithelial branching, and SHH inhibits FGF10. The development of the alveoli is influenced by a different mechanism whereby continued bifurcation is stopped and the distal tips become dilated to form the alveoli.
At the end of the fourth week, the lung bud divides into two, the right and left primary bronchial buds on each side of the trachea. During the fifth week, the right bud branches into three secondary bronchial buds and the left branches into two secondary bronchial buds. These give rise to the lobes of the lungs, three on the right and two on the left. Over the following week, the secondary buds branch into tertiary buds, about ten on each side. From the sixth week to the sixteenth week, the major elements of the lungs appear except the alveoli. From week 16 to week 26, the bronchi enlarge and lung tissue becomes highly vascularised. Bronchioles and alveolar ducts also develop. By week 26, the terminal bronchioles have formed which branch into two respiratory bronchioles. During the period covering the 26th week until birth the important blood–air barrier is established. Specialised type I alveolar cells where gas exchange will take place, together with the type II alveolar cells that secrete pulmonary surfactant, appear. The surfactant reduces the  The lungs of most
The lungs of most